Issue 3:3
Novel Emergency Medicine Curriculum Utilizing Self-Directed Learning and the Flipped Classroom Method: Cardiovascular Emergencies Small Group Module
DOI: https://doi.org/10.21980/J8X334We aim to teach the presentation and management of cardiovascular emergencies through the creation of a flipped classroom design. This unique, innovative curriculum utilizes resources chosen by education faculty and resident learners, study questions, real-life experiences, and small group discussions in place of traditional lectures. In doing so, a goal of the curriculum is to encourage self-directed learning, improve understanding and knowledge retention, and improve the educational experience of our residents.
The Continuous Residency Improvement Committee (CRIC) – A Novel Twist for Program Evaluation in an Academic Emergency Medicine Residency Program
DOI: https://doi.org/10.21980/J8SD17The purpose of this innovation was to develop a novel approach to continuous program evaluation and improvement using a multisource feedback design to improve resident satisfaction with the program’s responsiveness to feedback while addressing the ACGME mandate for self-study.
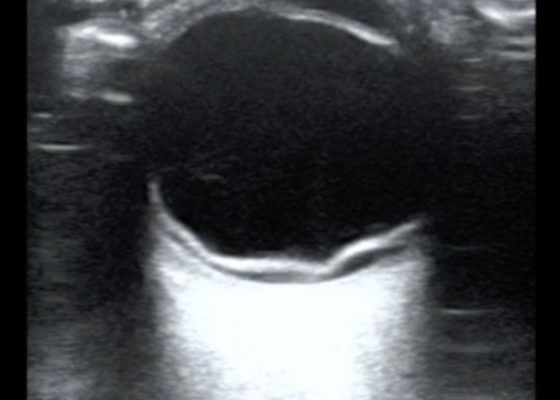
Realistic and Inexpensive Ultrasound Guided Paracentesis Simulator Using Pork Belly with Skin
DOI: https://doi.org/10.21980/J8NK9RBy the end of this instructional session learners should be able to: 1) Discuss the indications, contraindications, and complications associated with abdominal paracentesis; and 2) competently perform an ultrasound-guided abdominal paracentesis on a simulator and remove fluid.
Low Cost Task Trainer for Neonatal Umbilical Catheterization
DOI: https://doi.org/10.21980/J8HW6GBy the end of this instructional session learners should: 1) Discuss the indications, contraindications, and complications associated with umbilical catheterization. 2) Competently perform umbilical catheterization on the task trainer. 3) Demonstrate proper securement of the catheter.
A Low Cost Escharotomy Simulation Model for Residency Education
DOI: https://doi.org/10.21980/J8D34VBy the end of this educational session, the learner will be able to: 1) Understand the indications for an escharotomy. 2) List equipment needed to perform an escharotomy. 3) Demonstrate how to perform an escharotomy. 4) Perform an escharotomy and experience the sensation of cutting through simulated burned tissue. 5) Understand post-escharotomy management and referral to specialist.
Acute Hemolytic Transfusion Reaction
DOI: https://doi.org/10.21980/J88D2ZBy the end of this simulation session, the learner will be able to: 1) Recognize the clinical signs and symptoms associated with transfusion reactions. 2) Discuss necessary systems-based management of potential transfusion reactions, such as notifying the blood bank and evaluating to see if another patienta accidentally received a wrong unit of blood. 3) Discuss the management of various transfusion reactions. 4) Appropriately disposition the patient to an intensive care unit (ICU) or stepdown unit. 5) Effectively communicate with team members and nursing staff during the resuscitation of a critically ill patient.
In-Flight Emergency: Altered Mental Status Secondary to Hypoglycemia
DOI: https://doi.org/10.21980/J84M01By the end of this simulation session, learners will be able to: 1) Discuss the challenges associated with in-flight emergencies. 2) List what is available in United States (US) commercial airline medical kits. 3) Discuss an appropriate differential diagnosis for a patient with altered mental status (AMS). 4) Demonstrate appropriate treatment of hypoglycemia. 5) Describe possible complications in diabetic patients with insulin pumps when flying. 6) Review the legal ramifications of responding to an in-flight emergency.
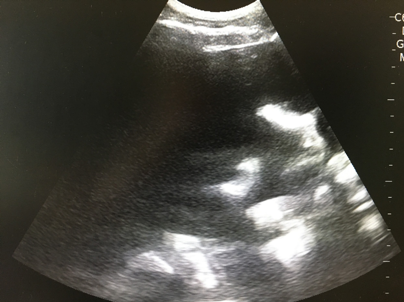
Bedside Ultrasound of Retinal Detachment in a 19-year-old
DOI: https://doi.org/10.21980/J80W6TThe ocular point of care ultrasound (POCUS) utilizing a high frequency linear probe shows a retinal detachment (RD) with a thick, hyperechoic undulating membrane in the vitreous humor that is anchored at the ora serrata anteriorly and the optic disc posteriorly. Note that the retina is detached all the way to the optic disc making it "mac off." The macula, and more specifically the fovea, is located in the central retina and contains a high concentration of cone photoreceptors responsible for central, high resolution, color vision. In a "mac on" RD, the retina detaches in the periphery but remains intact centrally. This is an ophthalmologic emergency and timely diagnosis and intervention can be vision saving. This patient also has evidence of a posterior vitreous hemorrhage which has a characteristic swirling appearance with kinetic exam on real-time imaging. The detached vitreous body is not as well defined and is not anchored posteriorly to the optic disc.