Ultrasound
A Woman’s Infertility Journey Complicated by Severe Ovarian Hyperstimulation Syndrome – A Case Report
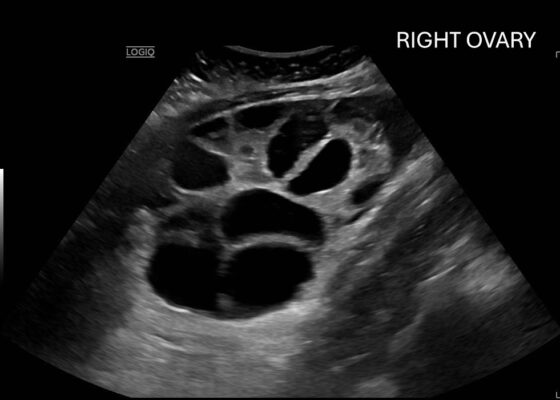
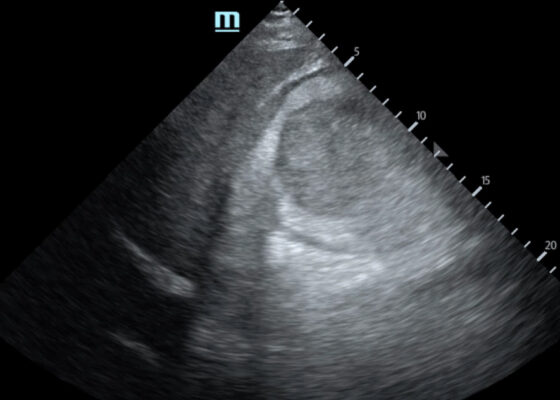
DOI: https://doi.org/10.5070/M5.52309Computed tomography (CT) of the abdomen and pelvis demonstrated pleural effusions in the lung bases (blue stars), ascites (blue stars), and enlarged ovaries with multiple cysts/follicles (white arrows). A formal pelvic US also demonstrated large volume ascites (white diamonds) and bilateral ovarian enlargement with numerous cysts. A CT angiogram (CTA) of the chest demonstrated small bilateral pleural effusions and no obvious pulmonary embolism.
A Case Report of Right Atrial Thrombosis Complicated by Multiple Pulmonary Emboli: POCUS For the Win!
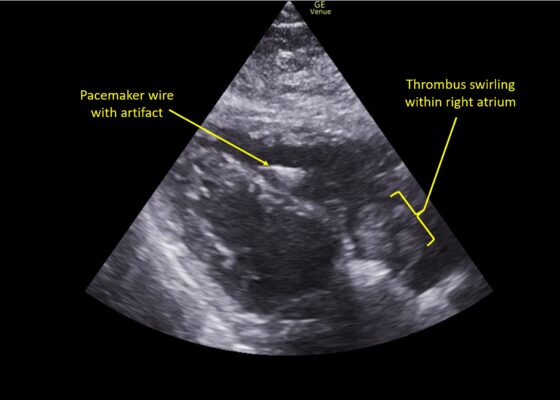
DOI: https://doi.org/10.21980/J8TM07Pulmonary POCUS was performed by the ED physician (GE Venue, C1-5-RS 5MHz curvilinear transducer), and lung examination was unremarkable with no pleural effusion, pneumothorax, or infiltrate. Subxiphoid views (GE Venue, 3Sc-RS 4MHz phased-array transducer) were obtained because this patient’s COPD with severe pulmonary hyperexpansion made parasternal and apical 4-chamber views suboptimal. A large thrombus can be seen within the right atrium (movie 1, images 1, 2). This has a serpiginous, rounded appearance and is mobile, appearing to swirl within the right atrium with intermittent extrusion through the tricuspid valve. A pacemaker wire is also visible within the right ventricle as a non-moving, hyperechoic, linear structure with posterior enhancement artifact. Pericardial effusion is not present.
Vaginal Bleeding Due to Iatrogenic Uterine Perforation – A Case Report
DOI: https://doi.org/10.21980/J83643The bedside transabdominal US of the pelvis showed a heterogeneous mixture of hypoechoic and hyperechoic endometrial thickening extending to the lower uterine segment (blue arrow), which was thought to represent active hemorrhage. Computed tomography of the abdomen and pelvis showed evidence of a large amount of endometrial hyperdensity (red arrow) suggestive of hemorrhagic contents within a grossly enlarged uterus. There was relative decreased enhancement of the uterine body and fundus, concerning for devascularization. There was also active extravasation along the left lateral uterus (yellow arrow).
