Ophthalmology
OptimEYEzing Emergency Skills: A Novel Model for Ocular Procedural Education for Emergency Medicine Residents
DOI: https://doi.org/10.5070/M5.52212By the end of this session, learners will be able to: 1) identify signs and symptoms of ocular emergencies, 2) appraise for indications to perform ocular procedures, 3) demonstrate procedural competence in ocular foreign body removal, fluorescein staining, lateral canthotomy, and intraocular pressure (IOP) measurements, 4) relate increased procedural confidence with ocular procedures.
A Case Report of Corneoscleral Laceration with Open Globe Injury and Iris Prolapse
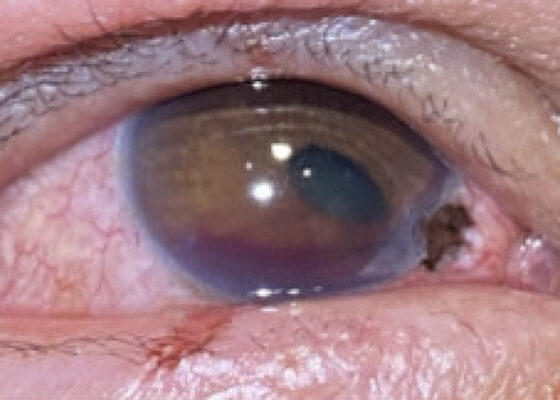
DOI: https://doi.org/10.5070/M5.52326Closer examination of the right eye revealed a 2 mm x 1 mm corneoscleral laceration to the 4-5 o'clock position at the border of zone I (yellow highlighting) and II (blue highlighting) with iris prolapse (yellow star) and plugging. Additionally, the affected eye revealed a peaked pupil (cyan highlighting) in the inferonasal direction with associated corectopia and a 2 mm Grade I hyphema (pink highlighting). Immediately inferior to the corneal laceration, 1 mm epithelial injury of the lower palpebra was present (green cross). Fluorescein exam demonstrated uptake at the 4-5 o'clock position (yellow arrow) but was negative for Seidel’s sign.
Diagnosis of Sinonasal Carcinoma in the Emergency Department: A Case Report Highlighting Red Flag Symptoms
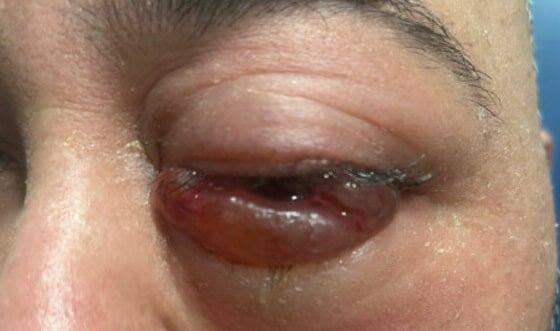
DOI: https://doi.org/10.5070/M5.52257Physical exam revealed a gross deformity of the left side of the face with soft tissue swelling with no overlying skin changes. The left eye was proptotic and completely immobile, with cranial nerve (CN) 3, 4, and 6 palsies. Additionally, a large obstructive mass was noted in the left naris with resultant rightward displacement of the nasal septum. Intraocular pressures (IOPs) were measured to be 6 mmHg in the right eye and 11 mmHg in the left eye.
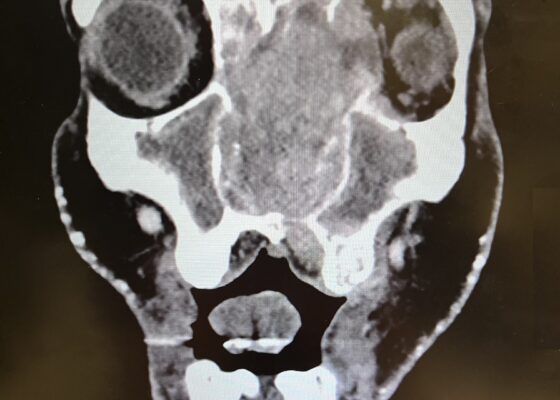
Imaging, including maxillofacial and neck soft tissue CTs revealed a large, destructive, soft tissue mass centered in the nasal cavity with significant osseous destruction of the midface and skull base (red highlighted area). There was mild intracranial extension with the mass abutting or infiltrating the inferior frontal lobes (green highlighted area). The nasal cavity and nasopharynx were obstructed (orange highlighted area). The mass invaded the left orbit with associated left-sided proptosis, left globe deformity, and compressed the left optic nerve and the left optic chiasm (blue arrows).
A Multimodal Approach to Lateral Canthotomy and Cantholysis Training for Emergency Medicine Trainees: A Simulation Training Package
DOI: https://doi.org/10.5070/M5.52351By the end of this session, learners should be able to: 1) recognize the clinical features of OCS, 2) describe the indications and steps of performing LCC, 3) perform a lateral canthotomy and cantholysis procedure on a low-fidelity model, and 4) demonstrate improved confidence in recognizing and managing OCS.
A Case Report of Carotid Cavernous Fistula: A Commonly Missed Diagnosis
DOI: https://doi.org/10.5070/M5.52242The initial physical exam performed by the ED provider revealed severe left eye chemosis, clear drainage, visual acuity of right eye 20/100 and left eye 20/400, and a left eye IOP of 52. There was a deficit of extraocular movement in all directions of gaze and limitation in all visual fields in the left eye. The MRI showed that at the level of the eye, the left cavernous sinus is asymmetrically enlarged compared to the right (red arrow) with an enlarged left inferior petrosal sinus with internal flow void on the pre-contrast MRI images (blue arrow). The orange arrow notes a central filling defect of the left superior ophthalmic vein on the MRA.
A Case Report of Inferior Rectus Abscess
DOI: https://doi.org/10.21980/J8J35GNon-contrast computed tomography (CT) imaging of the head in coronal, sagittal, and axial planes revealed a distinct 1.7 x 2.2 x 1.4 cm peripherally enhancing fluid collection within the left inferior orbit, involving the inferior rectus (yellow circle). This lesion resulted in restricted extraocular motility due to structural compression of the left globe. Laboratory results showed a mildly elevated white blood cell count of 11.5/mm3 and otherwise normal results including C-reactive protein (CRP) and erythrocyte sedimentation rate (ESR).
A Case of Painful Visual Loss – Managing Orbital Compartment Syndrome in the Emergency Department
DOI: https://doi.org/10.21980/J8N35DBy the end of this simulation, learners will be able to: 1) demonstrate the major components and a systematic approach to the emergency ophthalmologic examination, 2) develop a differential diagnosis of sight-threatening etiologies that could cause eye pain or vision loss, 3) demonstrate proficiency in performing potentially vision-saving procedures within the scope of EM practice.