Search By Topic
Found 48 Unique Results
Page 1 of 5
Page 1 of 5
Page 1 of 5
Innovative Ultrasound-Guided Erector Spinae Plane Nerve Block Model for Training Emergency Medicine Physicians
DOI: https://doi.org/10.21980/J8PW7DThis innovation model is designed to facilitate hands-on training of the ultrasound-guided ESP nerve block using a practical, realistic, and cost-effective ballistics gel model. By the end of this training session, learners should be able to: 1) identify relevant sonoanatomy on the created simulation model; 2) demonstrate proper in-plane technique; and 3) successfully replicate the procedure on a different target on the created training model.
Orthopaedic Surgery Didactic Session Improves Confidence in Distal Radius Fracture Management by Emergency Medicine Residents
DOI: https://doi.org/10.21980/J8K365By the end of this didactic session, learners should be able to: 1) assess DRF displacement on pre-reduction radiography and formulate reduction strategies, 2) perform a closed reduction of a DRF, 3) apply a safe and appropriate plaster splint to patient with a DRF and assess the patient’s neurovascular status, 4) assess DRF post-reduction radiography for relative fracture alignment, and 5) understand appropriate follow-up and necessary return precautions.
The Advantage of Using Video Laryngoscope in Puncture and Incisional Drainage of Peritonsillar Abscess: A Case Report
DOI: https://doi.org/10.21980/J8G935Incision of the peritonsillar abscess was performed with the assistance of the C-MAC video laryngoscope which provided a clear, illuminated, and unobstructed view of the incision site. Local anesthesia with 1% xylocaine was administered, and the abscess was incised with a scalpel and drained with a forceps.
High-Fidelity Simulation with Transvaginal Ultrasound in the Emergency Department
DOI: https://doi.org/10.21980/J8606QBy the end of the session, learners should be able to 1) recognize the clinical indications for transvaginal ultrasound in the ED, 2) practice the insertion, orientation, and sweeping motions used to perform a TVPOCUS study, 3) interpret transvaginal ultrasound images showing an IUP or alternative pathologies, and 4) understand proper barrier, disinfection, and storage techniques for endocavitary probes.
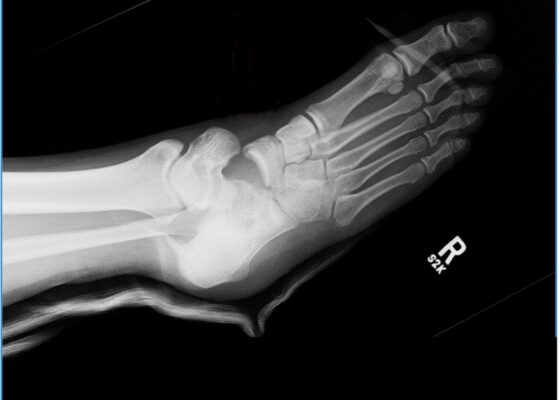
A Case Report of Lateral Subtalar Dislocation: Emergency Medicine Assessment, Management and Disposition
DOI: https://doi.org/10.21980/J8SS8PIn a lateral subtalar dislocation, the navicular bone (red bone in 3D anatomy image) and the calcaneus (yellow bone in 3D anatomy image) dislocate laterally in relation to the talus (lavender bone in 3D anatomy image). Plain film oblique and lateral X-rays demonstrate the initial dislocation (talus in red, navicular in blue). It is clear in the initial lateral view that there is loss of the talar/navicular articulation (noted by red arrow). The anterior-posterior x-ray is more challenging to discern the anatomy; however, the talus (red dot) is laterally displaced in comparison to the navicular (blue dot).
Modification of an Airway Training Mannequin to Teach Engagement of the Hyoepiglottic Ligament
DOI: https://doi.org/10.21980/J8R06PBy the end of this education session, participants should be able to: 1) identify relevant airway anatomy during intubation, including base of the tongue, epiglottis, midline vallecular fold, anterior arytenoids; 2) appreciate the value of a stepwise anatomically guided approach to intubation; 3) become familiar with the midline vallecular fold and underlying anatomy, including the hyoepiglottic ligament, and how proper placement of the laryngoscope can result in improved glottic visualization.
A Realistic, Low-Cost Simulated Automated Chest Compression Device
DOI: https://doi.org/10.21980/J8M63CBy the end of this educational session using a resuscitation trainer or high-fidelity manikin, learners should be able to: 1) recognize appropriate application of simulated ACCD to an ongoing resuscitation case; 2) demonstrate proper positioning of simulated ACCD in manikin model and 3) integrate simulated ACCD to provide compressions appropriately throughout cardiac arrest scenario.
Low-Cost Fishhook Removal Simulation
DOI: https://doi.org/10.21980/J8Q64PThe goal of this small group session is to fill the gap in training on fishhook injuries. At the end of the session participants should be able to describe the parts of a fishhook, as well as demonstrate and have increased confidence in performing multiple fishhook removal techniques.
Adolescent with Diabetic Ketoacidosis, Hypothermia and Pneumomediastinum
DOI: https://doi.org/10.21980/J8FP8JBy the end of the simulation, learners will be able to: 1) develop a differential diagnosis for an adolescent who presents obtunded with shortness of breath; 2) discuss the management of diabetic ketoacidosis; 3) discuss management of hypothermia in a pediatric patient; 4) discuss appropriate ventilator settings in a patient with diabetic ketoacidosis; and 5) demonstrate interpersonal communication with family, nursing, and consultants during high stress situations.
Inhalational Injury Secondary to House Fire
DOI: https://doi.org/10.21980/J8TW7NAt the conclusion of the simulation session, learners will be able to: 1) recognize the indications for intubation in a thermal burn/inhalation injury patient; 2) develop a systematic approach to an inhalational injury airway; and 3) recognize indications for transfer to burn center.