Posts by JETem
A Comprehensive and Modality Diverse Cervical Spine and Back Musculoskeletal Physical Exam Curriculum for Medical Students
DOI: https://doi.org/10.21980/J8RQ0NBy the end of this session, students will be able to: 1) demonstrate how to properly perform a cervical spine and back physical exam, 2) understand the reasoning behind cervical spine and back PE maneuvers, 3) identify the proper technique and equipment to use for the cervical spine and back PE, 4) understand normal and abnormal findings in the cervical spine and back PE, 5) accurately record and report exam findings for the cervical spine and back PE.
Metastatic Calcinosis Cutis in the Emergency Department: A Case Report
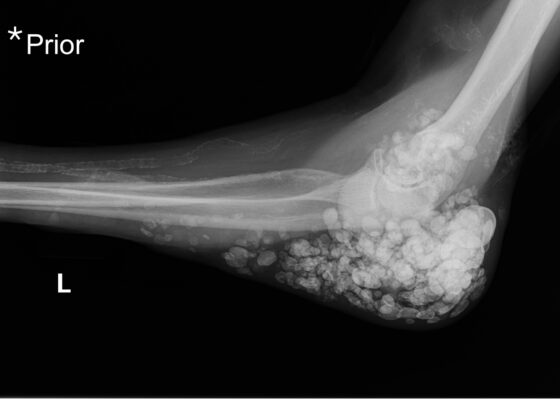
DOI: https://doi.org/10.21980/J87Q00X-ray imaging was obtained of the left elbow and showed soft tissue calcium deposits. Radiology stated, “massive periarticular calcinosis of renal failure obscures fine osseous detail. Several of the largest calcifications have decompressed since the prior exam and may contribute to the drainage observed clinically. Superimposed infection is not excluded.” X-rays with an asterisk are the comparison images from two months previous to the visit. Areas of decompression are highlighted in blue demonstrating that some of the larger calcified nodules are no longer present.
A Case Report of Facial Swelling and Crepitus Following a Dental Procedure
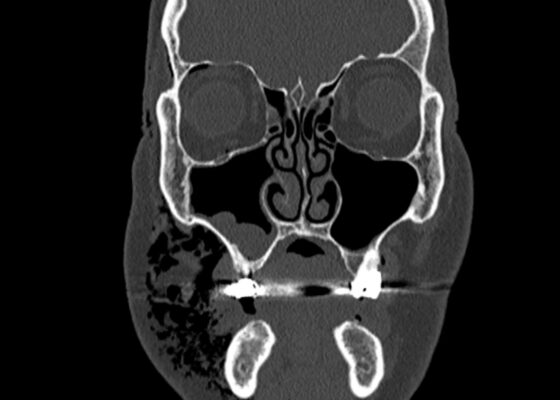
DOI: https://doi.org/10.21980/J83W8HGiven the physical exam findings of crepitus on the right neck up to the right lower eyelid, a maxillofacial CT scan without contrast was performed. It revealed diffuse subcutaneous air within the soft tissues of the face and neck and free air within the pre-septal soft tissue of the right eye, appearing as hyperlucent (dark) areas on CT within the soft tissue planes (blue outline). It showed no evidence of post-septal free air. A single-view chest X-ray was also performed and was unremarkable except for incompletely imaged soft tissue gas in the right lower neck (blue outline). On flexible fiberoptic laryngoscopy performed by ENT, the oropharynx appeared diffusely edematous and narrowed.
Case Report of Post-Operative Uvular Necrosis Following Intubation
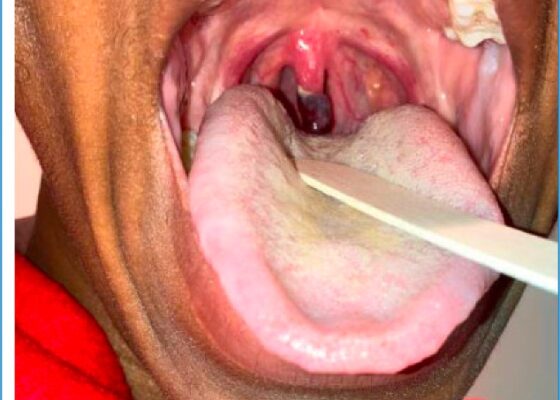
DOI: https://doi.org/10.21980/J8065JThe distal portion of her uvula was necrotic with a clear demarcation approximately halfway up the uvula. She had no trauma to the anterior oropharyngeal structures, tonsils, or adenoids. There were no lesions to the hard or soft palate. She had no carotid bruits or thrills, and no tenderness over the anterior portion of the neck.
Case Report of Incarcerated Gastric Volvulus and Splenic Herniation in Undiagnosed Congenital Diaphragmatic Hernia in an Infant
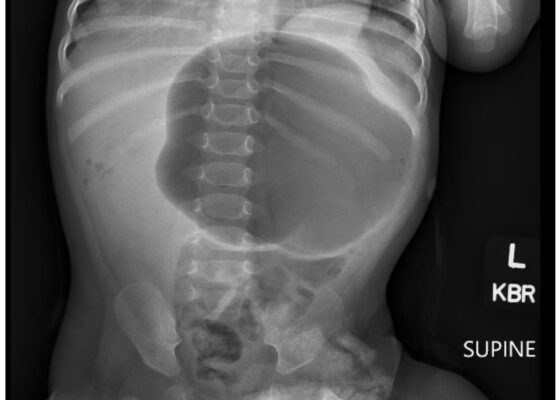
DOI: https://doi.org/10.21980/J8VD27An upper gastrointestinal series (UGI) showed an enteric tube with its tip in the stomach and side-port in the esophagus. There was a large amount of air in the stomach and a small volume of scattered distal bowel gas. The tip of an enteric tube was seen in the stomach (red arrow). Contrast partially filled the stomach, and the greater curvature was visualized superior to the lesser curvature in the left upper quadrant (blue arrow). The body of the stomach was herniated into the right chest through a Bochdalek hernia (blue star). There was a large amount of air in the stomach and a small volume of scattered distal bowel gas. These findings were consistent with mesenteroaxial gastric volvulus.
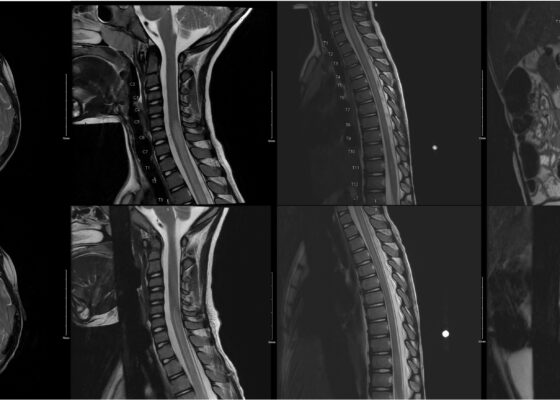
Beware of the Pediatric Limp: A Case of Mycoplasma Associated Acute Transverse Myelitis
DOI: https://doi.org/10.21980/J8QQ1QAn MRI with contrast, T2 sequence was performed. In Figures a-d, the MRI of the patient’s brain and spinal cord on admission shows abnormal signals in the patient’s pons (lack of symmetrical gray-white differentiation on cross-section) along with hyperintensity (sagittally shown as brightness in what should be homogenously intense spinal cord) and significant central cord edema (with swelling seen as increased width) starting from C5 and continuing to the conus medullaris around L1/L2.