Peritonsillar Abscess Simulator: A Low-Cost, High-Fidelity Trainer
ABSTRACT:
Audience:
Our reusable low-cost peritonsillar abscess simulator (PTA) simulator is designed to train emergency medicine (EM) residents, fellows, and medical students. Trainees who are interested in otolaryngology (OTL) or this specific disease may also benefit from this simulator.
Introduction:
Peritonsillar abscess is one of the most common deep infections1 of the head and neck, accounting for 7589 consultations and 11069 hospital bed days in the UK between 2009-2010.1,2 Emergency medicine physicians commonly treat this pathology with surgical and medical modalities. Not only is this a common diagnosis, but there is a significant cost associated with the evaluation and management of primary PTA. 3
Demands for high-volume patient care and good patient outcomes are increasing in a medical climate of limited financial resources and resident work hours. Given these complexities, medical education is viewing simulation training, with proven success in various surgical specialties, as a valuable addition to resident education and patient safety.3-5
The PTA is the collection of pus in the space between the palatine tonsil and its capsule. Successfully locating the abscess is crucial because it prevents the unwanted damage of nearby vascular structures, patient discomfort, and failure to treat the infection. Management of peritonsillar abscess is primarily surgical and includes incision and drainage (I & D), needle aspiration, or Quinsy tonsillectomy.
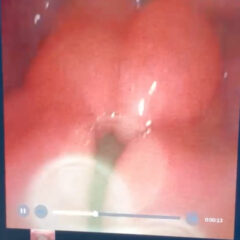
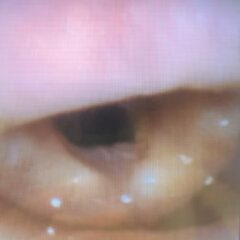
The simulator provides a realistic characteristic of typical PTA presentations, such as uvula deviation, swelling, trismus, and purulence during aspiration.
While learning to drain a PTA, trainees must locate the infection with a needle without injury to the surrounding structures of the oral cavity and deep structures of the neck. The discomfort caused during this procedure can be unsettling for both physician and patient. Simulation use and testing enable the trainee to develop familiarity with handling instruments, increase comfort with the sequence of a procedure, and improve confidence in the ability to perform a procedure safely.6,7,8 Simulators provide improved patient outcomes and increased EM residents’ comfort level.
Educational Objectives:
By the end of this training session, learners will be able to: 1) locate the abscess, 2) perform needle aspiration, and 3) develop dexterity in maneuvering instruments in the small three-dimensional confines of the oral cavity without causing injury to local structures.
Educational Methods:
Our PTA simulator was fabricated with a low-cost, non-degradable material and is the first known PTA simulator that used a validated survey for fidelity assessment. The simulator was fabricated using a silicone mold to mimic the oral cavity and oropharynx. A simulated abscess pocket consisting of saline encased in balloon material was placed in the proper anatomic location, allowing for abscess simulation on either side of the oropharynx model. The time to fabricate the model averaged 20 hours. The simulator was manufactured with low-cost materials at an expense of 45 USD and could be easily reproduced by any EM residency program.
Research Methods:
Twenty-one participants were instructed to expose and drain the simulated abscess. The model was evaluated using The Michigan Standard Simulation Experience Scale (MiSSES).7 Participants scored the simulator in five categories: Self-efficacy, fidelity, educational value, teaching quality, and the overall rating on a 5-point Likert scale of simulator. Overall rating and global evaluation scores were compared by groups (Group 1, Group 2) between training level (residents and attendings), specialty (emergency and otolaryngology), and previous experience (<5 or ≥5 drainages).
Convenience sampling was used to determinate the sample. Variables were summarized using the mean and standard deviation for continuous variables and percentages and frequencies for categorical variables. The MiSSES was scored as previously described in the literature.7 The Kolmogorov-Smirnov test was used to test for normal distribution of the variables. T-test for independent samples was performed to determinate if there exists a difference between groups in perception of a PTA simulator. The statistical analyses were performed using SPSS version 20.0 Armonk, NY: IBM.
Results:
Twenty-one participants were enrolled in the study: residents (n=15) and attending (n=6) from OTL and EM departments. The simulator’s plasticity allowed multiple attempts of needle aspiration and drainage without degradation and received high ratings on teaching quality, fidelity, and educational value. This PTA simulator achieved high fidelity ratings in the standard simulator`s assessment survey for realism of environment, simulation of trismus, uvular deviation, and realism of the mucosal surfaces.
On the MiSSES, the model received positive ratings (range 3.6 to 4.9). The highest rating was on teaching quality (4.9), fidelity (4.6), and educational value (4.5) (Table 1). We found that self-efficacy and teaching quality sections were rated higher for those who had less experience (≥5 PTA drainage), while fidelity was rated higher for OTL. The overall rating average was 4 and was higher of attendings, OTL, and those with less experience. All comparisons between groups were not statically significant (Table 2). About 76% of participants found that the simulator can be used in training with slight improvement or no improvement needed. (Table 3)
Discussion:
With favorable participant ratings and comments, we believe that this tool can offer high-fidelity simulation at a low cost. Widespread use may be possible, allowing training of EM residents in performing instrumentation of PTA in a controlled simulation environment. We have created a reusable low-cost PTA simulator that achieved a high score fidelity in a standard simulator`s assessment survey.
Topics:
Peritonsillar abscess, oropharynx, emergency medicine residency, otolaryngology residency training.