ENT
A Low-Cost Facial and Dental Nerve Regional Anesthesia Task Trainer
DOI: https://doi.org/10.21980/J8RP9QBy the end of this educational session, learners should be able to: 1) describe and identify relevant anatomy for supra-orbital, infra-orbital, mental, and inferior alveolar nerves and 2) successfully demonstrate supra-orbital, infra-orbital, mental, and inferior alveolar nerve blocks using a partial task trainer.
Auricular Perichondritis after a “High Ear Piercing:” A Case Report
DOI: https://doi.org/10.21980/J8WH16On physical examination, there was erythema, swelling, warmth, and general exquisite tenderness of the superior aspect of the left pinna (the outer ear) but excluding the ear canal, lobe, tragus, and crus. There was no facial involvement. There was no fluctuance about the ear and no drainage of fluid. The preauricular lymph nodes were enlarged and tender, but the anterior cervical lymph nodes were not tender. There was no mastoid tenderness, protrusion of the ear, or interruption of the postauricular crease.
Peritonsillar Abscess Model for Ultrasound Diagnosis Using Inexpensive Materials
DOI: https://doi.org/10.21980/J86G9PBy the end of this instructional session learners should be able to: 1) identify and discuss the indications, contraindications, and complications associated with peritonsillar abscesses, 2) properly identify and measure a PTA through ultrasound, and 3) competently perform ultrasound-guided peritonsillar abscess drainage on a simulator and remove fluid.
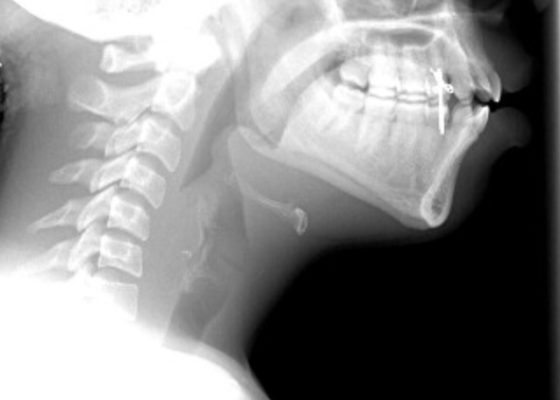
Case Report: Acute Supraglottitis
DOI: https://doi.org/10.21980/J8006VOn arrival, radiographs of the neck soft tissues were obtained, which showed a markedly enlarged epiglottic shadow (red arrow) concerning for epiglottitis. A computed tomography scan of the neck soft tissues with contrast was then obtained which revealed edematous mucosal thickening of the oropharynx (blue arrow) and supraglottic larynx (green arrow) including the epiglottis (purple arrow) concerning for acute infectious pharyngitis and supraglottic laryngitis with severe narrowing of the supraglottic laryngeal lumen, as well as associated extensive inflammation and edema of the superficial and deep left neck spaces. The patient’s white blood cell count was elevated to 25.7x109/L with 87% neutrophils. Her rapid strep test was positive. Otolaryngology was consulted and performed a bedside flexible laryngoscopy which showed significant edema of the epiglottis (orange arrow), vocal cords (white arrow), and arytenoids (black arrow), left greater than right. Based on the findings and concern for impending respiratory failure, the patient received an awake fiberoptic intubation by anesthesia at the bedside.
Abdominal Pain with Black Tongue
DOI: https://doi.org/10.21980/J8XS7JPatient’s tongue had a black discoloration, without elongated filiform papillae. We could not appreciate lymphadenopathy. His abdomen was tender to palpation.
Facial Fracture Induced Periorbital Emphysema
DOI: https://doi.org/10.21980/J8F05HPhysical exam showed marked left palpebral subcutaneous crepitus, as well as bulbar and palpebral conjunctival bulging. Visual acuity was normal with intact extraocular movements, and normal pupillary exam. Computed tomography (CT) imaging of the face was obtained and revealed multiple displaced fractures involving the left orbital floor and zygomatic arch associated with moderate periorbital and postseptal extraconal gas, resulting in orbital proptosis.
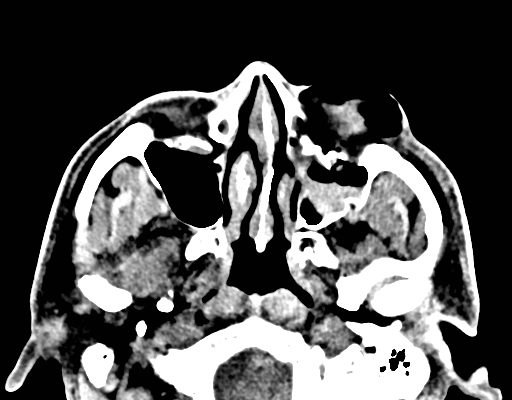
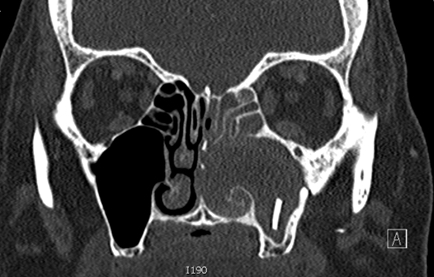
Foreign Body in Maxillary Sinus: A Rare Case of Chronic Rhinosinusitis
DOI: https://doi.org/10.21980/J85H09Computed tomography (CT) sinus with contrast demonstrated complete opacification of left paranasal sinuses and nasal cavity, and a linear radiopacity within the left maxillary sinus consistent with a foreign body. There were additional left facial subcutaneous radiopaque opacities.
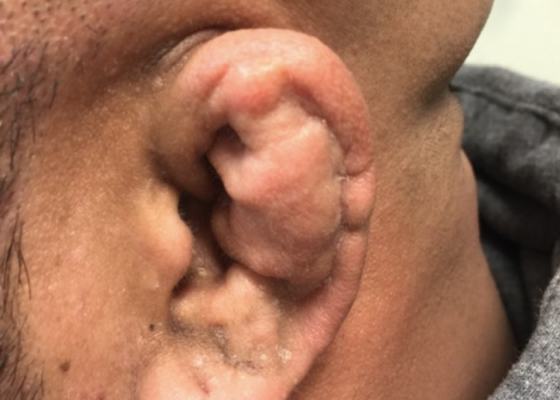
Cauliflower Ear Secondary to a Chronic Auricular Hematoma
DOI: https://doi.org/10.21980/J8S63XOn exam, the patient has a gross deformity to the left pinna that was not painful to touch or fluctuant. Findings and history are consistent with cauliflower ear, secondary to a chronic auricular hematoma.