Necrotizing Soft Tissue Infection
History of present illness:
A 71-year-old woman with a history of metastatic ovarian cancer presented with sudden onset, rapidly progressing painful rash in the genital region and lower abdominal wall. She was febrile to 103°F, heart rate was 114 beats per minute, and respiratory rate was 24 per minute. Her exam was notable for a toxic-appearing female with extensive areas of erythema, tenderness, and induration to her lower abdomen, intertriginous areas, and perineum with intermittent segments of crepitus without hemorrhagic bullae or skin breakdown.
Significant findings:
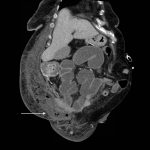
Computed tomography (CT) of the abdominal and pelvis with intravenous (IV) contrast revealed inflammatory changes, including gas and fluid collections within the ventral abdominal wall extending to the vulva, consistent with a necrotizing soft tissue infection.
Discussion:
Necrotizing fasciitis is a serious infection of the skin and soft tissues that requires an early diagnosis to reduce morbidity and mortality. Classified into several subtypes based on the type of microbial infection, necrotizing fasciitis can rapidly progress to septic shock or death if left untreated.1
Diagnosing necrotizing fasciitis requires a high index of suspicion based on patient risk factors, presentation, and exam findings. Definitive treatment involves prompt surgical exploration and debridement coupled with IV antibiotics.2,3 Clinical characteristics such as swelling, disproportionate pain, erythema, crepitus, and necrotic tissue should be a guide to further diagnostic tests.4 Unfortunately, lab values such as white blood cell count and lactate imaging studies have high sensitivity but low specificity, making the diagnosis of necrotizing fasciitis still largely a clinical one.4,5 CT is a reliable method to exclude the diagnosis of necrotizing soft tissue infections (sensitivity of 100%), but is only moderately reliable in correctly identifying such infections (specificity of 81%).5
Given the emergent nature of necrotizing fasciitis, prompt surgical evaluation is paramount. Emergent debridement is required (often revealing a characteristic “dishwater” pus) because even broad-spectrum antibiotics are not sufficient to completely resolve cases of necrotizing fasciitis.1
Topics:
Necrotizing soft tissue infection, computed tomography, sepsis, cellulitis.
References:
- Misiakos EP, Bagias G, Patapis P, Sotiropoulos D, Kanavidis P, Machairas A. Current Concepts in the Management of Necrotizing Fasciitis. Front Surg. 2014;1(36): eCollection. doi: 10.3389/fsurg.2014.00036
- Bilton BD, Zibari GB, McMillan RW, Aultman DF, Dunn G, McDonald JC. Aggressive surgical management of necrotizing fasciitis serves to decrease mortality: a retrospective study. Am Surg. 1998;64(5):397-400; discussion 400-401.
- Goh T, Goh LG, Ang CH, Wong CH. Early diagnosis of necrotizing fasciitis. Br J Surg. 2014;101(1): e119–25.doi: 10.1002/bjs.9371
- Goldstein EJ, Anaya DA, Dellinger EP. Necrotizing Soft-Tissue Infection: Diagnosis and Management. Clin Infect Dis. 2007;44(5):705–710.
- Murphy G, Markeson D, Choa R, Armstong A. Raised serum lactate: a marker of necrotizing fasciitis? J Plast Reconstr Aesthet Surg. 2013;66(12):1712-1716. doi: 10.1016/j.bjps.2013.07.008
- Zacharias N, Velmahos GC, Salama A, Alam HB, de Moya M, King DR, et al. Diagnosis of necrotizing soft tissue infections by computed tomography. Arch Surg. 2010;145(5):452-425. doi: 10.1001/archsurg.2010.50