Search By Topic
Found 16 Unique Results
Page 1 of 2
Page 1 of 2
Page 1 of 2
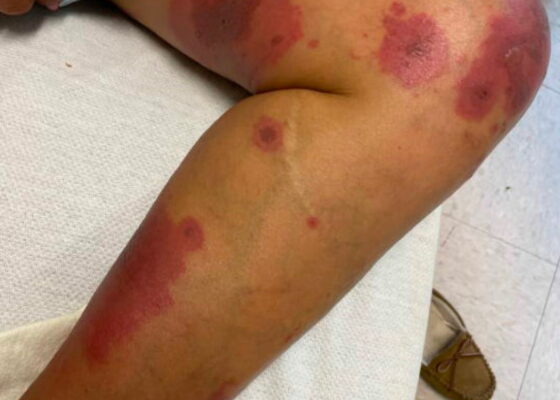
A Case Report on an Elusive Incident of Erythema Multiforme
DOI: https://doi.org/10.21980/J8BM0WHer physical exam was notable for multiple scattered tense vesicles on an erythematous base along the left and right lower extremities and right upper extremity. The lesions were excoriated and in different stages of evolution. No oral, mucosal, or conjunctival lesions were found. Physical exam was otherwise unremarkable.
Septic Abortion Complicated by Disseminated Intravascular Coagulation
DOI: https://doi.org/10.21980/J8GH1GAt the conclusion of the simulation session, learners will be able to: 1) Obtain a relevant focused history including pregnancy history, medication use, and past medical history. 2) Develop a differential for fever and vaginal bleeding in a pregnant patient. 3) Discuss management of septic abortion, including empiric broad-spectrum antibiotics and obstetric consultation for source control with dilation and curettage (D&C). 4) Discuss expected laboratory findings of disseminated intravascular coagulation (DIC). 5) Discuss management of DIC, including identification of underlying etiology and supportive resuscitation with blood products. 6) Review the components of blood products. 7) Identify appropriate disposition of the patient to the intensive care unit (ICU).
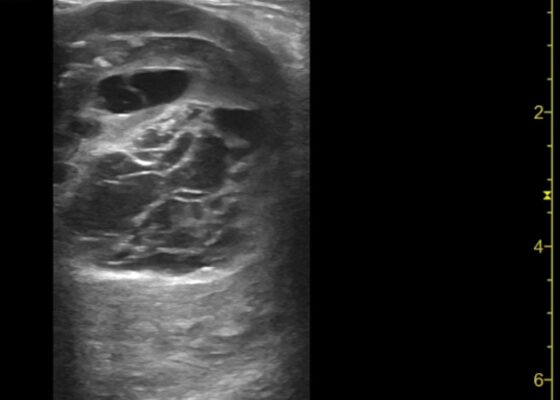
Thigh Mass Case Report
DOI: https://doi.org/10.21980/J8QD3CPoint-of-care ultrasound (POCUS) demonstrates a large, subcutaneous mass with areas of mixed echogenicity. The mass contains fluid-filled, anechoic areas with internal septations and absent doppler flow. The majority of the mass appears isoechoic to the surrounding tissues with a hyperechoic border. Computed tomography (CT) of his right thigh shows a 16 x 8.1 x 9.5 cm heterogenous, complex mass within his hamstring muscles, inferior to the femur. His lab work was significant for a white blood cell (WBC) of 17.3 (103/µL).
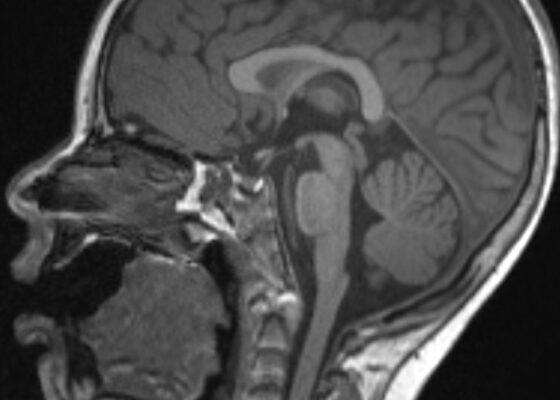
An Unusual Case Report of a Toddler with Metastatic Neuroblastoma Mimicking Myasthenia Gravis
DOI: https://doi.org/10.21980/J8G35VWhile still in the ED, MRI with and without gadolinium contrast of the brain, orbits, and cervical, thoracic and lumbar spine were obtained to evaluate for possible CNS lesions including encephalitis, myelitis, or demyelination. Imaging, however, demonstrated multiple unexpected findings: a T1 hypointense, T2 hyperintense and heterogeneously enhancing right adrenal mass measuring 2.7 x 2.1 x 3 cm (yellow asterisk) along with heterogenous enhancement at the clivus, C6, C7, T7, T8, T12, and L3 vertebral bodies (red asterisks). There were otherwise no significant intracranial signal or structural abnormalities and normal orbits.
