Orthopedics
Low-Cost, Reusable Fracture Reduction Task Trainer for Distal Radius Fractures
DOI: https://doi.org/10.5070/M5.52357Utilizing this task trainer, learners will be able to 1) identify key anatomic structures, 2) distinguish a Colles from a Smith fracture of the radius, 3) understand fracture reduction technique using traction, translation and angulation, 4) appreciate the amount of force required for manipulation of the distal fracture fragment, and 5) gain hands-on practice using a model with similar haptics to bone and soft tissue.
A Case Report on an Open Fracture Dislocation Injury of the Proximal Phalanx of the Thumb Resulting from Playing Cricket
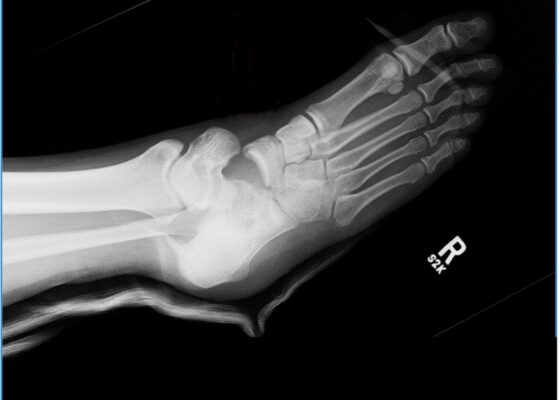
DOI: https://doi.org/10.5070/M5.52278There was an open injury to the volar aspect of the right thumb at the interphalangeal joint, with exposed bone. There was no active bleeding from the wound. He had intact sensation to the entire thumb and hand. His radial pulse was normal with normal capillary refill in all digits of his right hand. He had intact wrist flexion, extension, abduction, and adduction; however, he was unable to flex or extend his thumb secondary to the injury. He had no other injuries to the rest of his right upper extremity. An x-ray was obtained which showed a right thumb proximal phalanx intra-articular fracture (proximal fracture fragment outlined in yellow, distal fracture fragment outlined in pink) at the interphalangeal joint with dorsal dislocation of the distal phalanx (outlined in red). There were no radiopaque foreign bodies.
The EMazing Race: A Novel Gamified Board and Clinical Practice Review for Emergency Medicine Residents
DOI: https://doi.org/10.21980/J8.52075By the end of this 2-hour session, learners will demonstrate their knowledge on the following board-related emergency medicine topics: Ob/GYN – links to 13.7 Complications of Delivery in Core Model of EM 2022, Renal/GU – links to 15.0 Renal and Urogenital Disorders in Core Model of EM 2022 and Splinting – links to 18.1.8.2 Extremity bony trauma, fracture in Core Model of EM 2022.
A Comprehensive and Modality Diverse Cervical Spine and Back Musculoskeletal Physical Exam Curriculum for Medical Students
DOI: https://doi.org/10.21980/J8RQ0NBy the end of this session, students will be able to: 1) demonstrate how to properly perform a cervical spine and back physical exam, 2) understand the reasoning behind cervical spine and back PE maneuvers, 3) identify the proper technique and equipment to use for the cervical spine and back PE, 4) understand normal and abnormal findings in the cervical spine and back PE, 5) accurately record and report exam findings for the cervical spine and back PE.
Orthopaedic Surgery Didactic Session Improves Confidence in Distal Radius Fracture Management by Emergency Medicine Residents
DOI: https://doi.org/10.21980/J8K365By the end of this didactic session, learners should be able to: 1) assess DRF displacement on pre-reduction radiography and formulate reduction strategies, 2) perform a closed reduction of a DRF, 3) apply a safe and appropriate plaster splint to patient with a DRF and assess the patient’s neurovascular status, 4) assess DRF post-reduction radiography for relative fracture alignment, and 5) understand appropriate follow-up and necessary return precautions.
A Case Report of Lateral Subtalar Dislocation: Emergency Medicine Assessment, Management and Disposition
DOI: https://doi.org/10.21980/J8SS8PIn a lateral subtalar dislocation, the navicular bone (red bone in 3D anatomy image) and the calcaneus (yellow bone in 3D anatomy image) dislocate laterally in relation to the talus (lavender bone in 3D anatomy image). Plain film oblique and lateral X-rays demonstrate the initial dislocation (talus in red, navicular in blue). It is clear in the initial lateral view that there is loss of the talar/navicular articulation (noted by red arrow). The anterior-posterior x-ray is more challenging to discern the anatomy; however, the talus (red dot) is laterally displaced in comparison to the navicular (blue dot).
A Case Report of Acute Compartment Syndrome
DOI: https://doi.org/10.21980/J87061Inspection of the extremity revealed significant swelling with dark discoloration and multiple bullae (pre-operative photograph). Furthermore, notable swelling of the right foot was noted, which felt cold to palpation. Radiographs of pelvis, bilateral knees, tibia, fibula, and feet demonstrated no fractures or dislocations. The bilateral tibia and fibula X-ray revealed soft tissue swelling in the proximal legs, particularly evident in the right leg's AP view, which also showed numerous ovoid radiodensities in the anterior compartment, likely related to soft tissue injury. Post operative images are also provided demonstrating the patients’ four compartment fasciotomies which were loosely closed using staples.
Septic Arthritis of the Acromioclavicular Joint: A Case Report
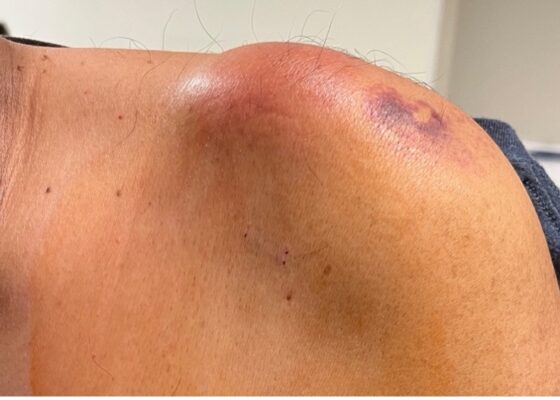
DOI: https://doi.org/10.21980/J8VP9NMagnetic resonance imaging (MRI) with contrast was obtained of the shoulder and ankle, and results from both scans showed findings consistent with septic arthritis complicated by intraarticular abscesses. The MRI of the patient’s left acromioclavicular joint is shown as both a T1-weighted sequence in sagittal view and T2-weighted sequence in coronal view. The images show effusion (the dark fluid denoted by the red arrow) with an adjacent fluid collection (blue arrow). A T2-weighted MRI in coronal view of the patient’s right ankle showing multiple effusions (green arrows) and a fluid collection along the medial tibial cortex and subcutaneous tissues (yellow arrow).