Issue 2:2
Development of a Head and Neck Regional Anesthesia Task Trainer for Emergency Medicine Learners
DOI: https://doi.org/10.21980/J8T595In participating in the educational session associated with this task trainer, the learner will:
1) Identify landmarks for the following nerve blocks: Infraorbital, Supraorbital (V1), Mental, Periauricular
2) Demonstrate the appropriate technique for anesthetic injection for each of these nerve blocks
3) Map the distribution of regional anesthesia expected from each nerve block
4) Apply the indications and contraindications for each regional nerve block
The Halloween Lateral Canthotomy Model
DOI: https://doi.org/10.21980/J8GW2NThe purpose of the model is to teach residents and students how to perform lateral canthotomy and to achieve competency in their skills.
Emed-Opoly: Echocardiography
DOI: https://doi.org/10.21980/J8PC77By the end of this session, the learner will be able to:
1) Recognize normal and abnormal left heart global function
2) Recognize normal and abnormal right heart global function
3) Recognize pericardial effusions and pericardial tamponade
Left Ventricular Assist Devices
DOI: https://doi.org/10.21980/J8JP4ZUpon completion of this cTBL module, the learner will be able to: 1) Properly assess LVAD patients’ circulatory status; 2) appropriately resuscitate LVAD patients; 3) identify common LVAD complications; 4) evaluate and appropriately manage patients with LVAD malfunctions.
Emergency Medicine Dermatology
DOI: https://doi.org/10.21980/J8DW21By the end of this educational session, the learner will: 1) List the six primary types of rash (maculopapular, petechial/purpura, diffuse erythematous, non-erythematous, vesiculo-bullous, and pustular). 2) Be able to accurately describe various types of lesions and rashes with appropriate terminology; 3) Understand the use of the Modified Lynch Algorithm and how it can be used to narrow down the differential diagnosis in patients presenting with rash.
Pediatric Sepsis Case Scenario
DOI: https://doi.org/10.21980/J8MK5XPediatric sepsis is a low-frequency, high impact condition. Nurses and physicians do not see it often, but must recognize and treat children with sepsis efficiently when they present. This makes pediatric sepsis education particularly amenable to simulation scenarios.
Status Epilepticus in the Emergency Department
DOI: https://doi.org/10.21980/J8RC7VAt the end of this simulation session, the learner will: 1) Demonstrate the management of status epilepticus 2) Justify when airway intervention is needed for status epilepticus 3) Describe risk factors for status epilepticus 4) Prepare a differential diagnosis for the causes in status epilepticus.
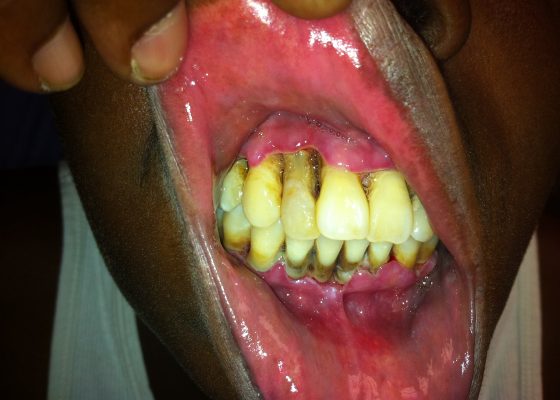
Acute Necrotizing Ulcerative Gingivitis (ANUG)
DOI: https://doi.org/10.21980/J8S88HPhysical examination revealed inflamed gingiva, ulceration, and soft tissue necrosis (Image 1) along with mandibular lymphadenopathy (not shown). Given her symptoms, poor oral care, and her immunocompromised state, she was given a diagnosis of Acute Necrotizing Ulcerative Gingivitis (ANUG) or Vincent’s Angina.