X-Ray
A Case Report on an Open Fracture Dislocation Injury of the Proximal Phalanx of the Thumb Resulting from Playing Cricket
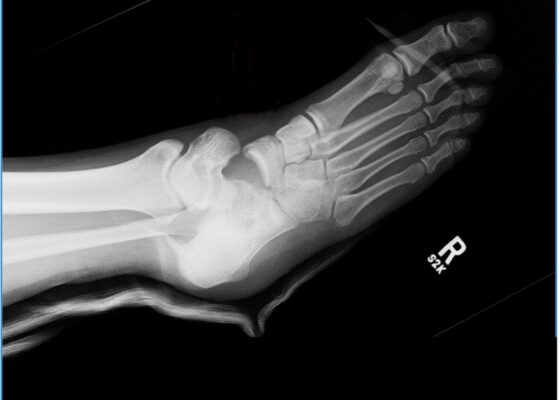
DOI: https://doi.org/10.5070/M5.52278There was an open injury to the volar aspect of the right thumb at the interphalangeal joint, with exposed bone. There was no active bleeding from the wound. He had intact sensation to the entire thumb and hand. His radial pulse was normal with normal capillary refill in all digits of his right hand. He had intact wrist flexion, extension, abduction, and adduction; however, he was unable to flex or extend his thumb secondary to the injury. He had no other injuries to the rest of his right upper extremity. An x-ray was obtained which showed a right thumb proximal phalanx intra-articular fracture (proximal fracture fragment outlined in yellow, distal fracture fragment outlined in pink) at the interphalangeal joint with dorsal dislocation of the distal phalanx (outlined in red). There were no radiopaque foreign bodies.
A Case Report of a 36-year-old Male Diagnosed with a Spontaneous Coronary Artery Dissection
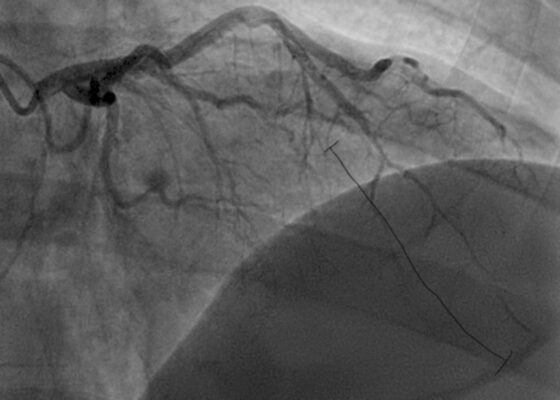
DOI: https://doi.org/10.5070/M5.52022The initial ECG obtained from the patient shows subtle ST-segment elevation noted in leads I, aVL, and V2-V5, suggestive of pathology of the left anterior descending artery. The results of the catheterization revealed a spontaneous coronary artery dissection of the distal portion of the left anterior descending coronary artery, which can be seen in the image of the angiogram, with the diseased portion notated between the brackets.
Metastatic Calcinosis Cutis in the Emergency Department: A Case Report
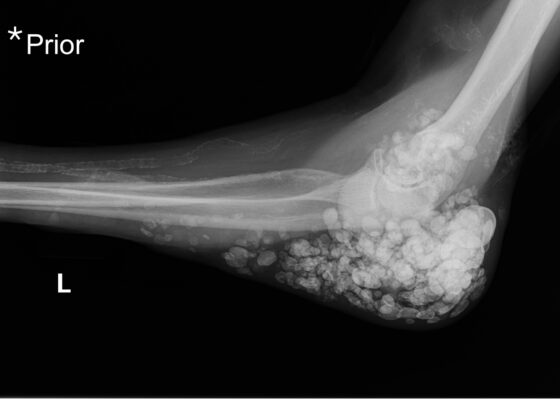
DOI: https://doi.org/10.21980/J87Q00X-ray imaging was obtained of the left elbow and showed soft tissue calcium deposits. Radiology stated, “massive periarticular calcinosis of renal failure obscures fine osseous detail. Several of the largest calcifications have decompressed since the prior exam and may contribute to the drainage observed clinically. Superimposed infection is not excluded.” X-rays with an asterisk are the comparison images from two months previous to the visit. Areas of decompression are highlighted in blue demonstrating that some of the larger calcified nodules are no longer present.