Case Report of a Child with Colocolic Intussusception with a Primary Lead Point
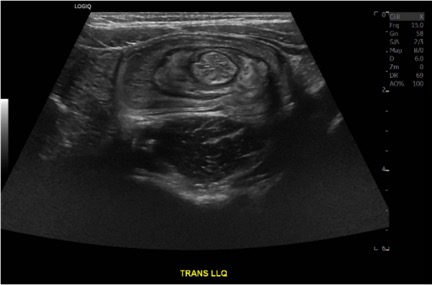
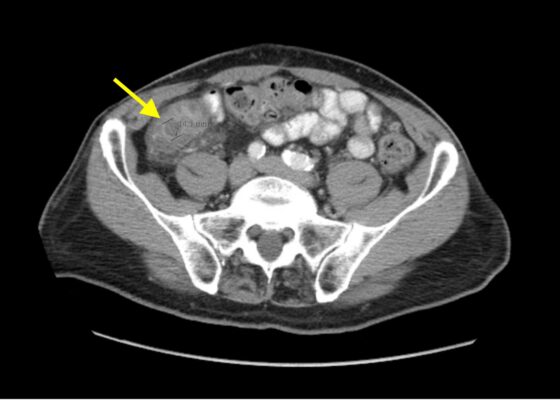
DOI: https://doi.org/10.21980/J8564QOn the initial ED visit, an abdominal ultrasound (US) was ordered which showed the classic intussusception finding of a target sign (yellow arrow), or concentric rings of telescoped bowel, on the transverse view of the left lower quadrant (LLQ).
Point-Of-Care Ultrasound Use for Detection of Multiple Metallic Foreign Body Ingestion in the Pediatric Emergency Department: A Case Report
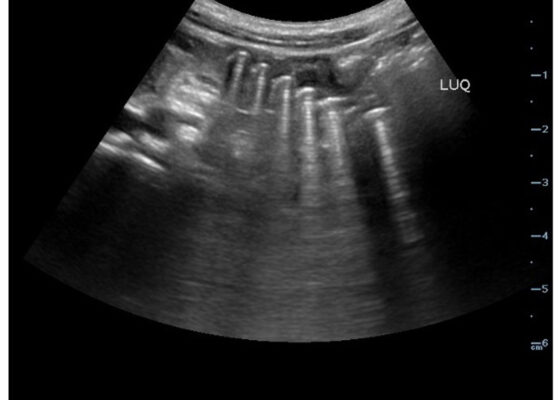
DOI: https://doi.org/10.21980/J83D2DBedside POCUS was performed on the patient’s abdomen using the curvilinear probe. The left upper quadrant POCUS image demonstrates multiple hyperechoic spherical objects with shadowing and reverberation artifacts concerning multiple foreign body ingestions. Though the patient and mother initially denied knowledge of foreign body ingestion, on repeated questioning after POCUS findings, the patient admitted to his mother that he ate the spherical magnets he received for his birthday about one week ago. The patient swallowed these over the course of two days. The presence of multiple radiopaque foreign bodies was confirmed with an abdominal X-ray.
Sonographic Retrobulbar Spot Sign in Diagnosis of Central Retinal Artery Occlusion: A Case Report
DOI: https://doi.org/10.21980/J8735PThe bedside ocular ultrasound (B-scan) was significant for small, hyperechoic signal (white arrow) in the distal aspect of the optic nerve, concerning for embolus in the central retinal artery. Subsequent direct fundoscopic exam was significant for a pale macula with cherry red spot (black arrow), consistent with central retinal artery occlusion (CRAO).
Trauma by Couch: A Case Report of a Massive Traumatic Retroperitoneal Hematoma
DOI: https://doi.org/10.21980/J84D2QUpon arrival at the trauma center, a FAST revealed a large, well-circumscribed abnormality (red outline) deep to the liver (blue outline and star) and gallbladder (green outline and star). The right kidney and hepatorenal space were not clearly visualized. The remainder of the FAST showed no free fluid in the splenorenal space, pelvis, and no pericardial effusion. He had lung sliding bilaterally.
Imaging Findings of Small Bowel – Diverticulitis: A Case Report
DOI: https://doi.org/10.21980/J8F078Bedside ultrasound was performed and showed thickened bowel wall (orange marker), fat enhancement (green marker), and phlegmonous structure with central echogenicity (yellow marker). Imaging of the abdomen and pelvis with CT showed marked wall thickening and inflammatory change involving a 7.0cm segment of the distal/terminal ileum suspicious for severe ileitis with phlegmon and microabscess on the coronal image (yellow arrow). Additonally, the transverse images show a small rim-enhancing focus within this region of inflammation measuring up to 1.4cm which could represent microabscess (yellow arrow). Diagnosis of diverticulitis by ultrasound is made by identifying the following findings: colon wall thicker than 5mm, fat enhancement, evidence of abscess, visualized diverticuli, air artifacts suggesting diverticuli, and tenderness with compression of the probe.6 Diagnosis of diverticulitis by CT is made by identifying the following findings: colonic wall thickening, pericolic fat stranding, abscess formation and enhancement of the colonic wall. Often, these signs are associated with an identifiable inflamed diverticulum.7