Renal Infarction from Type B Aortic Dissection
History of present illness:
A 69-year-old-female with a medical history of hypertension presented to the emergency department (ED) complaining of sudden onset of lower back and abdominal pain. Eight hours prior to presentation she reported turning to grab something on another counter and felt a sudden onset sharp pain in her lower back. She began to notice ill-defined abdominal pain, although she denied any shortness of breath, chest pain, numbness, weakness, or urologic symptoms. Her vital signs on presentation to the ED were temperature 36.5˚C, blood pressure 143/88 mmHg, heart rate 84/minute, respiratory rate 14/minute, and oxygen saturation 93% on room air. On arrival, the patient was in significant discomfort and was rolling on the bed due to pain. Although she appeared to be in moderate distress she had minimal, if any, tenderness on abdominal exam, and only mild left lower back tenderness to palpation. This disconnect between the patient’s apparent discomfort and the lack of physical exam findings prompted the ordering of a computed tomography angiography (CTA) of the abdomen/pelvis with greatest suspicion for abdominal aortic aneurysm.
Significant findings:
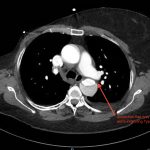
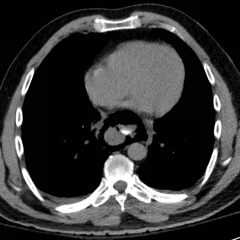
Initial abdominal images demonstrated a dissection flap; therefore, a CTA of the chest was also obtained. These images revealed a Stanford type B aortic dissection beginning just distal to the left subclavian artery and extending to the origin of the inferior mesenteric artery. The right renal artery arose from the true lumen of the dissection while the left renal artery arose from the false lumen. This case is interesting as imaging shows the lack of perfusion to the left kidney, residing in the retroperitoneum, which correlates with her non-descript abdominal and left flank pain.
Discussion:
Aortic dissection is defined as a tear within the wall of the aorta that allows blood to track between intima and media layers. A dissection is classified as Stanford Type A if it involves any portion of the ascending aorta and is usually managed surgically. A Stanford Type B dissection begins distal to the left subclavian artery and is often managed medically with specific focus on blood pressure reduction. Aortic dissection can involve various branching vessels which will affect both how the patient presents and the complexity of their medical course. Patients can present with limb ischemia, syncope, stroke, acute renal failure, mesenteric ischemia, myocardial infarction, or, such as the above patient, back and abdominal pain.1 While pain is often a presenting complaint, aortic dissections should be considered in the absence of pain.2 Painless limb paralysis can occur secondary to dissection involving vessels supplying the spinal cord.3 Diagnosis is typically made by CTA, which has a sensitivity of 98%-100%, although an initial chest x-ray can detect findings concerning for aortic dissection in 60%-90% of cases.4 Early and aggressive blood pressure control is essential to prevent worsening of the dissection by decreasing afterload and shearing forces. The preferred anti-hypertensive would be a titratable beta blocker such as esmolol or labetalol. Vascular surgery consultation can help determine the effects of branching vessel compromise or the treatment course for the patient.
For management of the above patient, vascular surgery was emergently consulted. Repeat vital signs included blood pressure 182/97 mmHg, heart rate 77/minute, respiratory rate 16/minute, and oxygen saturation 100% on 2L nasal cannula. Labetalol infusion was initiated to control her elevated blood pressure with a goal of less than 120/80 mmHg, intermittent fentanyl addressed pain and intravenous hydration was begun to protect her renal function. Additionally, she was started on a heparin drip to prevent thrombosis in the false lumen. This is not generally the standard of care for aortic dissections, but can be appropriate to avoid thrombosis-related complications in some patients.6
Topics:
Type B aortic dissection, back pain, cardiovascular, vascular, computed tomography, CT.
References:
- Grimm M, Schachner T. Complicated and uncomplicated acute type B aortic dissection: Definitions and approach in the light of IRAD and INSTEAD.In: Bonser RS, Pagano D, Haverich A, Mascaro J, eds. Controversies in Aortic Dissection and Aneurysmal Disease. London, UK: Springer; 2014:325-30.
- Alter SM, Eskin B, Allegra JR. Diagnosis of aortic dissection in the emergency department is rare. West J Emerg Med. 2015;16(5):629-631. doi: 10.5811/westjem.2015.6.25752
- Asouhidou I, Asteri T. Acute aortic dissection: be aware of misdiagnosis. BMC Research Notes.2009;2(2):1-6. doi: 10.1186/1756-0500-2-25.
- Tran TP, Khoynezhad A. Current management of type B aortic dissection. Vasc Health Risk Manag. 2009;5:53-63.
- Nickson, C. Acute aortic dissection. Life in the Fast Lane Medical Blog. https://lifeinthefastlane.com/ccc/acute-aortic-dissection/. Published December 31, 2015, Accessed February 25, 2017.
- Lachat M, Criado FJ, Veith FJ. The case for anticoagulation in patients with acute type B aortic dissection. J Endovasc Ther.2008;15(1):52-53. doi: 10.1583/07-2337.1