A Case Report of Facial Swelling and Crepitus Following a Dental Procedure
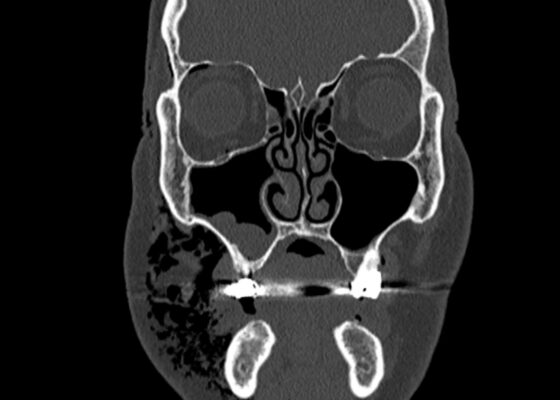
DOI: https://doi.org/10.21980/J83W8HGiven the physical exam findings of crepitus on the right neck up to the right lower eyelid, a maxillofacial CT scan without contrast was performed. It revealed diffuse subcutaneous air within the soft tissues of the face and neck and free air within the pre-septal soft tissue of the right eye, appearing as hyperlucent (dark) areas on CT within the soft tissue planes (blue outline). It showed no evidence of post-septal free air. A single-view chest X-ray was also performed and was unremarkable except for incompletely imaged soft tissue gas in the right lower neck (blue outline). On flexible fiberoptic laryngoscopy performed by ENT, the oropharynx appeared diffusely edematous and narrowed.
Case Report of Incarcerated Gastric Volvulus and Splenic Herniation in Undiagnosed Congenital Diaphragmatic Hernia in an Infant
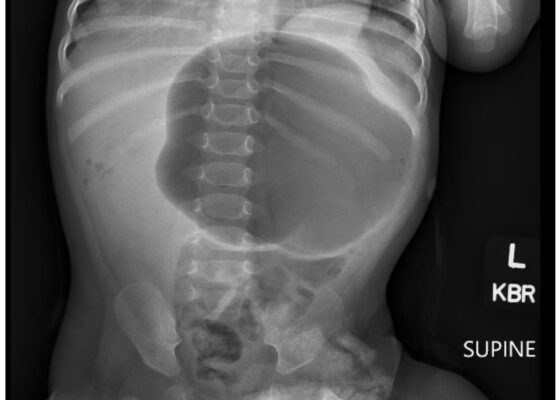
DOI: https://doi.org/10.21980/J8VD27An upper gastrointestinal series (UGI) showed an enteric tube with its tip in the stomach and side-port in the esophagus. There was a large amount of air in the stomach and a small volume of scattered distal bowel gas. The tip of an enteric tube was seen in the stomach (red arrow). Contrast partially filled the stomach, and the greater curvature was visualized superior to the lesser curvature in the left upper quadrant (blue arrow). The body of the stomach was herniated into the right chest through a Bochdalek hernia (blue star). There was a large amount of air in the stomach and a small volume of scattered distal bowel gas. These findings were consistent with mesenteroaxial gastric volvulus.
A Case Report of Lateral Subtalar Dislocation: Emergency Medicine Assessment, Management and Disposition
DOI: https://doi.org/10.21980/J8SS8PIn a lateral subtalar dislocation, the navicular bone (red bone in 3D anatomy image) and the calcaneus (yellow bone in 3D anatomy image) dislocate laterally in relation to the talus (lavender bone in 3D anatomy image). Plain film oblique and lateral X-rays demonstrate the initial dislocation (talus in red, navicular in blue). It is clear in the initial lateral view that there is loss of the talar/navicular articulation (noted by red arrow). The anterior-posterior x-ray is more challenging to discern the anatomy; however, the talus (red dot) is laterally displaced in comparison to the navicular (blue dot).
A Case Report of Acute Compartment Syndrome
DOI: https://doi.org/10.21980/J87061Inspection of the extremity revealed significant swelling with dark discoloration and multiple bullae (pre-operative photograph). Furthermore, notable swelling of the right foot was noted, which felt cold to palpation. Radiographs of pelvis, bilateral knees, tibia, fibula, and feet demonstrated no fractures or dislocations. The bilateral tibia and fibula X-ray revealed soft tissue swelling in the proximal legs, particularly evident in the right leg's AP view, which also showed numerous ovoid radiodensities in the anterior compartment, likely related to soft tissue injury. Post operative images are also provided demonstrating the patients’ four compartment fasciotomies which were loosely closed using staples.
Case Report of a Child with Colocolic Intussusception with a Primary Lead Point
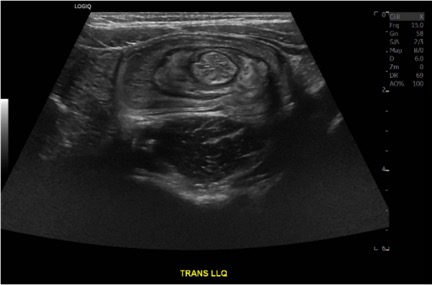
DOI: https://doi.org/10.21980/J8564QOn the initial ED visit, an abdominal ultrasound (US) was ordered which showed the classic intussusception finding of a target sign (yellow arrow), or concentric rings of telescoped bowel, on the transverse view of the left lower quadrant (LLQ).