Infectious Disease
Using Point-of-Care Ultrasound to Expedite Diagnosis of Necrotizing Fasciitis: A Case Report
DOI: https://doi.org/10.21980/J85051A consultative scrotal ultrasound was performed, which was read as showing a small right hydrocele, small bilateral scrotal pearls, and normal-appearing testes. Although present, there was no mention of subcutaneous air suggestive of NF, seen in figure 1 as punctate hyperechoic foci (arrowhead) with ring-down artifact known as dirty shadowing (arrow). Also, subcutaneous thickening (asterisk) and free fluid (arrow) were seen as shown in figure 2, although their clinical relevance was not recognized in the radiologist's final report. Figure 3 shows an abdominal and pelvic CT that re-demonstrates subcutaneous air in the scrotum and lower abdomen (arrow) as well as fascial thickening of the perineum and free intra-abdominal air. After these images, the patient was transferred to our hospital for further management. Almost immediately after the patient's arrival, POCUS was employed. As seen in figures 4, we were able to identify in just a few minutes extensive subcutaneous air accompanied by dirty shadowing, as well as re-demonstration of subcutaneous thickening, fluid collections, and a right hydrocele. Even without the outside hospital's CT, the sonographic findings were highly suggestive for the diagnosis of NF of the perineum, also known as Fournier’s gangrene.
Auricular Perichondritis after a “High Ear Piercing:” A Case Report
DOI: https://doi.org/10.21980/J8WH16On physical examination, there was erythema, swelling, warmth, and general exquisite tenderness of the superior aspect of the left pinna (the outer ear) but excluding the ear canal, lobe, tragus, and crus. There was no facial involvement. There was no fluctuance about the ear and no drainage of fluid. The preauricular lymph nodes were enlarged and tender, but the anterior cervical lymph nodes were not tender. There was no mastoid tenderness, protrusion of the ear, or interruption of the postauricular crease.
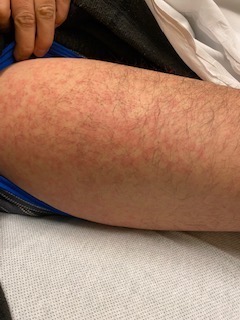
Case Report of COVID-19 Positive Male with Late-Onset Full Body Maculopapular Rash
DOI: https://doi.org/10.21980/J86W72The images demonstrate a diffuse, flat, maculopapular exanthema along the torso, bilateral upper and lower extremities, and neck without edema consistent with reported cutaneous manifestations of COVID-19. There are no surrounding bullae, vesicles, or draining. On palpation, there was blanching of the rash. Sensation to light touch was intact in all extremities. The findings were also apparent on the face with no mucosal involvement.
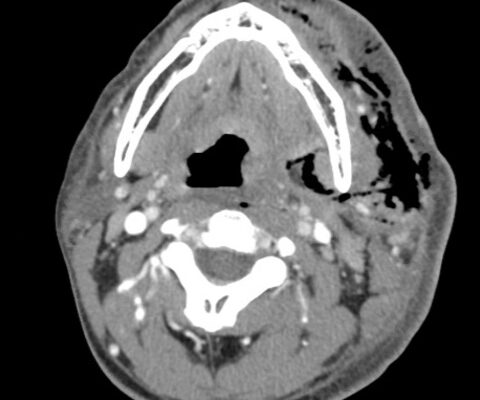
Necrotizing Fasciitis and Mediastinitis after Wisdom Tooth Extraction: A Case Report
DOI: https://doi.org/10.21980/J8XW7KComputer tomography (CT) imaging of soft tissues of the neck and of the chest/abdomen/pelvis revealed extensive swelling and subcutaneous air (see red arrows) on the left side of the face and neck extending to the left shoulder, as well as parapharyngeal/retropharyngeal spaces and posterior/superior mediastinum.
Improving Emergency Department Airway Preparedness in the Era of COVID-19: An Interprofessional, In Situ Simulation
DOI: https://doi.org/10.21980/J8V06MAt the conclusion of the simulation session, learners will be able to: 1) Understand the need to notify team members of a planned COVID intubation including: physician, respiratory therapist, pharmacist, nurse(s), and ED technician. 2) Distinguish between in-room and out-of-room personnel during high-risk aerosolizing procedures. 3) Distinguish between in-room and out-of-room equipment during high-risk aerosolizing procedures to minimize contamination. 4) Appropriately select oxygenation therapies and avoid high-risk aerosolizing procedures. 5) Manage high risk scenarios such as hypotension or failed intubation and be prepared to give push-dose vasoactive medications or place a rescue device such as an I-gel®.
A Case Report on Miliary Tuberculosis in Acute Immune Reconstitution Inflammatory Syndrome
DOI: https://doi.org/10.21980/J81H02A portable single-view radiograph of the chest was obtained upon the patient’s arrival to the ED resuscitation bay that showed diffuse reticulonodular airspace opacities (red arrows) seen throughout the bilateral lungs, concerning for disseminated pulmonary tuberculosis. Subsequently, a computed tomography (CT) angiography of the chest was obtained which again demonstrates this diffuse reticulonodular airspace opacity pattern (red arrows).
Necrotizing Fasciitis
DOI: https://doi.org/10.21980/J84M1DAt the conclusion of the simulation session, learners will be able to: 1) Describe the spectrum of clinical presentations of necrotizing fasciitis. 2) Identify the microbial etiology of necrotizing fasciitis. 3) Describe the empiric antibiotics appropriate for necrotizing fasciitis. 4) Describe benefits and limitations of various imaging studies when working up necrotizing fasciitis.
Primary Measles Encephalitis
DOI: https://doi.org/10.21980/J80S75At the conclusion of the simulation session, learners will be able to: 1) Obtain a relevant focused history, including immunization status, associated symptoms, sick contacts, and travel history. 2) Develop a differential for fever, rash, and altered mental status in a pediatric patient. 3) Discuss management of primary measles encephalitis, including empiric broad spectrum antibiotics and antiviral treatment. 4) Discuss appropriate disposition of the patient from pediatric emergency departments, community hospitals, and freestanding emergency departments, including appropriate time to call for transfer and the appropriate time to transfer this patient during emergency department (ED)workup. 5) Review types of isolation and indications for each.