Latest Articles
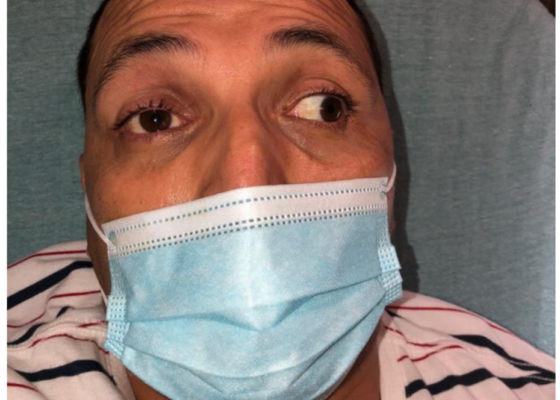
Case Report of a Man with Right Eye Pain and Double Vision
DOI: https://doi.org/10.21980/J8KW7GABSTRACT: A 39-year-old previously healthy male presented with three days of right eye pressure and one day of binocular diplopia. He denied history of trauma, headache, or other neurological complaints. He had normal visual acuity, normal intraocular pressure, intact convergence, and no afferent pupillary defect. His neurologic examination was non-focal except for an inability to adduct the right eye past midline
The Zipperator! A Novel Model to Simulate Penile Zipper Entrapment
DOI: https://doi.org/10.21980/J8NS8FAfter training on the Zipperator, learners will be able to: 1) demonstrate at least two techniques for zipper release and describe how methods would extrapolate to a real patient; 2) verbalize increased comfort with the diagnosis of zipper entrapment; and 3) present a plan of care for this low-volume, high-anxiety presentation.
Two-Screen Virtual Board Game Didactic for Teaching Wilderness and Environmental Medicine Topics to Emergency Medicine Residents
DOI: https://doi.org/10.21980/J8J343By the end of this didactic, the learner will: 1) describe the basics of the presentation of each topic listed above; 2) recall the basics of management of each topic listed above; and 3) improve learners’ preparedness for the Emergency Medicine Inservice Exam and Written Board Examination
Working with Senior Residents: How to get past “You’re doing great!”
DOI: https://doi.org/10.21980/J8D93JABSTRACT: Audience: This content is intended for emergency medicine faculty. Introduction: Faculty at our institution noted that it can be easy to identify and address the knowledge gaps of junior learners. However, they often find different skills are needed when precepting senior residents, a sentiment shared by faculty at other institutions.1 To foster the skills needed for lifelong learning and
Small-Scale High-Fidelity Simulation for Mass Casualty Incident Readiness
DOI: https://doi.org/10.21980/J84S8SThe learners will (1) recognize state of mass casualty exercise as evidenced by verbalization or triaging by START (Simple Triage and Rapid Treatment) criteria, (2) triage several patients, including critically ill or peri-arrest acuities, according to START criteria, (3) recognize the need to limit care based on available resources, as evidenced by verbal orders or communication of priorities to team, and (4) limit emergency resuscitation, given limited resources, by only providing treatments and employing diagnostics that do not deplete limited time, staffing, and space inappropriately.
Cardiac Arrest in an Adolescent with Pulmonary Embolism
DOI: https://doi.org/10.21980/J8135TABSTRACT: Audience: The target audience of this simulation is emergency medicine residents and medical students. The simulation is based on a real case of a 13-year-old female who presented with seizures and hypoxia and was ultimately diagnosed with pulmonary embolism. The case highlights diagnosis and management of an adolescent with new onset seizures, deterioration in status, and treatment options in
Spontaneous Coronary Artery Dissection Causing Cardiac Arrest in a Post-Partum Patient – A Case Report
DOI: https://doi.org/10.21980/J8F947A post-ROSC electrocardiogram revealed ST elevations in leads I, aVL, and V3-V6, with reciprocal ST depressions in leads II, III, and aVF. Initial troponin I level was 0.238 ng/mL and a bedside cardiac ultrasound revealed decreased motion of the anterior wall. Cardiology was consulted and the patient was immediately taken to the catheterization lab where she was found to have long and diffuse luminal narrowing of her distal left anterior descending artery (LAD) resulting in 70% stenosis, consistent with the angiographic appearance of an intramural hematoma caused by dissection (white arrows). No intervention was performed.
A Boy with Rash and Joint Pain Diagnosed with Scurvy: A Case Report
DOI: https://doi.org/10.21980/J89H1XHis lower extremity magnetic resonance imaging (MRI) findings showed abnormal signals in his knees, which were most consistent with scurvy. The white arrows on the T1-weight sequence indicate hypointensity (decreased signal or darker region) of the knees. The white arrows in the T2-weighted short-tau inversion recovery (STIR) sequence indicate hyperintensity (increased signal or brighter region) in an MRI of the knees.
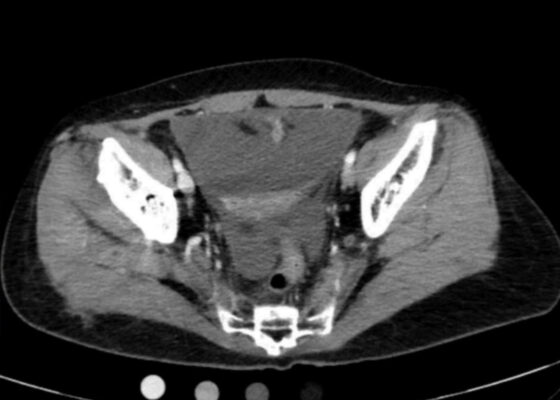
An Atraumatic, Idiopathic Case Report of Intraperitoneal Bladder Dome Rupture
DOI: https://doi.org/10.21980/J85S83On regular CT scan imaging, the urinary bladder is partially distended with contrast with no focal wall thickening or intraluminal hematoma. There is an intraperitoneal bladder rupture with site of rupture likely at the dome of the bladder. The bladder is outlined in red, and the bladder rupture boundaries are outlined in yellow, showing the urine as free fluid escaping into the intraperitoneal space. We also provide these findings in an axial CT in video format. On CT cystography, there is a significant amount of contrast-enhanced urine noted within the visualized peritoneal spaces. The small amount of air present anteriorly is related to the catheterization because a Foley balloon is present within the bladder. These findings are annotated with the peritoneal spaces outlined in yellow, the air in the blue outline, and the bladder in the red outline. All of these CT cystography findings are also presented in an axial view in video format.
Ureteral Obstruction and Ureteral Jet Identification—A Case Report
DOI: https://doi.org/10.21980/J8206GA point-of-care ultrasound of the urinary tract was performed, evaluating the kidneys and bladder. When imaging her kidneys, right-sided hydronephrosis was noted with a normal appearance to the left kidney. To further evaluate, a curvilinear probe was placed on her bladder with color doppler to assess for ureteral jets. Ureteral jets are seen as a flurry of color ejecting from each of the ureters as urine is released from the ureterovesical junction. In a healthy patient, this finding should be seen ejecting from both ureters every 1-3 minutes as the kidneys continue to filter the blood and create urine to be stored in the bladder. In our patient, however, ureteral jets were only noted on the left side (arrow), which was significant in further verifying our suspicion of right ureteral obstruction.