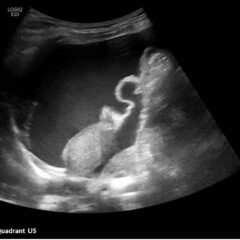
Syncope Due to a Ruptured Ectopic Pregnancy
ABSTRACT:
Audience:
This simulation is intended for all levels of emergency medicine residents.
Introduction:
Syncope and near-syncope are very common presenting complaints to the emergency department.1 There are several causes of syncope ranging from benign to life threatening. It is imperative that the emergency physician is able to evaluate and treat patients with undifferentiated syncope even with limited information. Approximately half of syncope cases can be differentiated by the presentation and clinical context.1 In addition to a thorough history, an electrocardiogram (ECG) should be obtained on all patients presenting with syncope or near-syncope since it is non-invasive and cost effective in assessing cardiac causes of syncope. In this particular simulation, the cause of syncope is due to a hemorrhagic shock from a ruptured ectopic pregnancy.
Educational Objectives:
At the conclusion of this simulation, the learner will be able to: 1) review the initial management of syncope; 2) utilize laboratory and imaging techniques to diagnose a ruptured ectopic pregnancy; and 3) demonstrate the ability to resuscitate and disposition an unstable ruptured ectopic pregnancy.
Educational Methods:
This simulation case was designed as a medium-to-high fidelity simulation scenario. It could also be altered and utilized as a practice oral board exam case.
Research Methods:
The quality of the simulation and educational content was evaluated by debriefing and verbal feedback that was obtained immediately after the case. Additionally, a survey was emailed to participants and observers of the case to provide qualitative feedback.
Results:
Post-simulation feedback from learners and observers was positive. Everyone present for the simulation felt that it was realistic and provided a unique opportunity to practice resuscitation skills.
Discussion:
Syncope and near-syncope are common presentations to the emergency department with multiple etiologies that range from cardiac, neurologic, neurocardiogenic, and orthostatic to unknown. It is crucial that we diagnose and treat life-threatening causes of syncope rapidly and with limited information. In this case, the cause of syncope due to a ruptured ectopic pregnancy should be rapidly diagnosed with a thorough history and exam, urine pregnancy test, and a bedside abdominal ultrasound. Once the urine pregnancy test was resulted, ectopic pregnancy was the top differential diagnosis for each learner that participated. Initially, most learners only performed a transabdominal pelvic ultrasound of the pelvis, which is normal in the case. One learner performed a rapid ultrasound for shock and hypotension (RUSH) exam and was able to find free fluid in the right upper quadrant. Overall, this case and the debriefing topics were effective for learners at all levels.
Topics:
Ectopic pregnancy, obstetrical emergencies, ultrasound, resuscitation.