Search By Topic
Found 59 Unique Results
Page 1 of 6
Page 1 of 6
Page 1 of 6
Diabetic Ketoacidosis and Necrotizing Soft Tissue Infection
DOI: https://doi.org/10.21980/J89M0KAt the end of this oral board session, examinees will: 1) Demonstrate the ability to obtain a complete medical history and physical exam. 2) Identify and appropriately treat DKA. 3) Identify, treat, and make appropriate consults for NSTI. 4) Demonstrate effective communication of the treatment plan with the patient.
A Case Report of Inferior Rectus Abscess
DOI: https://doi.org/10.21980/J8J35GNon-contrast computed tomography (CT) imaging of the head in coronal, sagittal, and axial planes revealed a distinct 1.7 x 2.2 x 1.4 cm peripherally enhancing fluid collection within the left inferior orbit, involving the inferior rectus (yellow circle). This lesion resulted in restricted extraocular motility due to structural compression of the left globe. Laboratory results showed a mildly elevated white blood cell count of 11.5/mm3 and otherwise normal results including C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR).
A Case Report of Hydropic Gallbladder Presenting as Right Lower Quadrant Abdominal Pain
DOI: https://doi.org/10.21980/J8DD26Computed tomography (CT) of the abdomen and pelvis with contrast was ordered, and general surgery was consulted for the initial working diagnosis of acute appendicitis. However, the CT scan resulted with findings of a markedly distended gallbladder measuring approximately 14.5 x 4 centimeters (cm) with marked gallbladder wall thickening (magenta) and pericholecystic fat stranding (cyan). The appendix was not dilated and had no inflammatory changes or edema. Follow-up right upper quadrant ultrasound confirmed the diagnosis of acute cholecystitis.
Bridging Hospital Resource Variability: Adapting the Escape Room to Integrate Procedure Teaching for Emergency Medicine Trainees in India
DOI: https://doi.org/10.21980/J8CK98By the end of the escape room, learners should be able to: 1) describe the mechanism of action of antiretroviral therapies available in India, 2) prescribe initial antiretroviral therapy to a patient presenting to the emergency department with a new diagnosis of HIV, 3) develop a differential diagnosis for a patient with HIV presenting to the ED with chest pain, 4) identify common dermatologic manifestations of opportunistic infections in patients with HIV, 5) identify computerized tomography scan and lumbar puncture features for central nervous system infections seen in patients with Acquired Immunodeficiency Syndrome (AIDS), 6) identify red flag features and appropriate workup for a patient with HIV presenting with a headache to the ED, 7) interpret images obtained during a Rapid Ultrasound for Shock and Hemorrhage (RUSH) exam, 8) identify cardiac tamponade and perform a pericardiocentesis, and 9) communicate and collaborate as a team to manage a complex, unstable patient with HIV in the ED.
A Man With Chest Pain After An Assault – A Case Report
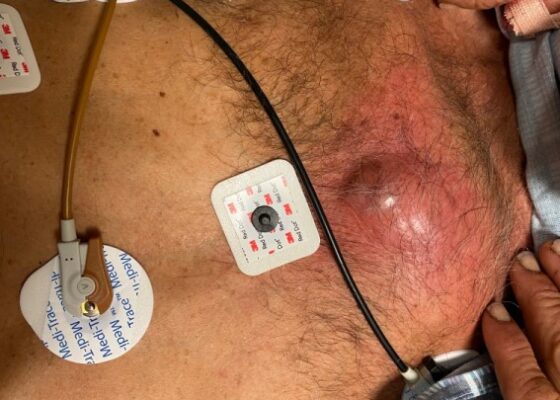
DOI: https://doi.org/10.21980/J8J93SOn exam, we found a suspected chest wall abscess with surrounding erythema (blue arrow). The patient underwent CT of the chest which showed a comminuted displaced midsternal fracture (yellow arrow) with moderate fluid and air anteriorly (red arrow), consistent with an abscess. His laboratory results had no significant abnormalities.
