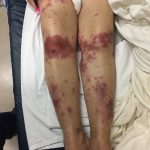
Steven-Johnson Syndrome
History of present illness:
72-year-old female with a history of hypertension and rheumatoid arthritis who presented to the emergency department (ED) with a chief complaint of rash for the past ten days. Her primary care provider prescribed azithromycin two weeks prior to her arrival in the ED for a sore throat. The rash started on her bilateral lower extremities and spread cephalad. She also noted a prodrome of subjective fevers and malaise.
Significant findings:
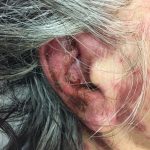
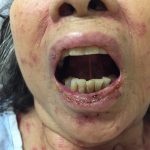
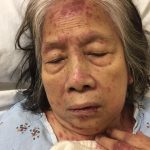
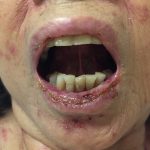
At presentation to the ED, a macular rash was notable on all four extremities, trunk and face, and involved mucous membranes of the oropharynx and vaginal introitus. The rash was painful, erythematous and purpuric with targetoid lesions. There were also multiple areas of sloughing and desquamation with a positive Nikolsky sign. Denudement totaled approximately 2% of total body surface area.
Discussion:
Stevens-Johnson syndrome (SJS) is a dermatolobullous disease on a spectrum of disease that includes toxic epidermal necrolysis (TEN). The distinguishing characteristic is percentage of body surface area (BSA) involvement, with SJS involving less than 10% of BSA while TEN involves greater than 30% of BSA.1
Medications are the most common cause of SJS with sulfonamides and penicillin being the most likely culprits (26%). Other medications include acetaminophen, carbamazepine, non-steroidal anti-inflammatory drugs (NSAIDs), phenytoin, and corticosteroids. Malignancy and immunosuppression are both risk factors for SJS.2
Onset of symptoms typically occurs four to twenty-eight days after starting a new medication, and typically presents with a prodrome that may include fever, upper respiratory infection symptoms, headache, and malaise.2 The rash is usually an atypical target lesion that first appears centrally.3 The rash may be painful and almost always has mucous membrane involvement. A positive Nikolsky sign is also seen, which is the sloughing off of epidermis when a shearing force is applied.1 It is important to note that SJS is a clinical diagnosis. Therefore, a relevant history including the use of drugs and previous infections are critical. Skin biopsies may be taken as well.2
Management includes identification and removal of the causal agent, and supportive treatment including hydration, electrolyte replacement, airway maintenance, prevention of secondary infection and pain control.2 The benefits of immune-targeted therapies are not well established, but there have been results showing a small reduction in mortality with the use of corticosteroids.1 The patient may need admission to a burn ICU.
The mortality rate for SJS is usually less than 5%, with sepsis being the main cause of death. Early clinical diagnosis is associated with improved mortality rates.4
Topics:
Stevens-Johnson syndrome, SJS, toxic epidermal necrolysis, TEN, maculopapular rash.
References:
- Marzano AV, Borghi A, Cugno M. Adverse drug reactions and organ damage: the skin. Eur J Intern Med. 2016;28:17-24. doi: 10.1016/j.ejim.2015.11.017
- Wong A, Malvestiti AA, Hafner MF. Stevens-Johnson syndrome and toxic epidermal necrolysis: a review. Rev Assoc Med Bras. 2016;62(5):468-473. doi:1590/1806-9282.62.05.468
- Kohanim S, Palioura S, Saeed HN, Akpek EK, Amescua G, Basu S, et al. Stevens-Johnson syndrome/toxic epidermal necrolysis–A comprehensive review and guide to therapy. I. Systemic Disease. Ocul Surf. 2016;14(1):2-19. doi: 1016/j.jtos.2015.10.002
- Miliszewski MA, Kirchhof MG, Sikora S, Papp A, Dutz JP. Stevens-Johnson syndrome and toxic epidermal necrolysis: an analysis of triggers and implications for improving prevention. Am J Med. 2016;129(11):1221-1225. doi: 10.1016/j.amjmed.2016.03.022