HIT-Heparin Induced Thrombocytopenia Simulation Case
DOI: https://doi.org/10.21980/J89Q0MAfter completing this simulated case, participants will be able to: 1) Obtain a detailed history that includes recent medications, medical, surgical, and social history to evaluate for HIT risk factors, 2) perform an adequate neurovascular exam including evaluation of motor function, sensation, skin color, pulses, and capillary refill, 3) order appropriate laboratory testing and imaging for diagnosis of thrombocytopenia and arterial occlusion, including bed side doppler or ultrasound, 4) discuss and recognize the symptoms of HIT and the contraindications of platelet and heparin administration in the emergency department, 5) avoid administration of heparin in the emergency department setting and recognize that platelets may worsen thrombus formation and lead to limb amputation, 6) select appropriate medications for treatment and determine appropriate disposition for a patient presenting with HIT, 7) demonstrate interpersonal communication with patient and family, 8) recognize that HIT with thrombosis is a potential complication in hospitalized patients and outpatient settings and is associated with high mortality rates.
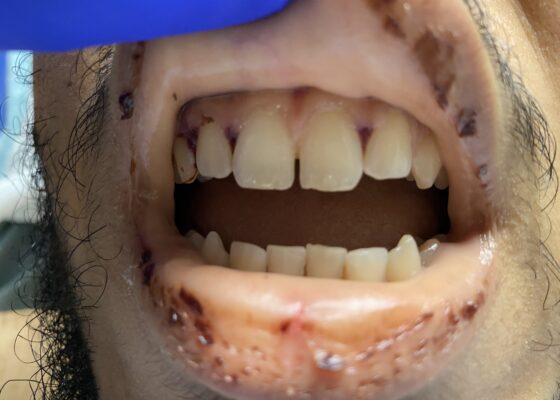
Case Report of Thrombotic Thrombocytopenic Purpura in a Previously Healthy Adult
DOI: https://doi.org/10.21980/J8VK9MThe physical exam revealed globalized pallor of his skin as well as conjunctival pallor. Mucous membranes were found to be dry and pale with dried gingival hemorrhages apparent between teeth (image). Additionally, mild hepatosplenomegaly was noted. While in the ED, the patient’s urine was dark reddish-brown, which he then reported had been similarly discolored for the past 7 days.
Blast Crisis
DOI: https://doi.org/10.21980/J8W35KBy the end of this simulation, the participant will be able to: 1) create a thorough differential for the undifferentiated febrile, altered patient, 2) identify the signs and symptoms of blast crisis, 3) describe proper resuscitation of a patient in blast crisis, and 4) describe the indications, steps, and contraindications of performing a lumbar puncture.
