Ob/Gyn
Postpartum Complications Modified TBL
DOI: https://doi.org/10.5070/M5.52264By the end of this session learners will be able to: 1) identify the timeline in which postpartum complications typically occur, 2) discuss the specific differential diagnoses common in the postpartum period, 3) recognize risk factors for endometritis and mastitis, 4) recognize the presentation of postpartum cardiomyopathy and pituitary infarction, 5) formulate a treatment plan for postpartum endometritis including appropriate antibiotics and disposition, 6) formulate a treatment plan for mastitis including appropriate antibiotics and disposition, 7) formulate an appropriate assessment plan for pituitary infarction with appropriate disposition, and 8) formulate an appropriate treatment plan and disposition for postpartum cardiomyopathy.
A Woman’s Infertility Journey Complicated by Severe Ovarian Hyperstimulation Syndrome – A Case Report
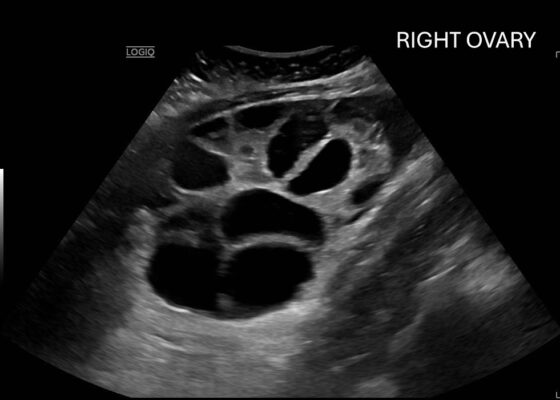
DOI: https://doi.org/10.5070/M5.52309Computed tomography (CT) of the abdomen and pelvis demonstrated pleural effusions in the lung bases (blue stars), ascites (blue stars), and enlarged ovaries with multiple cysts/follicles (white arrows). A formal pelvic US also demonstrated large volume ascites (white diamonds) and bilateral ovarian enlargement with numerous cysts. A CT angiogram (CTA) of the chest demonstrated small bilateral pleural effusions and no obvious pulmonary embolism.
The EMazing Race: A Novel Gamified Board and Clinical Practice Review for Emergency Medicine Residents
DOI: https://doi.org/10.21980/J8.52075By the end of this 2-hour session, learners will demonstrate their knowledge on the following board-related emergency medicine topics: Ob/GYN – links to 13.7 Complications of Delivery in Core Model of EM 2022, Renal/GU – links to 15.0 Renal and Urogenital Disorders in Core Model of EM 2022 and Splinting – links to 18.1.8.2 Extremity bony trauma, fracture in Core Model of EM 2022.
Critical Care Transport: Blunt Polytrauma in Pregnancy
DOI: https://doi.org/10.21980/J81366At the completion of this simulation participants will be able to 1) perform primary and secondary trauma surveys, 2) assess the neurovascular status of a tibia/fibula fracture, 3) appreciate anatomic and physiologic differences in pregnancy, 4) appropriately order analgesia and imaging, 5) recognize and treat hemorrhagic shock, 6) perform an extended focused assessment with sonography in trauma exam (eFAST) in undifferentiated hemorrhage, 7) identify a displaced pelvic fracture and properly apply a pelvic binder, and 8) obtain and interpret fetal heart rate using ultrasound.