Search By Topic
Found 22 Unique Results
Page 1 of 3
Page 1 of 3
Page 1 of 3
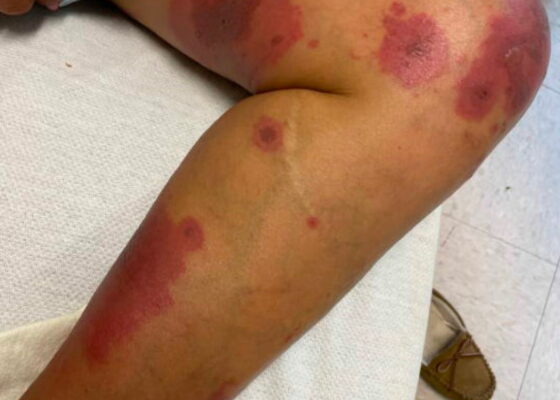
A Case Report on an Elusive Incident of Erythema Multiforme
DOI: https://doi.org/10.21980/J8BM0WHer physical exam was notable for multiple scattered tense vesicles on an erythematous base along the left and right lower extremities and right upper extremity. The lesions were excoriated and in different stages of evolution. No oral, mucosal, or conjunctival lesions were found. Physical exam was otherwise unremarkable.
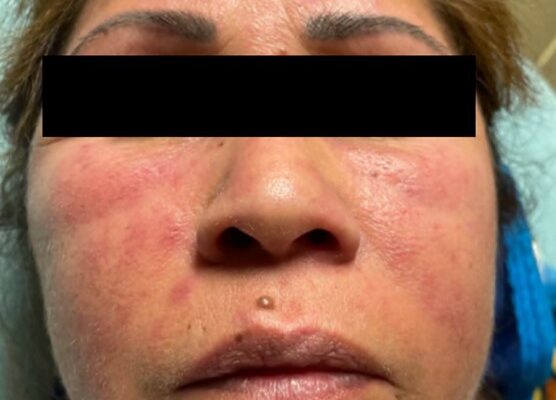
A Case Report on Dermatomyositis in a Female Patient with Facial Rash and Swelling
DOI: https://doi.org/10.21980/J8506DThe physical exam revealed significant periorbital swelling, facial edema, and a maculopapular rash across the upper chest, symmetrically across the extensor surfaces of the hands and the bilateral arms and thighs. The photograph of her face shows light-red to violaceous macules and patches, with inclusion of the nasolabial folds as well the forehead and upper eyelids with periorbital edema (heliotrope sign). The other rash images show “Shawl sign” (photograph of back showing erythema over the posterior aspect of the upper back), V sign (photograph of chest showing light-red violaceous plaque on mid-chest), Gottron's papules (photograph of hands showing light red scaly papules overlying the right proximal interphalangeal joint [R PIP] and the metacarpophalangeal joint [MCP], and holster sign (photograph of thigh showing light red patches on bilateral lateral thighs). This distribution of rashes is pathognomonic for DM.
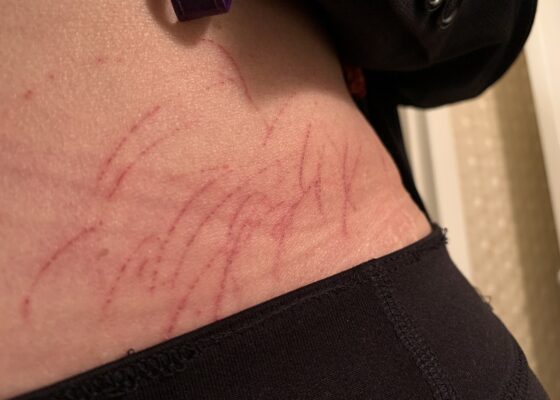
A Case Report of Dermatographia
DOI: https://doi.org/10.21980/J8P05PPhysical examination was unremarkable except for the urticaria on the right aside of her abdomen (white arrow) with overlying excoriations (stars). Of note, there were no burrows, papules or vesicles in the typical locations including the webs of the fingers, wrists, axillae, areolae, or genitalia. Examination of the linear dermatographia clearly revealed superficial wheals, versus underlying serpiginous lesions.