Rapid Airway Narrowing Associated with Hodgkin’s Lymphoma
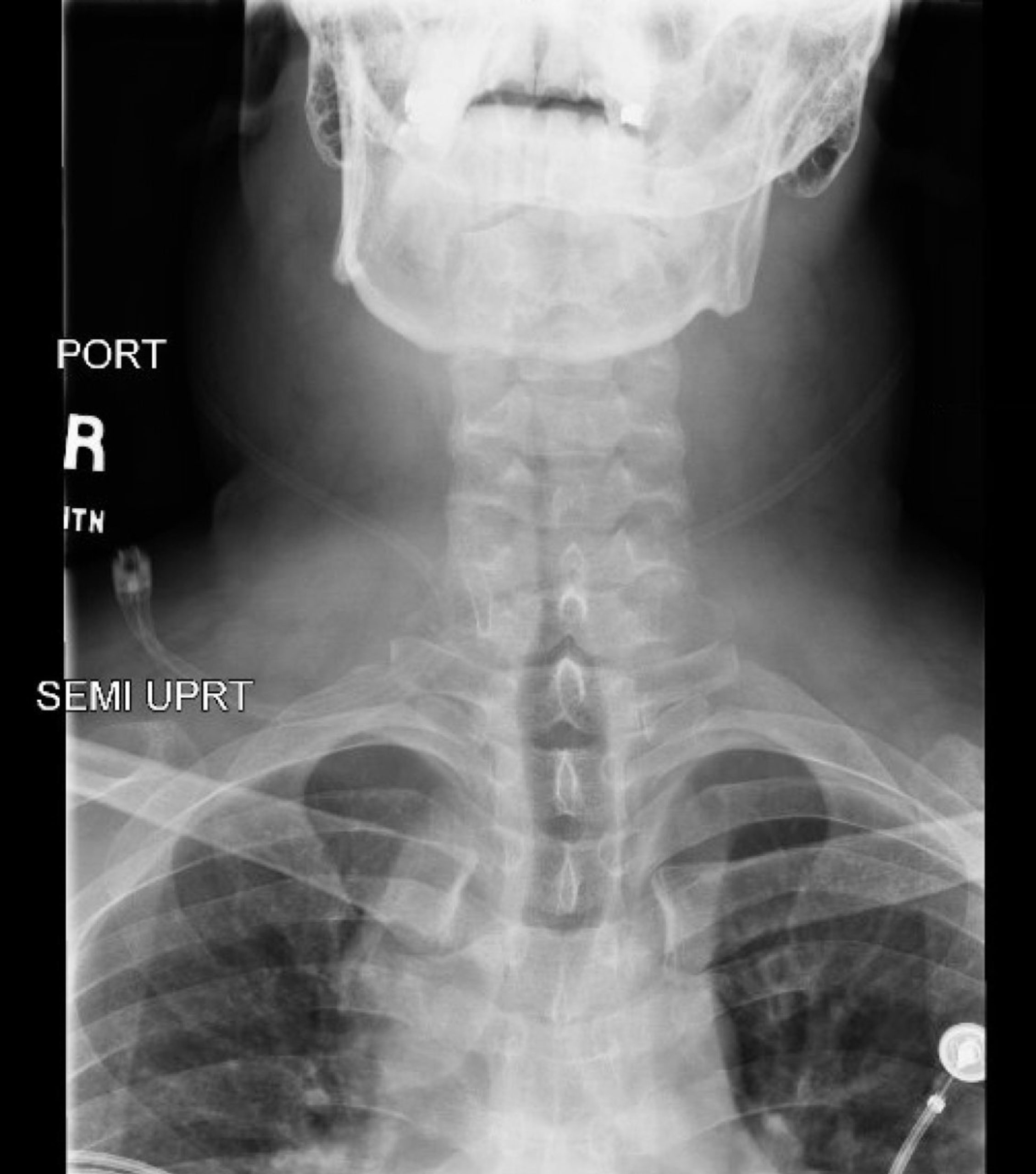
DOI: https://doi.org/10.21980/J86D3QNeck X-ray showed nonspecific significant prevertebral soft tissue swelling at the level of the cervical spine, with associated apparent thickening of the epiglottis (yellow arrow), diffuse soft tissue swelling of the neck (red arrows) and tracheal airway narrowing (light blue arrow). The computed tomography imaging of the neck was significant for multiple conglomerating pathological lymph nodes with a significant mass effect (orange arrows) compressing the right internal jugular vein (green arrow).
Spontaneous Intracranial Hemorrhage in Severe Hemophilia A: A Rare Cause of Seizure in a Young Child
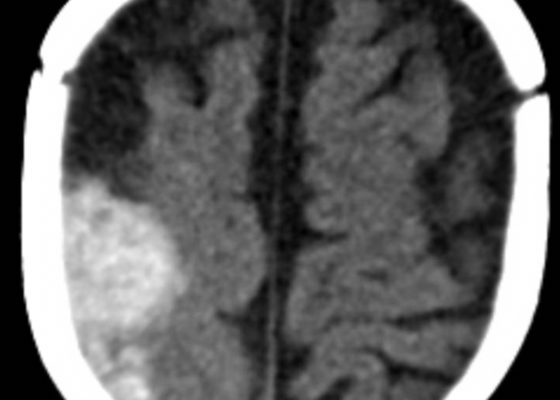
DOI: https://doi.org/10.21980/J8G91DA computed tomography (CT) scan of the head without contrast was obtained out of concern for intracranial pathology due to the patient’s young age and the witnessed focal seizure. The CT showed a 4.2 x 1.2 x 1.5 cm acute extra-axial intracranial right frontoparietal hemorrhage favoring epidural over subdural hemorrhage given its lenticular shape. There was no underlying fracture, herniation or midline shift identified.
Novel Emergency Medicine Curriculum Utilizing Self-Directed Learning and the Flipped Classroom Method: Hematologic/Oncologic Emergencies Small Group Module
DOI: https://doi.org/10.21980/J8VW56We aim to teach the presentation and management of psychiatric emergencies through the creation of a flipped classroom design. This unique, innovative curriculum utilizes resources chosen by education faculty and resident learners, study questions, real-life experiences, and small group discussions in place of traditional lectures. In doing so, a goal of the curriculum is to encourage self-directed learning, improve understanding and knowledge retention, and improve the educational experience of our residents.