Incarcerated Ventral Hernia of T-colon Resulting in Colon Perforation and Intraabdominal Abscess
History of present illness:
A 75-year-old female with a remote history of rectal cancer presented to the emergency department with acute right upper abdominal pain. The pain had begun suddenly after lunch. On review of systems, the patient had mild nausea. Initial vital signs were within normal limit. She denied fever, chills, or vomiting. The physical examination revealed a distended, tympanic abdomen with tenderness to palpation in the right upper quadrant. Laboratory examinations revealed a white-blood-cell count of 8.73 x 103 with 86% neutrophils. C-Reactive protein value was 1.17 mg/dL. She had a history of rectal cancer status post low anterior resection 14 years prior to this visit.
Significant findings:
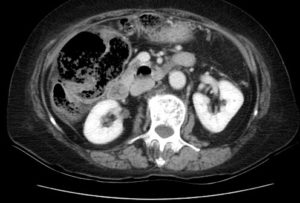
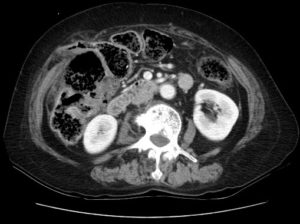
Computed tomography (CT) showed herniation of stool-filled, thin-walled colon through a narrow abdominal wall defect (green circle). Associated stranding of herniated fat is also seen (blue arrow). The narrow neck of the hernia sac and the fat stranding suggest incarceration. An abscess containing gas bubble secondary to perforation was observed in the vicinity of hepatic flexure (red circle).
Discussion:
Ventral hernias generally occur as a result of previous surgery or trauma. The incidence ranges from 2 % to 20%.1 Ventral hernias include all hernias of the anterior and the lateral abdominal wall.2,3 Midline hernias are more common. Paramedian or lateral defects are less common, but have a high prevalence of incarceration.1 The diagnosis of ventral hernias is still challenging without accepted diagnostic standards.4 Computed tomography scan is the recommended diagnostic tool if diagnosis cannot be made by physical examination. If the incarceration is not reduced, strangulation might occur and may lead to perforation.5,6 In patients with an acutely incarcerated or strangulated ventral hernia, emergent surgical consultation is warranted. An open rather than a laparoscopic approach is suggested.4 Intravenous broad-spectrum antibiotics should be started if obstruction is suspected or fever, leukocytosis is present. This case illustrates a ventral hernia of the colon resulting in acute colon obstruction, perforation of hepatic flexure, and intra-abdominal abscess. Emergency surgery is an essential part of treatment.
The patient in this case underwent laparotomy with right hemicolectomy and intra-abdominal abscess drainage. The patient subsequently received multiple operations because of anastomosis leakage and iatrogenic duodenal injury. The patient was discharged after 90 days of hospitalization.
Topics:
Ventral Hernia, incarceration, perforation.
References:
- Le Huu NR, Mege D, Ouaissi M, Sieleznezneff I, Sastre B. Incidence and prevention of ventral incisional hernia. J Visc Surg. 2012:149(5): e3-14.doi: 10.1016/j.jviscsurg.2012.05.004.
- Aguirre DA, Santosa AC, Casola G, Sirlin CB. Abdominal wall hernia: imaging features, complications, and diagnostic pitfalls at multi-detector row CT. 2005;25(6):1501-1520. doi: org/10.1148/rg.256055018.
- Lassandro F, Iasiello F, Pizza NL, et al. Abdominal hernias: radiological features. World J Gastrointest Endosc. 2011;3(6):110-117. doi: 4253/wjge.v3.i6.110.
- Birindelli A, Sartelli M, Saverio SD, et al. 2017 update of the WSES guideline for emergency repair of complicated abdominal wall hernias. World J Emerg Surg.2017; 12:37. doi: 1186/s13017-017-0149-y.
- Skelly BL, Neill Obstructed hepatic flexure contained in right-sided inguinoscrotal hernia resulting in a caecal perforation. Ann R Coll Surg Engl. 2013;95(6): e102-104. doi: 10.1308/003588413X13629960047551.
- Ota S, Noguchi T, Takao T, et al. An incarcerated colon inguinal hernia that perforated into the scrotum and exhibited an air-fluid level. Case Rep Med. 2015;1-3. doi: 1155/2015/105183.