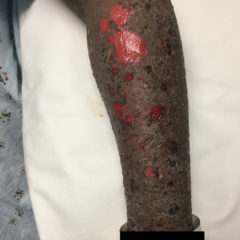
Various Degrees of Thermal Burns
History of present illness:
A 38-year-old male presented with significant thermal burns several hours after someone poured acetone on him and lit it on fire. He had burns to the face, neck, and mouth, without evidence of respiratory distress.
Significant findings:
On exam,there is a large swath of skin with evidence of thermal injury involving the neck, shoulder, chest, and face, including damage to the ear, external nostril, and lips. Burns exhibit varying degrees of severity and total approximately 4.5% of the body surface area. Several areas are charred and insensate to pinprick. The left earlobe is partially burned off. Patient’s airway is patent with no evidence of thermal injury or obstruction to the oropharynx or nasal vestibule.
Discussion:
Stratification of burn severity is categorized based on depth. First degree is superficial, very sensitive to pain, and exhibits blanching erythema. Second degree superficial partial thickness is sensitive to pain, but also exhibits blisters. Second degree deep partial thickness exhibits some sensitivity to pain and is erythematous or white. Third degree is full thickness, appears charred, and is completely insensate to pain.1 The most common mechanism for burns is contact with hot liquid, and the most common region affected is the upper extremities.2 Third degree burns account for only approximately 5% of all emergency department visits for thermal injuries.3 Clinical determination of depth according to color, blistering, and sensitivity to pinprick help determine whether a burn can heal within 21 days or if grafting will be necessary.4
The American Burn Association has criteria for transfer to a Burn Center based on total body surface area (TBSA): partial thickness > 20% TBSA, partial thickness >10% TBSA in children younger than 10 or adults older than 50, and full-thickness burns >5%.5,6 Other criteria include involvement of sensitive body parts, third degree burns, electric or chemical burns, inhalation injury, complications with preexisting conditions or rehabilitation, concomitant trauma, and burns in children.5,6 This patient met transfer criteria for third degree burns and facial involvement and was transferred for further management.
Topics:
Burn, thermal burn, trauma, dermatology.
References:
- Singer AJ, Lee CC. Thermal Burns. In: Walls RM, Hockberger RS, Gausche-Hill M, et al. eds. Rosen’s Emergency Medicine: Concepts and Clinical Practice. 9th ed. Philadelphia, PA: Elsevier; 2018:715-732.
- Taira BR, Singer AJ, Thode HC, Lee C. Burns in the emergency department: a national perspective. J Emerg Med. 2010;39(1):1-5. doi: 10.1016/j.jemermed.2008.01.009.
- Bessey PQ, Phillips BD, Lentz CW, et al. Synopsis of the 2013 annual report of the national burn repository. J Burn Care Res. 2014;35 Suppl 2: S218-34. doi: 10.1097/BCR.0000000000000080
- Jaskille AD, Shupp JW, Jordan MH, Jeng JC. Critical review of burn depth assessment techniques: Part I. Historical review. J Burn Care Res. 2009;30(6):937-47. doi: 10.1097/BCR.0b013e3181c07f21
- Reiband HK, Lundin K, Alsbjørn B, Sørensen AM, Rasmussen LS. Optimization of burn referrals. Burns. 2014;40(3):397-401.doi: 10.1016/j.burns.2013.08.001.
- Burn Center Referral Criteria. American Burn Association. Available at: http://ameriburn.org/wp-content/uploads/2017/05/burncenterreferralcriteria.pdf. Published May 2017. Accessed September 9, 2018.