Photograph
A Case Report on an Open Fracture Dislocation Injury of the Proximal Phalanx of the Thumb Resulting from Playing Cricket
DOI: https://doi.org/10.5070/M5.52278There was an open injury to the volar aspect of the right thumb at the interphalangeal joint, with exposed bone. There was no active bleeding from the wound. He had intact sensation to the entire thumb and hand. His radial pulse was normal with normal capillary refill in all digits of his right hand. He had intact wrist flexion, extension, abduction, and adduction; however, he was unable to flex or extend his thumb secondary to the injury. He had no other injuries to the rest of his right upper extremity. An x-ray was obtained which showed a right thumb proximal phalanx intra-articular fracture (proximal fracture fragment outlined in yellow, distal fracture fragment outlined in pink) at the interphalangeal joint with dorsal dislocation of the distal phalanx (outlined in red). There were no radiopaque foreign bodies.
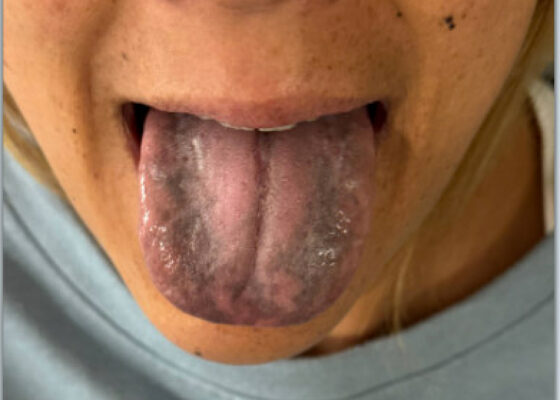
Woman with a Blackened Tongue: A Case Report
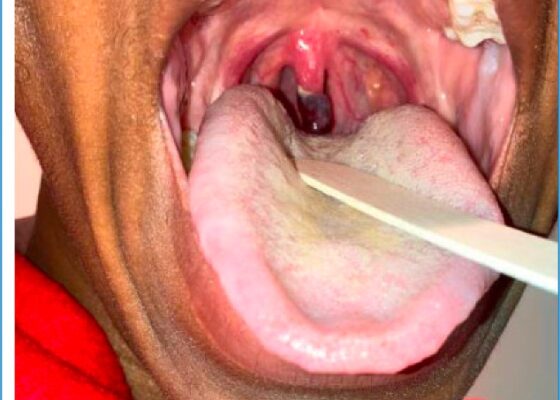
DOI: https://doi.org/10.5070/M5.52329The patient’s vital signs were blood pressure 109/72 mmHg, respiratory rate 18 breaths per minute, pulse 93 beats per minute, temperature 97°F. Physical examination revealed notable black discoloration of the tongue and gingiva, along with hyperpigmented skin exhibiting numerous diffuse nevi distributed across the face and upper extremities.
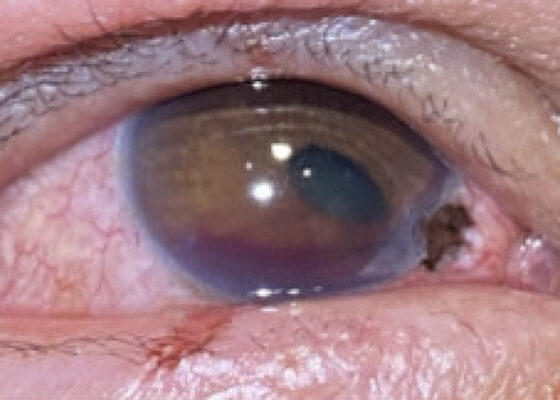
A Case Report of Corneoscleral Laceration with Open Globe Injury and Iris Prolapse
DOI: https://doi.org/10.5070/M5.52326Closer examination of the right eye revealed a 2 mm x 1 mm corneoscleral laceration to the 4-5 o'clock position at the border of zone I (yellow highlighting) and II (blue highlighting) with iris prolapse (yellow star) and plugging. Additionally, the affected eye revealed a peaked pupil (cyan highlighting) in the inferonasal direction with associated corectopia and a 2 mm Grade I hyphema (pink highlighting). Immediately inferior to the corneal laceration, 1 mm epithelial injury of the lower palpebra was present (green cross). Fluorescein exam demonstrated uptake at the 4-5 o'clock position (yellow arrow) but was negative for Seidel’s sign.
Diagnosis of Sinonasal Carcinoma in the Emergency Department: A Case Report Highlighting Red Flag Symptoms
DOI: https://doi.org/10.5070/M5.52257Physical exam revealed a gross deformity of the left side of the face with soft tissue swelling with no overlying skin changes. The left eye was proptotic and completely immobile, with cranial nerve (CN) 3, 4, and 6 palsies. Additionally, a large obstructive mass was noted in the left naris with resultant rightward displacement of the nasal septum. Intraocular pressures (IOPs) were measured to be 6 mmHg in the right eye and 11 mmHg in the left eye.
