Erectile Dysfunction as a Presenting Symptom for Renal Cell Carcinoma
History of present illness:
A 54-year-old African American male presented to the emergency department (ED) with acute on chronic sharp pain radiating from the right groin to the medial aspect of the right thigh of two weeks duration. In association with the pain, he described intermittent numbness from the medial thigh to the anterior knee. Upon direct questioning he acknowledged new onset erectile dysfunction, difficulties with urination, and unintended weight loss of ten pounds over the last two months. He denied fevers, blood thinners, intravenous drug use or recent trauma but had chronic back pain resulting from a motor vehicle collision ten years prior. His only other medical history was hypertension and cigarette smoking.
Patient had normal vital signs and appeared older than stated age. In the right leg, he had 4/5 strength with hip flexion and difficulty maintaining a right leg raise for greater than two seconds. Motor strength was normal in the left leg and bilateral upper extremities. Sensation to pinprick and light touch was diminished on the right medial thigh extending to the right anterior knee. Proprioception was intact in all extremities. Patellar and Achilles reflexes were 2+ bilaterally and Babinski’s sign was not present bilaterally. Based on examination findings and a history concerning for spinal cord compression, a magnetic resonance imaging (MRI) of the thoracic and lumbar spine was performed. Laboratory studies were remarkable for a mildly elevated creatinine of 1.7 mg/dL, a hemoglobin of 9.6, and trace hematuria on urinalysis.
Significant findings:
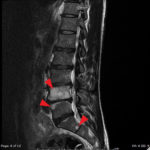
The MRI showed extensive spondylotic changes suggestive of malignancy (red arrows) with severe spinal canal stenosis at the lumbar spine L3-L4 (purple arrows) level contributing to clumping of cauda equina nerve roots and severe bilateral neuroforaminal narrowing with diffuse disc bulges abutting the exiting nerve roots at multiple levels. Findings also showed a hypo-attenuated tumor (blue arrow) and hyper-attenuated loculated tumor (green arrow) consistent with renal cell carcinoma (RCC).
Discussion:
While the ultimate diagnosis in this case ended up being renal cell carcinoma, we hope that this highlights the importance of a thorough history and physical examination in those patients presenting with acute on chronic issues. The initial physical exam and history caused concern for acute cord compression prompting the decision for advanced imaging. Physicians should consider many etiologies for cord compression and ask questions to risk stratify for infection (spinal epidural abscess, diskitis, and myelitis), trauma (fractures, spinal cord injuries), disk herniation, metastatic disease, and vascular causes (abdominal aortic aneurysm, retroperitoneal bleeding and spinal epidural hematoma). This can be done by eliciting red flags including extremes of age, history of cancer, immunodeficiency, history of trauma or coagulopathy, and specific cord compression symptoms (bowel or bladder incontinence, saddle anesthesia and progressive lower extremity weakness.)
While we were able to rapidly obtain MRI imaging, other imaging modalities may be more readily accessible. If a boney cause is suspected, plain radiographs can be obtained to help assess for compression fractures, lytic lesions, or erosion of bones that could be traumatic or due to metastatic disease. However, radiographs cannot rule out infection, vascular causes, or cord compression. Computed tomography can be helpful to assess boney pathology, but a typical CT does not show epidural space, the spinal cord, or the nerves. Magnetic resonance imaging is preferable for soft tissue imaging and is the most sensitive test for spinal cord pathology.1,2 If there are contraindications to performing an MRI, a CT myelogram can be performed to provide information about spinal cord abnormalities, but this should be done in consultation with both a spine specialist and radiologist.
Renal cell carcinomais the most common primary renal neoplasm and is highly aggressive, accounting for almost 14,000 deaths/year in the United States.3 The “classic triad” of flank pain, hematuria and a palpable abdominal mass is rarely observed and when present indicates a large tumor burden.4 Over the past 50 years the 5-year survival rate has nearly doubled mediated by earlier detection and improved surgical techniques. Patients presenting with RCC are usually older men with risk factors including smoking, hypertension, and obesity.5-7 Renal cell carcinoma in itself can be a diagnostic dilemma because it may present commonly as the source of a paraneoplastic syndrome. Patients can present with neuromyopathy, hypertension, anemia, fever, weight loss, and hypercalcemia. It is unclear whether all locally confined RCC found on imaging results is clinically significant.8 However, in this case the MRI in the ED allowed for expedited diagnosis, evaluation, and treatment of this highly aggressive malignancy which otherwise may have been missed. Spinal metastasis with cord compression is an oncologic emergency. This case demonstrates the diagnostic difficulty of RCC as well as the importance of thorough history and neurological examination in the common complaint of back pain.
Topics:
Magnetic resonance imaging,MRI, advanced imaging, spinal cord compression, cauda equina, erectile dysfunction, renal cell carcinoma.
References:
- Ahmad Z, Mobasheri R, et al. How to interpret computed tomography of the lumbar spine. Ann R Coll Surg Engl. 2014 Oct; 96(7): 502-507.
- Distefano D, Cianfoni A. Imaging of spinal cord compression. Imaging Med. 2014;6(1): 86-116.
- Bukowski RM, Novick A. Clinical Management of Renal Tumors. Totowa, NJ: Humana Press; 2008.
- Cohen HT, McGovern FJ. Renal-cell carcinoma. N Engl J Med. 2005;353(23):2477-2490. doi: 10.1056/NEJMra043172
- Pantuck AJ, Zisman A, Belldegrun AS. The changing natural history of renal cell carcinoma. J Urol. 2001;166(5):1611-1623. doi: 10.1016/S0022-5347(05)65640-6
- Noone AM, Howlader N, Krapcho M, et al (eds). SEER Cancer Statistics Review, 1975-2015, National Cancer Institute. Bethesda, MD, https://seer.cancer.gov/csr/1975_2015/, based on November 2017 SEER data submission, posted to the SEER web site, April 2018. http://seer.cancer.gov/statfacts/html/kidrp.html.Accessed on June 4, 2018.
- Adams KF, Leitzmann MF, Albanes D, et al. Body size and renal cell cancer incidence in a large US cohort study. Am J Epidemiol. 2008;168(3):268-277. doi: 10.1093/aje/kwn122
- Hollingsworth JM, Miller DC, Daignault S, Hollenbeck BK. Rising incidence of small renal masses: a need to reassess treatment effect. J Natl Cancer Inst. 2006;98(18):1331-1334. doi: 10.1093/jnci/djj362