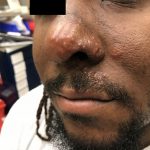
Hutchinson’s Sign
History of present illness:
A 30-year-old African American male presents with two days of gradually worsening vesicular pruritic rash over the left naris, left upper lip, and inferior to medial epicanthus, initially noted just on the upper lip the night before. By the next day it had spread to the nose and cheek. Patient denies any fever, pain, discharge from the rash, ear or nose, or changes in vision. He denies exposure to any new hygiene products, household cleaning products, recent outdoor activities, travel, or insect bites. Past medical history significant for a childhood varicella infection. Patient works for a moving company, and had an episode of heat exhaustion at work one week prior to onset. Denies alcohol or drug abuse.
Significant findings:
The unilateral distribution of vesicular lesions over the patient’s left naris, cheek, and upper lip are consistent with Herpes zoster reactivation with Hutchinson’s sign. Hutchinson’s sign is a herpes zoster vesicle present on the tip or side of the nose.1 It reflects zoster involvement of the 1st branch of the trigeminal nerve, and is concerning for herpes zoster ophthalmicus.1 Herpes zoster vesicles may present as papular lesions or macular vesicles on an erythematous base.2,3 Emergent diagnosis must be made to prevent long-term visual sequelae.4
Discussion:
The history of a childhood viral exanthem, specifically a past varicella infection, helps direct the diagnosis.2 Herpes zoster ophthalmicus is an ophthalmological emergency and results from viral reactivation within the V1 branch of CN V, leading to direct ocular involvement.1 Symptoms of ocular involvement include red eye, blurry vision, eye pain or photophobia.1 If left untreated, corneal ulceration, scarring, perforation, glaucoma, cataracts, and blindness may occur.1 Fluorescein staining with slit lamp examination will show a characteristic “dendritic ulcer” within the epithelial layer of the cornea.1 Treatment is generally with oral acyclovir (800mg five times daily for 7-10 days) or valacyclovir (1,000 mg three times daily for 7-14 days) and close ophthalmology follow-up.3 If patients have disease in multiple dermatomes, underlying immunosuppression, orbital, optic nerve, or cranial nerve involvement, they should be admitted for treatment with IV acyclovir (10mg/kg, three times per day, for seven days) and ophthalmologic consult.1
Topics:
Herpes zoster ophthalmicus, Hutchinson’s sign, emergency management.
References:
- Walker RA, Srikar A. Eye emergencies. In: Tintinalli JE, Stapczynski J, Ma O, Cline DM, Cydulka RK, Meckler GD, eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 8th New York, NY: McGraw-Hill; 2016:1543-1578.
- Schmader KE, Oxman MN. Varicella and herpes zoster. In: Goldsmith LA, Fitzpatrick TB, eds. Fitzpatrick’s Dermatology in General Medicine. 8th New York, NY: McGraw-Hill ;2012:2383-2401.
- Andrus P, Guthrie J. Acute peripheral neurologic disorders. In: Tintinalli JE, Stapczynski J, Ma O, Yealy DM, Meckler GD, Cline DM. eds. Tintinalli’s Emergency Medicine: A Comprehensive Study Guide. 8th New York, NY: McGraw-Hill; 2016: 1178-1185.
- Nithyanandam S, Stephen J, Joseph M, Dabir S. Factors affecting visual outcome in herpes zoster ophthalmicus: a prospective study. Clin Exp Ophthalmol. 2010;38(9):845-850. doi: 10.1186/s12348-014-0025-9