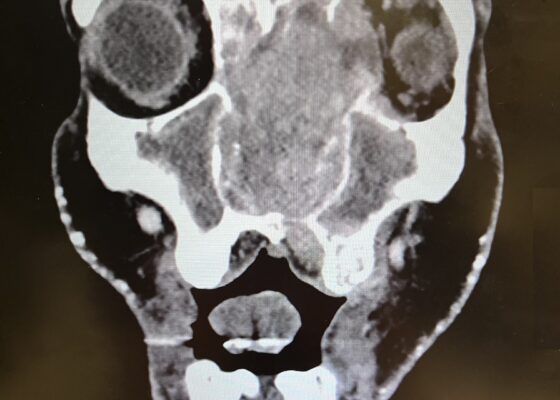
Imaging, including maxillofacial and neck soft tissue CTs revealed a large, destructive, soft tissue mass centered in the nasal cavity with significant osseous destruction of the midface and skull base (red highlighted area). There was mild intracranial extension with the mass abutting or infiltrating the inferior frontal lobes (green highlighted area). The nasal cavity and nasopharynx were obstructed (orange highlighted area). The mass invaded the left orbit with associated left-sided proptosis, left globe deformity, and compressed the left optic nerve and the left optic chiasm (blue arrows).
A Case Report of an Atypical Presentation of Fournier’s Gangrene
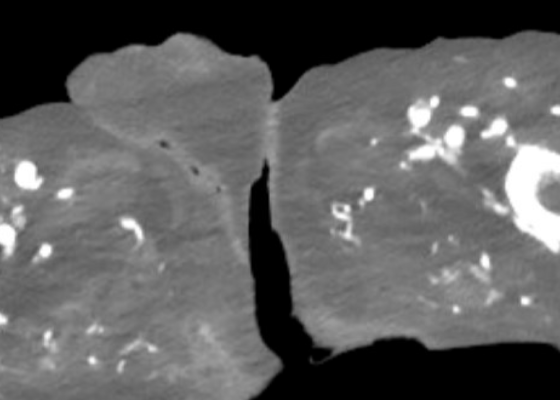
DOI: https://doi.org/10.5070/M5.52203A computed tomography (CT) scan of the abdomen and pelvis was significant for scrotal fluid and punctate gas locules (red arrow) without discrete evidence of invasion into the adjacent soft tissues, suspicious for Fournier’s gangrene. There was also fluid collection centered around the seminal vesicles suggestive of an abscess.
Case Report of a Dermatologic Reaction to Wound Closure Strips and Liquid Adhesive
DOI: https://doi.org/10.21980/J8.52256The patient removed the splint, and the wound were notable for erythematous bullae (blue arrow), blisters (yellow arrow), and skin maceration (red arrow) in the distribution under the wound closure strips. Of note, there was no surrounding erythema with poorly defined borders.
Case Report of Post-Operative Uvular Necrosis Following Intubation
DOI: https://doi.org/10.21980/J8065JThe distal portion of her uvula was necrotic with a clear demarcation approximately halfway up the uvula. She had no trauma to the anterior oropharyngeal structures, tonsils, or adenoids. There were no lesions to the hard or soft palate. She had no carotid bruits or thrills, and no tenderness over the anterior portion of the neck.
Case Report: Iatrogenic Bowel Perforation Following Dental Procedure
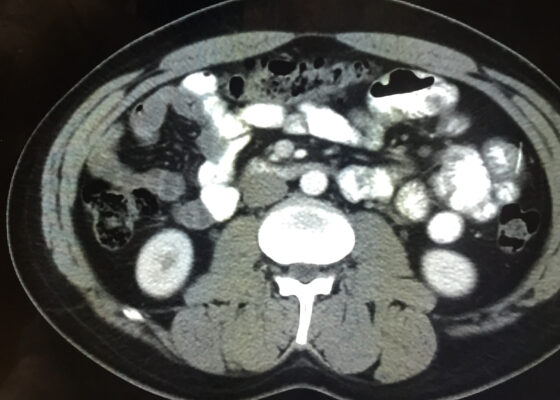
DOI: https://doi.org/10.21980/J8CD38The patient’s abdominal CT demonstrated a metallic foreign body in the left side of the abdomen within the small bowel, without surrounding induration or abscess. Radiology questioned whether the metallic foreign object perforated the bowel. Seen in the cross-sectional CT image, there is a hyperdense linear structure transversing the small intestinal wall, given that a portion of the structure was located outside of the lumen of the bowel.