Issue 4:4
A Low-Cost, Reusable Ultrasound Pericardiocentesis Simulation Model
DOI: https://doi.org/10.21980/J8TD1JThrough the use of this model and skill session, learners will be able to: 1) discuss the indications, contraindications, and complications associated with ultrasound guided pericardiocentesis; 2) demonstrate an ability to obtain subxiphoid and parasternal long views of the heart; 3) demonstrate an ability to identify pericardial fluid in these two views; and 4) demonstrate proper probe and needle placement to successfully perform an ultrasound guided pericardiocentesis in these two views.
ECG Stampede
DOI: https://doi.org/10.21980/J8PP93ECG Stampede is a unique educational program comprised of a comprehensive, video-based curriculum with accompanying student and instructor guides. ECG Stampede also features an engaging game accessible via modern browsers and dedicated mobile applications for iOS and Android devices. The gamified model presents learners with a batch of ECGs for which they must assign one of four triage acuities.
Status Asthmaticus
DOI: https://doi.org/10.21980/J8JW6SAt the end of this case, the learners should be able to diagnose an asthma exacerbation, provide the appropriate medications, determine when intubation is necessary, and describe the general principles of ventilator management in an asthmatic patient.
Emergency Medicine Curriculum Utilizing the Flipped Classroom Method: Pulmonary Emergencies
DOI: https://doi.org/10.21980/J8F646The educational strategies used in this curriculum include small group case-based modules authored by education faculty and content experts based on the core emergency medicine content outlined in the ABEM Model EM curriculum. The Socratic method, used during small group sessions, encourages active participation; small groups also focus on the synthesis and application of knowledge through the discussion of clinical experiences. The use of free open access medical education (FOAM) resources allows learners to work at their own pace and maximize autonomy. Learners are encouraged to use such resources for preparation prior to small group sessions, and also to review and help solidify important points after the conclusion of in-person discussions.
Novel Emergency Medicine Curriculum Utilizing Self-Directed Learning and the Flipped Classroom Method: Neurologic Emergencies Small Group Module
DOI: https://doi.org/10.21980/J89H0JWe aim to teach the presentation and management of cardiovascular emergencies through the creation of a flipped classroom design. This unique, innovative curriculum utilizes resources chosen by education faculty and resident learners, study questions, real-life experiences, and small group discussions in place of traditional lectures. In doing so, a goal of the curriculum is to encourage self-directed learning, improve understanding and knowledge retention, and improve the educational experience of our residents.
Resuscitation Rotation: A Novel Emergency Medicine Rotation to Augment Resuscitative Training
DOI: https://doi.org/10.21980/J85P9FOur goal is to augment resuscitative education in the ED in order to improve resident skill, confidence, and knowledge of resuscitative treatments.
A Simulation-Based Course for Prehospital Providers in a Developing Emergency Medical Response System
DOI: https://doi.org/10.21980/J82053This curriculum presents a refresher course in recognizing and stabilizing an acutely ill patient for prehospital providers practicing in a low/middle-income developing EMS system.
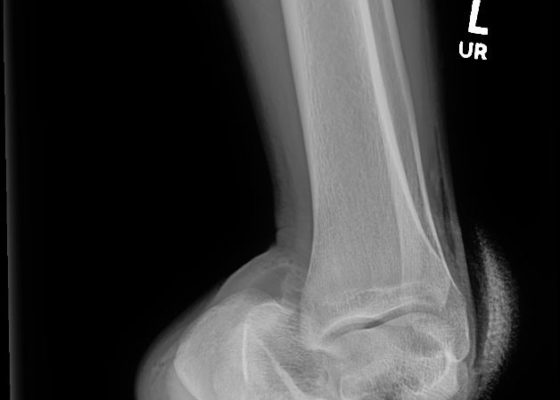
Open Subtalar Dislocation
DOI: https://doi.org/10.21980/J87P8PX-ray of the left ankle revealed a complete dislocation of the subtalar joint with medial dislocation of the calcaneus (outlined in orange) relative to the talus (outlined in red) with subcutaneous air noted in the lateral soft tissues (blue arrows in Figure 1). The talonavicular joint has also been disrupted (navicular outlined in blue). There was no evidence of fracture. Post-reduction computed tomography of the left lower extremity confirmed no evidence of associated fracture.