Viridans streptococci Intracranial Abscess Masquerading as Metastatic Disease
History of present illness:
A 64-year-old woman with a remote history of breast cancer presented to the emergency department with one day of worsening right-sided weakness and headaches. She had been seen two weeks prior for similar symptoms and underwent unenhanced brain computed tomography (CT), which revealed a left parietal mass suspected to represent new metastatic disease. The patient presented on this visit not only with weakness of her right upper and lower extremity, but was found to be febrile, tachycardic and exhibiting lethargy. Peripheral white blood cell count (WBC) was 27.1 (x103/mm3). Given her rapidly declining clinical course and expected time to complete magnetic resonance imaging (MRI) of the brain, the decision was made to first perform an emergent contrast-enhanced brain CT to further evaluate the mass. The contrast-enhanced brain CT revealed a large rim-enhancing left parietal lesion.
Significant findings:
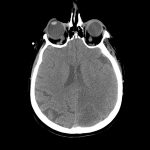
A non-contrast CT (Figure 1) revealed a large hypoattenuating left parietal lesion. When the CT was enhanced with intravenous contrast (Figure 2), the same lesion showed peripheral rim enhancement, suggestive of a brain abscess.
Discussion:
Intracranial abscess is a rare yet potentially devastating disease process that can often be difficult to diagnosis, with an incidence of about 0.4-0.9 cases per 100,000 people.1 Mortality rates are about 15% within the past decade, but can increase up to 85% if the abscess ruptures. The most common mechanisms for formation of intracranial abscesses include direct spread from local infections (odontogenic infections or sinusitis), hematogenous spread (congenital heart disease, endocarditis, dental procedures, or intrapulmonary shunting), or penetrating trauma.2 Intracranial abscesses are more likely to occur in severely immunosuppressed patients, after neurosurgical procedures, or in head trauma. About 32%-60% of brain abscesses are polymicrobial, but Viridans streptococci, a group of aerobic gram-positive cocci, is one of the most commonly isolated microorganisms, especially from intraoral sources.3,4 The most common presenting symptom in patients is a headache, and the classic triad of headache, fever, and focal neurologic deficits is present in only about 20% of cases.5 Neurologic findings often take days to weeks to manifest and will vary based on the location of the abscess. Up to 25% of patients will also present with seizures.1
Classic CT features favoring an abscess include a continuous thin rim of peripheral enhancement and thinning along the medial wall.6 However, these are nonspecific and frequently difficult to differentiate from high-grade neoplasms, metastases, infarcts, or hematomas. MRI with gadolinium is therefore significantly more sensitive and specific for diagnosing and differentiating a brain abscess from primary or metastatic cancer. Prospective studies report a sensitivity and specificity of about 96% for MRI when combined with diffusion-weighted imaging.1,5
In this case, the patient underwent operative stereotactic drainage of the lesion. A biopsy was negative for malignancy, but bacterial cultures grew Viridans streptococci. Additional imaging of the chest revealed a large pulmonary arteriovenous malformation as the suspected etiology for the abscess. The patient was treated with intravenous vancomycin and ceftriaxone and ultimately discharged to rehabilitation for physical therapy.
Topics:
Brain abscess, Viridans streptococci, computed tomography, CT, magnetic resonance imaging, MRI.
References:
- Brouwer MC, Tunkel AR, McKhann GM, van de Beek D. Brain abscess. N Engl J Med. 2014;371(5):447-456. doi: 10.1056/NEJMra1301635
- Brook I. Microbiology and treatment of brain abscess. J Clin Neurosci.2017;38:8-12. doi: 10.1016/j.jocn.2016.12.035
- Moazzam AA, Rajagopal SM, Sedghizadeh PP, Zada G, Habibian M. Intracranial bacterial infections of oral origin. J Clin Neurosci.2015; 22(5):800-806. doi: 10.1016/j.jocn.2014.11.015
- Prasad KN, Mishra AM, Gupta D, Husain N, Husain M, Gupta RK. Analysis of microbial etiology and mortality in patients with brain abscess. J Infection. 2006;53(4):221-227. doi: 10.1016/j.jinf.2005.12.002
- Dorsett M, Liang SY. Diagnosis and treatment of central nervous system infections in the emergency department. Emerg Med Clin N Am. 2016;34(4):917-942. doi: 10.1016/j.emc.2016.06.013
- Rath TJ, Hughes M, Arabi M, Shah GV. Imaging of cerebritis, encephalitis, and brain abscess. Neuroimag Clin N Am. 2012;22(4):585-607. doi: 10.1016/j.nic.2012.04.002