Biceps Tendon Rupture
History of present illness:
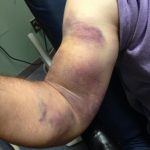
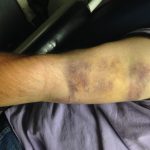
A 55-year-old male presented to the emergency department with a chief complaint of right arm pain. Five days prior to arrival, he attempted to lift himself up on his van and experienced what he described as a “rubber band snapping” in his right arm. He reported severe pain at the time that persisted but lessened in severity. Additionally, he reported increasing bruising over the proximal right arm. He had no history of prior right arm or shoulder injury.
Significant findings:
Physical exam was significant for ecchymosis and mild swelling of the right bicep. When the right arm was flexed at the elbow, a prominent mass was visible and palpable over the right bicep. Right upper extremity strength was 4/5 with flexion at the elbow.
Discussion:
The biceps brachii muscle is comprised of a long and short head, which share a common attachment at the bicipital tuberosity on the radius. The short head originates from the coracoid process of the scapula and the long head originates from the supraglenoid tubercle.1 Biceps tendon rupture has been found to occur at a rate of 0.53/100,000 over five years, and is three times more likely to occur in men than women.2 Risk factors for biceps tendon rupture include male sex, old age, increased body mass index, smoking, and pre-existing shoulder pathology.3,4 Diagnosis of biceps tendon rupture is typically a clinical diagnosis utilizing inspection and palpation as well as special testing such as the Speed’s and/or Yergason’s tests. Ultrasound may be used to aid in diagnosis; in full-thickness tears, ultrasound was found to have a sensitivity of 88% and a specificity of 98%. However, in partial thickness tears ultrasound has a sensitivity of 27% and a specificity of 100%.5 Often considered the gold standard in diagnosis, MRI has been found to have a sensitivity of only 67% and specificity of 98% in detecting complete tears6. Treatment initially consists of rest, ice, compression, and a short course of non-steroidal anti-inflammatory drugs. Follow up with an orthopedic surgeon is recommended in two to four weeks to determine operative versus non-operative management.7
Topics:
Biceps tendon, musculoskeletal injury, tendon rupture, orthopedics.
References:
- Netter F. Upper limb. In: Atlas of Human Anatomy. 6th Philadelphia, PA: Elsevier Saunders; 2014:431-506.
- Clayton RA, Court-Brown CM. The epidemiology of musculoskeletal tendinous and ligamentous injuries. 2008; 39(12):1338-1344. doi: 10.1016/j.injury.2008.06.021
- Kelly MP, Perkinson SG, Ablove RH, Tueting JL. Distal biceps tendon ruptures: an epidemiological analysis using a large population database.Am J Sports Med.2015;43(8):2012. doi: 10.1177/0363546515587738
- Patton WC, McCluskey GM 3rd. Biceps tendinitis and subluxation. Clin Sports Med. 2001;20(3):505. doi: 10.1016/S0278-5919(05)70266-0
- Da Gama Lobo L, Fessell DP, Miller BS, et al. The role of sonography in differentiating full versus partial distal biceps tendon tears: Correlation with surgical findings. AJR Am J Roentgenol.2013;200(1):158. doi: 10.2214/AJR.11.7302
- Malavolta EA, Assunção JH, Guglielmetti CL, de Souza FF, Gracitelli ME, Ferreira Neto AA. Accuracy of preoperative MRI in the diagnosis of disorders of the long head of the biceps tendon.Eur J Radiol. 2015; 84(11):2250. doi:1016/j.ejrad.2015.07.031
- Schickendantz M, King D. Nonoperative management (including ultrasound-guided injections) of proximal biceps disorders. Clin Sports Med. 2016;35(1):57. doi: 10.1016/j.csm.2015.08.006