Search By Keyword
Found 645 Unique Results
Page 6 of 65
Page 6 of 65
Page 6 of 65
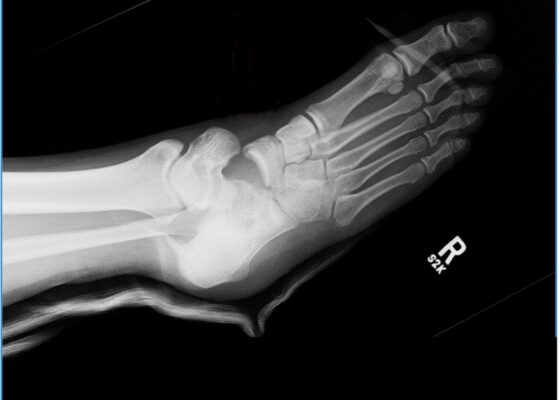
A Case Report of Lateral Subtalar Dislocation: Emergency Medicine Assessment, Management and Disposition
DOI: https://doi.org/10.21980/J8SS8PIn a lateral subtalar dislocation, the navicular bone (red bone in 3D anatomy image) and the calcaneus (yellow bone in 3D anatomy image) dislocate laterally in relation to the talus (lavender bone in 3D anatomy image). Plain film oblique and lateral X-rays demonstrate the initial dislocation (talus in red, navicular in blue). It is clear in the initial lateral view that there is loss of the talar/navicular articulation (noted by red arrow). The anterior-posterior x-ray is more challenging to discern the anatomy; however, the talus (red dot) is laterally displaced in comparison to the navicular (blue dot).
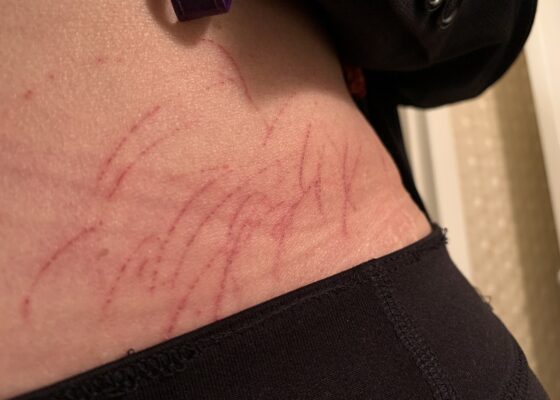
A Case Report of Dermatographia
DOI: https://doi.org/10.21980/J8P05PPhysical examination was unremarkable except for the urticaria on the right aside of her abdomen (white arrow) with overlying excoriations (stars). Of note, there were no burrows, papules or vesicles in the typical locations including the webs of the fingers, wrists, axillae, areolae, or genitalia. Examination of the linear dermatographia clearly revealed superficial wheals, versus underlying serpiginous lesions.
Modification of an Airway Training Mannequin to Teach Engagement of the Hyoepiglottic Ligament
DOI: https://doi.org/10.21980/J8R06PBy the end of this education session, participants should be able to: 1) identify relevant airway anatomy during intubation, including base of the tongue, epiglottis, midline vallecular fold, anterior arytenoids; 2) appreciate the value of a stepwise anatomically guided approach to intubation; 3) become familiar with the midline vallecular fold and underlying anatomy, including the hyoepiglottic ligament, and how proper placement of the laryngoscope can result in improved glottic visualization.
A Realistic, Low-Cost Simulated Automated Chest Compression Device
DOI: https://doi.org/10.21980/J8M63CBy the end of this educational session using a resuscitation trainer or high-fidelity manikin, learners should be able to: 1) recognize appropriate application of simulated ACCD to an ongoing resuscitation case; 2) demonstrate proper positioning of simulated ACCD in manikin model and 3) integrate simulated ACCD to provide compressions appropriately throughout cardiac arrest scenario.
