Atypical Presentation of Abdominal Aortic Aneurysm
History of present illness:
An 84-year-old male with a past medical history of congestive heart failure, hypertension, nonischemic cardiomyopathy, chronic obstructive pulmonary disease, cerebral vascular accident, chronic kidney disease, and known thoracic aortic aneurysm (TAA) presented to the emergency department (ED) with complaints of malaise, dyspnea on exertion, and worsening bilateral lower extremity edema. He was recently seen by his nephrologist and told he had a worsening creatinine.
Significant findings:
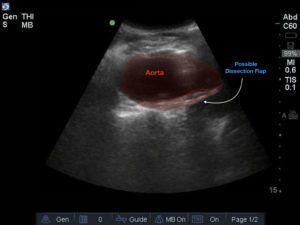
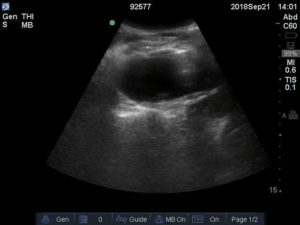
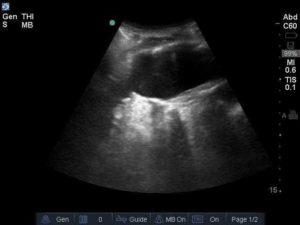
Bedside ultrasound revealed an abdominal aortic aneurysm (AAA) with concern for dissection vs thrombus/hematoma due to an area of echogenicity within the lumen of the vessel, since normal blood vessels (including the aorta) have lumens that are uniformly anechoic. An intimal flap concerning for dissection appears as a hyperechoic stripe within the lumen of the vessel on ultrasound, often with a hypoechoic and/or anechoic area appreciated underneath the flap, indicating a separate area of blood flow. If this visualized area is of significant size, color doppler can be used to confirm blood flow on both sides of the flap. Given his bedside ultrasound findings, the patient underwent emergent computed tomography scan and was found to have an enlarged infrarenal abdominal aortic aneurysm, with acute intramural hematoma, extending into bilateral common iliac arteries.
Discussion:
An abdominal aortic diameter greater than 3.0 cm is classically defined as an AAA. Risk factors associated with developing a AAA include male sex, smoking, advanced age and a positive family history.1,2 Furthermore, given that approximately 25 percent of patients with thoracic aortic aneurysm will also be found to have an abdominal aortic anuersym,3 this patient was at an elevated risk. Overlap in histochemical changes are observed in patients with AAA and TAA, and there may be a common cellular link that explains a similar pathogenesis.4 Formation of thrombus is the product of decreased laminar flow at the periphery of a dilated aorta, which causes blood stagnation.5
Ultrasound is a noninvasive method of testing for AAA that has little to no risk to the patient. An abbreviated examination of the aorta is easy to complete in less than one or two minutes and has a high sensitivity and specificity of 95% and 100%, respectively.4,6 In patients with known TAA, one should have a low threshold for screening for AAA in the ED, ideally with bedside ultrasound. Small aneurysms, between 3.0cm and 5.5cm in size, should be monitored annually for expansion in intervals specific to their size. In patients with AAA size above 5.5cm, surgical repair should be performed.7 Medical management can be used as an adjunct and consists of smoking cessation and high blood pressure control. The use of statins has also shown some benefit in reducing mortality.8
This patient was evaluated by vascular surgery in the ED and considered not an optimal surgical candidate. Because he was found to have concurrent renal impairment, any amount of intra-operative contrast dye would be detrimental and advised against. During his admission he was cautiously diuresed and ultimately discharged home with outpatient vascular surgical follow up for elective repair.
Topics:
Abdominal aortic aneurysm, aortic thrombus, aortic intramural hematoma, POCUS, ultrasound, CT.
References:
- Singh, K, Bonaa, KH, Jacobsen BK, Bjork L, Solberg S. Prevalence and risk factors for abdominal aortic aneurysms in a population-based study: the Tromsø Study. Am J Epidemiol. 2001; 154: 236–244.
- Johansen K, Koepsell T. Familial tendency for abdominal aortic aneurysms. JAMA. 1986; 256:1934–6.
- Black JH, Greene CL, Woo YJ. Epidemiology, risk factors, pathogenesis, and natural history of thoracic aortic aneurysm. In: Melin JA, ed. UpToDate. Waltham, MA: UpToDate Inc. https://www.uptodate.com/contents/epidemiology-risk-factors-pathogenesis-and-natural-history-of-thoracic-aortic-aneurysm. Accessed December 11, 2018.
- Chaer RA, Vasoncelos R, Marone LK, et al. Synchronous and metachronous thoracic aneurysms in patients with abdominal aortic aneurysms. J Vasc Surg. 2012;56(5):1261–1265. doi: 10.1016/j.jvs.2012.04.056.
- Reardon RF, Clinton ME, Madore F, Cook TP. Abdominal Aortic Aneurysm. In: Ma OJ, Mateer JR, Reardon RF, Joing SA, eds. Ma and Mateer’s Emergency Ultrasound. 3rd New York, NY: McGraw-Hill; 2014: 225-245.
- Fleming C, Whitlock EP, Beil TL, Lederle FA. Screening for abdominal aortic aneurysm: a best-evidence systematic review for the U.S. Preventive Services Task Force. Ann Intern Med. 2005; 142:203–11.
- Chaikof EL, Brewster DC, Dalman RL, et al. SVS practice guidelines for the care of patients with an abdominal aortic aneurysm: executive summary. J Vasc Surg. 2009; 50:880–96.
- Sukhija R, Aronow WS, Sandhu R, et al. Mortality and size of abdominal aortic aneurysm at long-term follow-up of patients not treated surgically and treated with and without statins. Am J Cardiol. 2006; 97:279-80.