Septic Abortion Complicated by Disseminated Intravascular Coagulation
DOI: https://doi.org/10.21980/J8GH1GAt the conclusion of the simulation session, learners will be able to: 1) Obtain a relevant focused history including pregnancy history, medication use, and past medical history. 2) Develop a differential for fever and vaginal bleeding in a pregnant patient. 3) Discuss management of septic abortion, including empiric broad-spectrum antibiotics and obstetric consultation for source control with dilation and curettage (D&C). 4) Discuss expected laboratory findings of disseminated intravascular coagulation (DIC). 5) Discuss management of DIC, including identification of underlying etiology and supportive resuscitation with blood products. 6) Review the components of blood products. 7) Identify appropriate disposition of the patient to the intensive care unit (ICU).
Septic Arthritis of the Acromioclavicular Joint: A Case Report
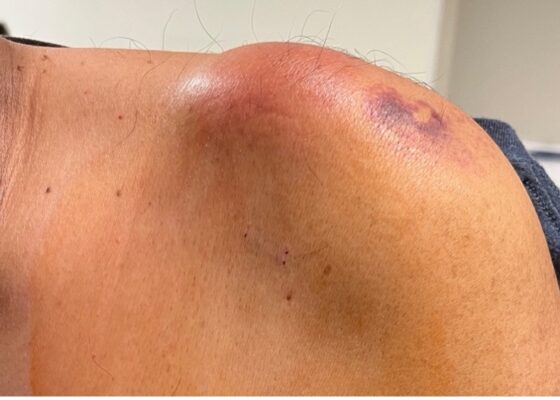
DOI: https://doi.org/10.21980/J8VP9NMagnetic resonance imaging (MRI) with contrast was obtained of the shoulder and ankle, and results from both scans showed findings consistent with septic arthritis complicated by intraarticular abscesses. The MRI of the patient’s left acromioclavicular joint is shown as both a T1-weighted sequence in sagittal view and T2-weighted sequence in coronal view. The images show effusion (the dark fluid denoted by the red arrow) with an adjacent fluid collection (blue arrow). A T2-weighted MRI in coronal view of the patient’s right ankle showing multiple effusions (green arrows) and a fluid collection along the medial tibial cortex and subcutaneous tissues (yellow arrow).
A Case Report of Invasive Mucormycosis in a COVID-19 Positive and Newly-Diagnosed Diabetic Patient
DOI: https://doi.org/10.21980/J81M1GOn physical exam, when the patient was asked to try and look to her right, the right eye failed to move laterally/abduct (blue arrow). Additionally, when asked to look straight ahead, the eye was slightly adducted (red arrow). There was a lack of motion of the right eye in abduction when the patient was asked to look to her right (yellow arrow).
A Patient with Generalized Weakness – A Case Report
DOI: https://doi.org/10.21980/J8593CThe CT of the abdomen and pelvis showed evidence of a large subcapsular rim-enhancing fluid collection with multiple gas and air-fluid levels along the right kidney measuring 8 x 4 cm axially and 11 cm craniocaudally (blue outline) with mass effect on the right renal parenchyma (yellow outline). Another suspected fluid collection adjacent to the upper pole of the right kidney measuring 4 x 3.4 cm was noted (red outline). Bilateral pyelonephritis was suggested without hydronephrosis or nephrolithiasis. The findings suggested complicated pyelonephritis with emphysematous abscess and hematoma formation.
Flipping Tickborne Illnesses with Infographics
DOI: https://doi.org/10.21980/J83H12After participation in this module, learners will be able to 1) list the causative agents for Lyme Disease, Babesiosis, Tularemia, Ehrlichiosis, Anaplasmosis, Tick Paralysis, Rocky Mountain Spotted Fever, and Powassan Virus, 2) identify different clinical features to distinguish the different presentations of tickborne illnesses, and 3) provide the appropriate treatments for each illness.