Abdominal/Gastroenterology
A Case Report of Acute Appendicitis Complicated by Appendicoliths
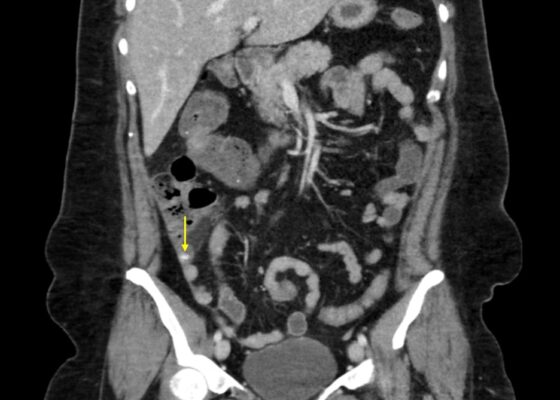
DOI: https://doi.org/10.5070/M5.52213Contrast-enhanced CT of the abdomen and pelvis was obtained. Coronal CT demonstrated a dilated appendix measuring up to 1.2 cm in diameter with multiple appendicoliths (yellow arrows), the largest measuring 1.1 cm. Mild periappendiceal fat stranding was present, consistent with acute appendicitis complicated by appendicoliths. The surrounding bowel and colon were normal in caliber and distribution. An additional coronal view demonstrated a dilated appendix (yellow arrow) containing an appendicolith with periappendiceal inflammatory changes. No evidence of perforation, abscess, or drainable fluid collection was identified.
Trapped In Transit – A Case Report of a Pediatric Gastric Bezoar Causing Intermittent Small Bowel Obstruction
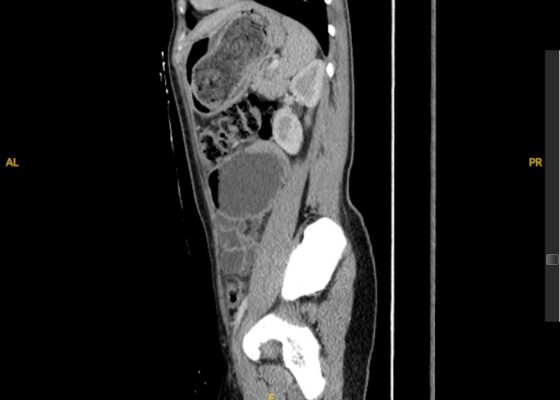
DOI: https://doi.org/10.5070/M5.52259The CT scan identified a heterogenous, mass-like lesion extending from the gastric fundus to the antrum, along with a small bowel obstruction (SBO) and significant small bowel dilation. An additional smaller heterogenous mass-like lesion was seen in the small bowel, causing the SBO. Given the mass-like lesion’s mixed attenuation and presence of internal air, a gastric bezoar was strongly suspected.
Case Report of Incarcerated Gastric Volvulus and Splenic Herniation in Undiagnosed Congenital Diaphragmatic Hernia in an Infant
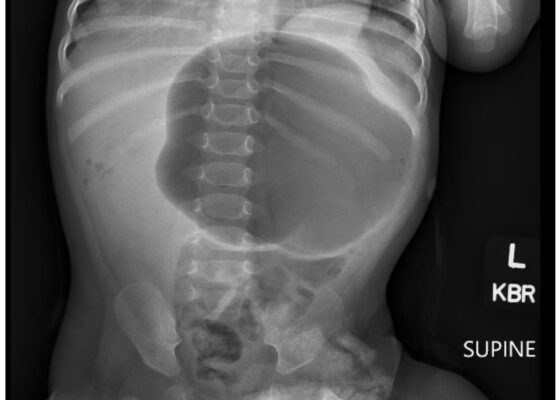
DOI: https://doi.org/10.21980/J8VD27An upper gastrointestinal series (UGI) showed an enteric tube with its tip in the stomach and side-port in the esophagus. There was a large amount of air in the stomach and a small volume of scattered distal bowel gas. The tip of an enteric tube was seen in the stomach (red arrow). Contrast partially filled the stomach, and the greater curvature was visualized superior to the lesser curvature in the left upper quadrant (blue arrow). The body of the stomach was herniated into the right chest through a Bochdalek hernia (blue star). There was a large amount of air in the stomach and a small volume of scattered distal bowel gas. These findings were consistent with mesenteroaxial gastric volvulus.
Case Report: Iatrogenic Bowel Perforation Following Dental Procedure
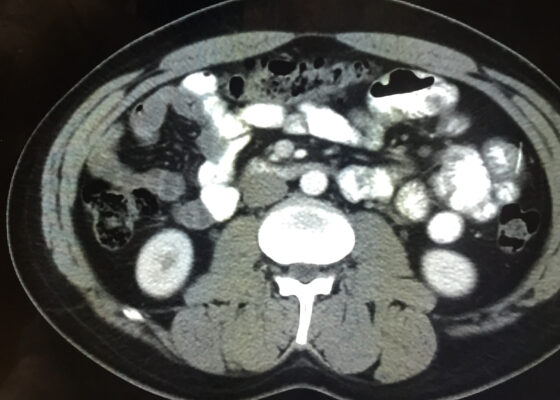
DOI: https://doi.org/10.21980/J8CD38The patient’s abdominal CT demonstrated a metallic foreign body in the left side of the abdomen within the small bowel, without surrounding induration or abscess. Radiology questioned whether the metallic foreign object perforated the bowel. Seen in the cross-sectional CT image, there is a hyperdense linear structure transversing the small intestinal wall, given that a portion of the structure was located outside of the lumen of the bowel.
A Case Report of Hydropic Gallbladder Presenting as Right Lower Quadrant Abdominal Pain
DOI: https://doi.org/10.21980/J8DD26Computed tomography (CT) of the abdomen and pelvis with contrast was ordered, and general surgery was consulted for the initial working diagnosis of acute appendicitis. However, the CT scan resulted with findings of a markedly distended gallbladder measuring approximately 14.5 x 4 centimeters (cm) with marked gallbladder wall thickening (magenta) and pericholecystic fat stranding (cyan). The appendix was not dilated and had no inflammatory changes or edema. Follow-up right upper quadrant ultrasound confirmed the diagnosis of acute cholecystitis.