Latest Articles
Escape Intern Orientation! — A Capstone and Team Building Activity for New EM Interns
DOI: https://doi.org/10.5070/M5.52158By the end of this small group exercise, learners will be able to: 1) identify first, second, and third-degree heart block on a 12-lead ECG; 2) recognize STEMI pattern on a 12-lead ECG; 3) categorize appropriate images that make up an EFAST exam for a trauma patient; 4) recall the proper management of a tension pneumothorax; 5) identify an organized approach to emergency department rapid-sequence intubation (RSI); 6) recognize acute otitis media (AOM); 7) locate the appropriate antibiotic and pediatric dose to treat acute otitis media via the Harriet Lane Handbook; 8) demonstrate how to apply evidence-based guidelines to a clinical case of neonatal pediatric fever; 9) recall common clinical findings of basilar skull fracture; 10) identify important concepts in the management of stroke syndromes; 11) recognize vital sign abnormalities that could indicate sepsis; and 12) review important concepts related to the management of septic patients.
Enhancing Relationship-Centered Communication and Feedback in Emergency Medicine Through Applied Improvisation (EM-PROV)
DOI: https://doi.org/10.5070/M5.52345By the end of this session, learners will be able to improve relationship-centered communication (RCC): 1) define “yes, and” and its role in RCC, and 2) demonstrate active listening and responsiveness using improvisational techniques such as “yes, and,” gift-giving, establishing scene, and callbacks. They will also be able to improve learner feedback: 1) define “yes, and” and its role in learner feedback, 2) review three evidence-based feedback models through a “yes, and” lens, and 3) practice improv techniques and deliver structured feedback in real-time peer scenarios using improvisational techniques such as “yes, and,” gift-giving, establishing scenes, and callbacks.
Postpartum Complications Modified TBL
DOI: https://doi.org/10.5070/M5.52264By the end of this session learners will be able to: 1) identify the timeline in which postpartum complications typically occur, 2) discuss the specific differential diagnoses common in the postpartum period, 3) recognize risk factors for endometritis and mastitis, 4) recognize the presentation of postpartum cardiomyopathy and pituitary infarction, 5) formulate a treatment plan for postpartum endometritis including appropriate antibiotics and disposition, 6) formulate a treatment plan for mastitis including appropriate antibiotics and disposition, 7) formulate an appropriate assessment plan for pituitary infarction with appropriate disposition, and 8) formulate an appropriate treatment plan and disposition for postpartum cardiomyopathy.
Midline Catheters: A Novel Curriculum for Emergency Medicine Residents
DOI: https://doi.org/10.5070/M5.52243The purpose of this curriculum is to teach emergency medicine residents how to place and utilize midline catheters.
Stopping Fistula Hemorrhage without Bleeding Time and Money – A Low Cost, Low Resource Hemodialysis Fistula Model for Emergency Medicine Residents
DOI: https://doi.org/10.5070/M5.52204After using the task trainer bleeding fistula model, learners will be able to: 1) identify vascular access hemorrhage as an emergency presentation in dialysis patients; 2) execute a stepwise approach to manage a bleeding fistula; 3) demonstrate effective hemorrhage control for a patient with uncontrolled bleeding from their fistula, including choice of appropriate suture material and suturing technique; and 4) discuss pitfalls of hemorrhage control in patients with fistulas, including risks of tourniquet use and complications related to clot formation at the fistula site.
OptimEYEzing Emergency Skills: A Novel Model for Ocular Procedural Education for Emergency Medicine Residents
DOI: https://doi.org/10.5070/M5.52212By the end of this session, learners will be able to: 1) identify signs and symptoms of ocular emergencies, 2) appraise for indications to perform ocular procedures, 3) demonstrate procedural competence in ocular foreign body removal, fluorescein staining, lateral canthotomy, and intraocular pressure (IOP) measurements, 4) relate increased procedural confidence with ocular procedures.