An Appy That Needs Epi: An Atypical Presentation of Anaphylaxis
DOI: https://doi.org/10.21980/J80H14At the conclusion of the simulation, learners will be able to: 1) demonstrate ability to efficiently review patient records to optimize patient care and identify relevant details to current presentation, 2) rapidly assess a patient when there is a change in clinical status, 3) recognize the need to start resuscitative fluids for undifferentiated hypotension, 4) identify anaphylaxis, 5) demonstrate the medical management of anaphylaxis, 6) utilize the I-PASS framework to communicate with the inpatient team during the transition of care.
Not Another Presentation of Cellulitis: A Case Report of Erythromelalgia
DOI: https://doi.org/10.21980/J8BD2KEpisodic tender, warm, erythematous swelling of the extremity experienced by this patient is typical of erythromelalgia. Erythematous streaking on the volar surface of the left forearm (red arrow) and tender, warm, erythematous blanching swelling was present on the palmar hand (yellow arrow). Most patients with erythromelalgia also have lower extremity involvement including the dorsum or sole of the foot and toes.1
A Culinary Misadventure: A Case Report of Shiitake Dermatitis
DOI: https://doi.org/10.21980/J8X936Close visual examination revealed erythematous linear papules on her upper and lower back. No bullae, drainage, or sloughing of the skin was present. The rest of her body, including palms, soles, and mucosa, was spared.
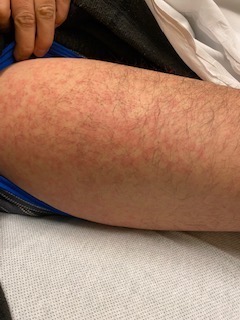
Case Report of COVID-19 Positive Male with Late-Onset Full Body Maculopapular Rash
DOI: https://doi.org/10.21980/J86W72The images demonstrate a diffuse, flat, maculopapular exanthema along the torso, bilateral upper and lower extremities, and neck without edema consistent with reported cutaneous manifestations of COVID-19. There are no surrounding bullae, vesicles, or draining. On palpation, there was blanching of the rash. Sensation to light touch was intact in all extremities. The findings were also apparent on the face with no mucosal involvement.
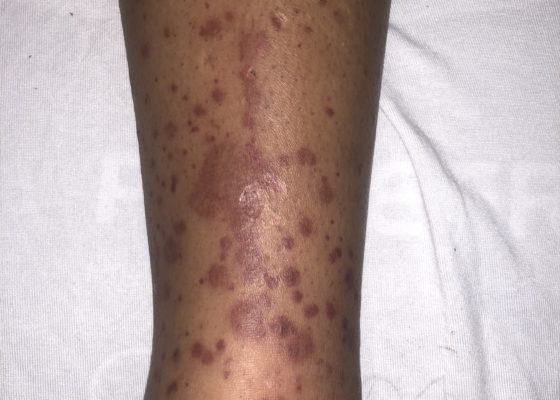
Henoch-Schönlein Purpura in the Adult
DOI: https://doi.org/10.21980/J8QH08The images show a raised, palpable, purpuric rash on the lower extremities, surrounded by a mild, 1+ non-pitting edema. Several of the lesions are exfoliated with serous discharge. There is no surrounding erythema, fluctuance, or lymphangitis to suggest cellulitis. There was no tenderness to palpation; however, pruritus was exacerbated on palpation.
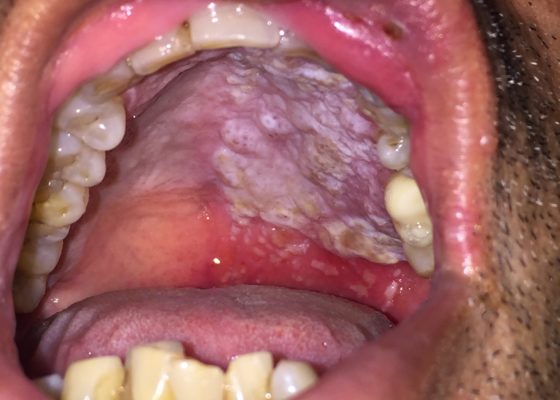
Oral Herpes Zoster
DOI: https://doi.org/10.21980/J8QS69Physical exam findings revealed vesicular lesions on the lip, hard and soft palates which did not cross the midline. The lesions appeared in the distribution of the maxillary branch (V2) of the trigeminal nerve, consistent with herpes zoster.
Levamisole Induced, Cocaine Associated Vasculitis
DOI: https://doi.org/10.21980/J8K35SAn asymmetric pattern of palpable purpura with bullae was noted on bilateral lower extremities with smaller patches on bilateral upper extremities. There was no tenderness or crepitus.