Septic Abortion Complicated by Disseminated Intravascular Coagulation
DOI: https://doi.org/10.21980/J8GH1GAt the conclusion of the simulation session, learners will be able to: 1) Obtain a relevant focused history including pregnancy history, medication use, and past medical history. 2) Develop a differential for fever and vaginal bleeding in a pregnant patient. 3) Discuss management of septic abortion, including empiric broad-spectrum antibiotics and obstetric consultation for source control with dilation and curettage (D&C). 4) Discuss expected laboratory findings of disseminated intravascular coagulation (DIC). 5) Discuss management of DIC, including identification of underlying etiology and supportive resuscitation with blood products. 6) Review the components of blood products. 7) Identify appropriate disposition of the patient to the intensive care unit (ICU).
Electrical Storm/Refractory Ventricular Tachycardia
DOI: https://doi.org/10.21980/J8TS80By the end of this simulation, learners should be able to: 1) recognize unstable ventricular tachycardia and initiate ACLS protocol, 2) practice dynamic decision making by switching between various ACLS algorithms, 3) create a thoughtful approach for further management of refractory ventricular tachycardia, 4) interpret electrocardiogram (ECG) with ST-segment elevation (STE) and left bundle branch block (LBBB), 5) appropriately disposition the patient and provide care after return of spontaneous circulation (ROSC), 6) navigate a difficult conversation with the patient’s husband when she reveals that the patient’s wishes were to not be resuscitated.
Managing STEMIs without a Catheterization Lab: A Simulated Scenario to Improve Emergency Clinician Recognition and Execution of Thrombolysis in the Setting of Rural STEMI Management
DOI: https://doi.org/10.21980/J8K933By the end of this simulation, learners will be able to: 1) diagnose ST elevation myocardial infarction accurately and initiate thrombolysis in the rural setting without timely access to cardiac catheterization; 2) engage the simulated patient in a shared decision-making conversation, clearly outlying the benefits and risks of thrombolysis; 3) identify the indications and contraindications for thrombolysis in ST elevation myocardial infarction; 4) arrange for transfer to a tertiary care center following completion of thrombolysis.
Hypertensive Emergency Team-Based Learning
DOI: https://doi.org/10.21980/J8BP90By the end of this TBL session, learners should be able to: 1) define features of asymptomatic hypertension versus hypertensive emergency, 2) discuss which patients with elevated blood pressure may require further diagnostic workup and intervention, 3) identify a differential diagnosis for patients presenting with elevated blood pressures, 4) recognize the features of different types of end-organ damage, 5) review an algorithm for the pharmacologic management of hypertensive emergencies, 6) indicate dosing and routes of various anti-hypertensive medications, 7) choose the appropriate treatment for a patient who is hypertensive and presenting with flash pulmonary edema, 8) identify an aortic dissection on computed tomography (CT), 9) choose the appropriate treatment for a patient who is hypertensive and presenting with an aortic dissection, 10) identify intracranial hemorrhage on CT, 11) choose the appropriate treatment for a patient who is hypertensive and presenting with an intracranial hemorrhage, and 12) describe the intervention for warfarin reversal.
A Case Report of Acute Compartment Syndrome
DOI: https://doi.org/10.21980/J87061Inspection of the extremity revealed significant swelling with dark discoloration and multiple bullae (pre-operative photograph). Furthermore, notable swelling of the right foot was noted, which felt cold to palpation. Radiographs of pelvis, bilateral knees, tibia, fibula, and feet demonstrated no fractures or dislocations. The bilateral tibia and fibula X-ray revealed soft tissue swelling in the proximal legs, particularly evident in the right leg's AP view, which also showed numerous ovoid radiodensities in the anterior compartment, likely related to soft tissue injury. Post operative images are also provided demonstrating the patients’ four compartment fasciotomies which were loosely closed using staples.
Vaginal Bleeding Due to Iatrogenic Uterine Perforation – A Case Report
DOI: https://doi.org/10.21980/J83643The bedside transabdominal US of the pelvis showed a heterogeneous mixture of hypoechoic and hyperechoic endometrial thickening extending to the lower uterine segment (blue arrow), which was thought to represent active hemorrhage. Computed tomography of the abdomen and pelvis showed evidence of a large amount of endometrial hyperdensity (red arrow) suggestive of hemorrhagic contents within a grossly enlarged uterus. There was relative decreased enhancement of the uterine body and fundus, concerning for devascularization. There was also active extravasation along the left lateral uterus (yellow arrow).