Low-Cost, Reusable Fracture Reduction Task Trainer for Distal Radius Fractures
DOI: https://doi.org/10.5070/M5.52357Utilizing this task trainer, learners will be able to 1) identify key anatomic structures, 2) distinguish a Colles from a Smith fracture of the radius, 3) understand fracture reduction technique using traction, translation and angulation, 4) appreciate the amount of force required for manipulation of the distal fracture fragment, and 5) gain hands-on practice using a model with similar haptics to bone and soft tissue.
A Novel Low-Cost Phantom for Ultrasound-Guided Fascia Iliaca Nerve Blocks
DOI: https://doi.org/10.5070/M5.52321By the end of the training session using the FI phantom and bedside ultrasound, learners should be able to: 1) discuss indications, contraindications, and complications of FI blocks; 2) identify anatomy relevant to performing an FI block on ultrasound; and 3) independently perform an FI block or demonstrate proper needle position for FI block on ultrasound of the phantom.
A Case Report of Acute Appendicitis Complicated by Appendicoliths
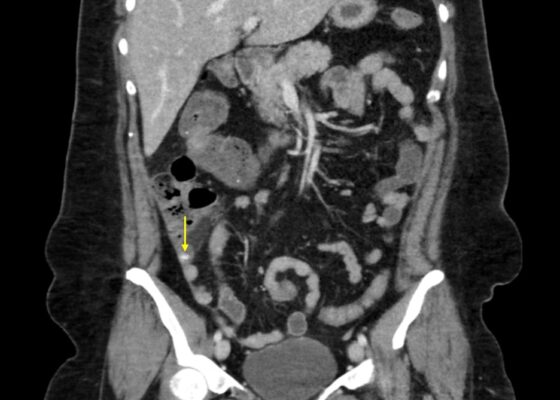
DOI: https://doi.org/10.5070/M5.52213Contrast-enhanced CT of the abdomen and pelvis was obtained. Coronal CT demonstrated a dilated appendix measuring up to 1.2 cm in diameter with multiple appendicoliths (yellow arrows), the largest measuring 1.1 cm. Mild periappendiceal fat stranding was present, consistent with acute appendicitis complicated by appendicoliths. The surrounding bowel and colon were normal in caliber and distribution. An additional coronal view demonstrated a dilated appendix (yellow arrow) containing an appendicolith with periappendiceal inflammatory changes. No evidence of perforation, abscess, or drainable fluid collection was identified.
Case Report: Acute Dyspnea in a Young Female
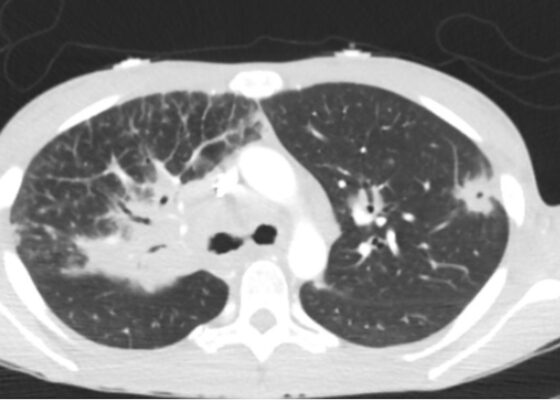
DOI: https://doi.org/10.5070/M5.52254The patient underwent computer tomography (CT) imaging of the chest, abdomen, and pelvis. Computer tomography of the chest showed bilateral diffuse pulmonary nodules in a perilymphatic distribution (yellow arrows), and diffusely increased mediastinal and hilar soft tissue densities (blue circle), likely representing lymphadenopathy; a left upper lobe lesion with central cavitation (orange circle) was also seen likely to be associated with the same disease process as the extensive lymphadenopathy. Imaging of the abdomen and pelvis was significant for diffuse hypodensities of the liver and spleen suggesting a multi-system process.