Neurology
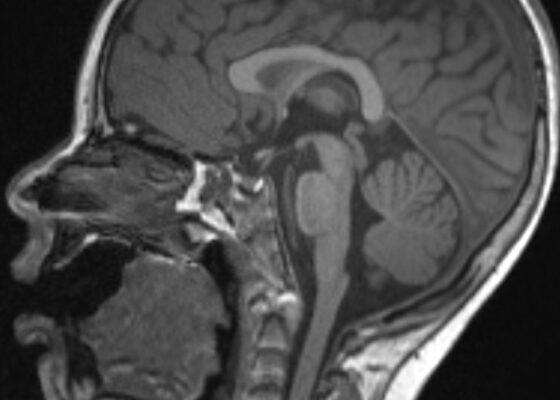
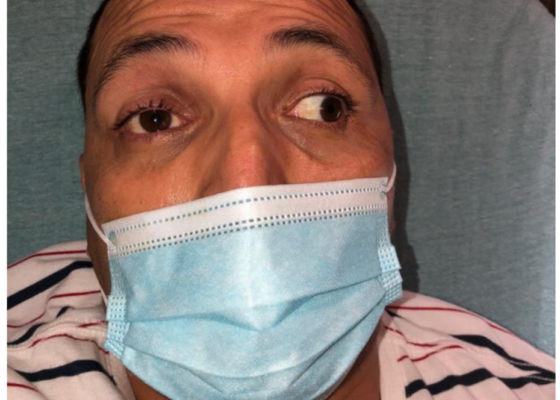
The Clue is in the Eyes. A Case Report of Internuclear Ophthalmoplegia
DOI: https://doi.org/10.21980/J8DP9MThere was no appreciable esotropia or exotropia noted on straight gaze (yellow arrows). On extraocular muscle examination, patient was noted to have a complete left medial rectus palsy consistent with a left internuclear ophthalmoplegia (red arrow). This was evidence by both eyes easily gazing left (green arrows); however, with rightward gaze, her left eye failed to gaze past midline (red arrow).
Headache Over Heels: CT Negative Subarachnoid Hemorrhage
DOI: https://doi.org/10.21980/J8ND2CBy the end of this case, the participant will be able to: 1) construct a broad differential diagnosis for a patient presenting with syncope, 2) name the history and physical exam findings consistent with SAH, 3) identify SAH on computer tomography (CT) imaging, 4) identify the need for lumbar puncture (LP) to diagnose SAH when CT head is non-diagnostic > 6 hours after symptom onset, 5) correctly interpret cerebral fluid studies (CSF) to aid in the diagnosis of SAH, and 6) specify blood pressure goals in SAH and suggest appropriate medication management.
Epilepsy Caused by Neurocysticercosis: A Case Report
DOI: https://doi.org/10.21980/J81P96In our patient, two lesions were most notable on CT in the frontal and occipital lobes. The lesion in the left frontal lobe (blue circle) was an approximately 1.5 centimeter (cm) rounded area with rim enhancement and surrounding hypodensity, consistent with vasogenic edema. A similar sized low-density area in the left occipital lobe (red circle) was noted, with increased peripheral density at the 3 o’clock position representing calcification. There were no areas of apparent hemorrhage or midline shift. The final radiology report concluded there were multiple cystic lesions, one with surrounding vasogenic edema in the left frontal lobe.
A Case Report of a Man with Burning Arm and Leg Weakness
DOI: https://doi.org/10.21980/J8V659A non-contrast computed tomography (CT) of the head and neck was performed, followed by an MRI of the cervical spine. The CT demonstrated congenital narrowing of the cervical spinal canal, with posterior disc osteophyte complex and disc bulge at C3-4 and C4-5 (arrow). The T2-weighted MRI additionally demonstrated obliteration of the anterior and posterior subarachnoid space at the level of C3-C5, with associated patchy central cord signal abnormality (arrow).
Transverse Myelitis in Naloxone Reversible Acute Respiratory Failure—A Case Report
DOI: https://doi.org/10.21980/J8B659Magnetic resonance imaging of the brain, cervical, thoracic and lumbar spine without contrast was obtained and revealed increased signal throughout the spinal cord from C-1 to the conus medullaris with mild expansion consistent with transverse myelitis.
An Unusual Case Report of a Toddler with Metastatic Neuroblastoma Mimicking Myasthenia Gravis
DOI: https://doi.org/10.21980/J8G35VWhile still in the ED, MRI with and without gadolinium contrast of the brain, orbits, and cervical, thoracic and lumbar spine were obtained to evaluate for possible CNS lesions including encephalitis, myelitis, or demyelination. Imaging, however, demonstrated multiple unexpected findings: a T1 hypointense, T2 hyperintense and heterogeneously enhancing right adrenal mass measuring 2.7 x 2.1 x 3 cm (yellow asterisk) along with heterogenous enhancement at the clivus, C6, C7, T7, T8, T12, and L3 vertebral bodies (red asterisks). There were otherwise no significant intracranial signal or structural abnormalities and normal orbits.
Case Report of a Man with Right Eye Pain and Double Vision
DOI: https://doi.org/10.21980/J8KW7GABSTRACT: A 39-year-old previously healthy male presented with three days of right eye pressure and one day of binocular diplopia. He denied history of trauma, headache, or other neurological complaints. He had normal visual acuity, normal intraocular pressure, intact convergence, and no afferent pupillary defect. His neurologic examination was non-focal except for an inability to adduct the right eye past midline