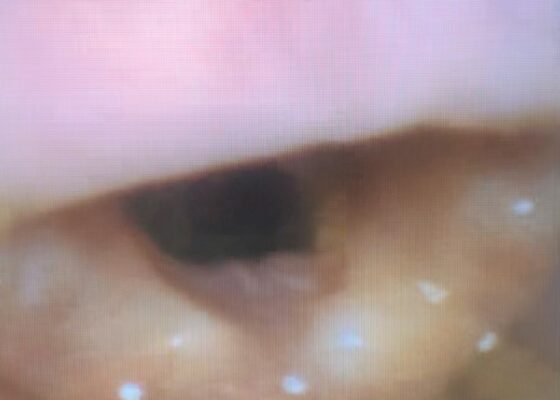
Visual EM
Evaluation of ACE-inhibitor Induced Laryngeal Edema Using Fiberoptic Scope: A Case Report
DOI: https://doi.org/10.21980/J83P9TPhysical exam was initially significant for swelling isolated to the right sided cheek and upper lip. There was no edema to lower lip, uvular swelling, or swelling to the submandibular space. She was speaking full sentences and did not endorse any voice changes. Initial vital signs were as follows: BP 125/77, HR 74, RR 16, and oxygen saturation of 100% on room air. Approximately 40 minutes later, after 125 mg solumedrol intravenous (IV) and 50mg diphenhydramine by mouth, swelling had spread to the entire upper lip and the patient reported spreading to her jaw (Photo 1). Although no jaw or submandibular edema was appreciated on physical exam, a flexible fiberoptic laryngoscope was used to evaluate the patient’s airways given worsening symptoms. Viscous lidocaine was applied intranasally five minutes prior to the procedure. The patient was positioned in a seated position on the stretcher. A flexible fiberoptic laryngoscope was then inserted through the nares and advanced slowly. Laryngoscopy showed diffuse edema of the epiglottis, arytenoids, and ventricular folds (see photos 2-4). Vital signs and respiratory status remained stable both during and after the procedure.
A Case Report of May-Thurner Syndrome Identified on Abdominal Ultrasound
DOI: https://doi.org/10.21980/J8C64KThe patient initially received a venous doppler ultrasound that showed no evidence of a right or left femoropopliteal venous thrombus. Due to the high suspicion of a DVT given the symmetric swelling to the entire limb and acute onset of pain, a CTV was ordered. The transverse view of the CTV showed chronic thrombotic occlusion of the proximal left common iliac vein associated with compression from the right common iliac artery (figure 1, transverse image of CTA), as well as thrombotic occlusion of the left internal iliac vein tributary and corresponding left ascending lumbar vein. Given the previously mentioned clinical context, these features suggested the diagnosis of May-Thurner syndrome.
Vitreous Hemorrhage Case Report
DOI: https://doi.org/10.21980/J88D3BPoint of care ultrasound (POCUS) revealed hyperechoic material in the vitreous consistent with a vitreous hemorrhage. On the ultrasound images, there is visible hyperechoic debris seen floating in the vitreous as the patient moves his eye. Since the vitreous is typically anechoic (black) in color on ultrasound, turning up the gain on the ultrasound machine makes these findings easier to see and often highlights abnormalities, such as this hemorrhage (see annotated still).
High-Pressure Injection Injury to the Hand – A Case Report
DOI: https://doi.org/10.21980/J8D64WPlain radiographs of the left hand and forearm demonstrated extensive subcutaneous emphysema. The air can be seen as lucent striations tracking along the second and third fingers as well as along the dorsum of the hand and wrist. There is also diffuse soft tissue emphysema surrounding the metacarpophalangeal joints. Lab analysis did not show any significant acute abnormalities.
Point-of-Care Ultrasound to Diagnose Molar Pregnancy: A Case Report
DOI: https://doi.org/10.21980/J82W7TA transabdominal point-of-care ultrasound (POCUS) was initiated to determine whether an abnormality to the pregnancy could be identified. Curvilinear probe was used. Our transabdominal POCUS, in the transverse plane, showed a heterogenous mass with multiple anechoic areas in the uterus. The white arrow on the ultrasound identifies these findings. The classic “snowstorm” appearance was concerning for molar pregnancy.
A Case Report of Fournier’s Gangrene
DOI: https://doi.org/10.21980/J8Z356Physical exam revealed a comfortable-appearing male patient with tachycardia and a regular cardiac rhythm. The genitourinary exam indicated significant erythema and fluctuance of the bilateral lower buttocks with extension to the perineum. Black eschar and ecchymosis were also noted at the perineum. There was significant tenderness to palpation that extended beyond the borders of erythema. There was no palpable crepitus on initial examination. Physical exam was otherwise unremarkable.
A Case Report of the Rapid Evaluation of a High-Pressure Injection Injury of a Finger Leading to Positive Outcomes
DOI: https://doi.org/10.21980/J8TD2XOn exam the patient was noted to have a punctate wound to the ulnar aspect of his right index finger, just proximal to the distal interphalangeal joint. The finger appeared pale and taut, with absent capillary refill. The patient displayed diminished range of motion with both extension and flexion of the joints of the finger. Sensation was absent and no doppler flow was appreciated to the distal aspects of the finger. X-ray of the hand was obtained and showed many small foreign bodies in the soft tissue and extensive radiolucent material consistent with gas or oil-based material to the palmar aspect of the index finger tracking up to the level of the metacarpal heads.
Unravelling the Mystery of a Continuous Coil: A Case Report
DOI: https://doi.org/10.21980/J8PM00A CT scan of the abdomen and pelvis with intravenous contrast for evaluation of new onset abdominal pain and distension was obtained in the emergency department. The axial view (CT Image A) shows the coil pack from the prior coil-assisted retrograde transvenous obliteration procedure, seen in the left renal vein and gastric varix (red arrow). The path of the coil (yellow arrow) is continuous into the inferior vena cava (CT Image B). It is then seen (CT Image C) situated in the right ventricle (green arrow). Finally, the coil pack is seen in a coronal section, demonstrating its upward path (blue arrow) in the inferior vena cava. (CT Image D). Additional findings included ascites with advanced cirrhosis. As noted in the CT images, a vascular embolization coil was seen within a varix near the junction of the left renal vein. This appeared to have unraveled and extended superiorly into the inferior vena cava and ultimately into the right atrium and right ventricle.