Visual EM
Trapped In Transit – A Case Report of a Pediatric Gastric Bezoar Causing Intermittent Small Bowel Obstruction
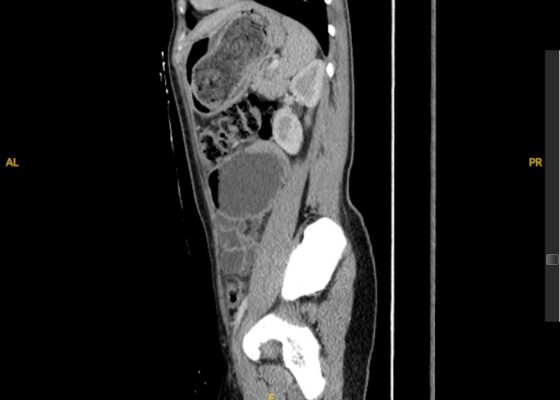
DOI: https://doi.org/10.5070/M5.52259The CT scan identified a heterogenous, mass-like lesion extending from the gastric fundus to the antrum, along with a small bowel obstruction (SBO) and significant small bowel dilation. An additional smaller heterogenous mass-like lesion was seen in the small bowel, causing the SBO. Given the mass-like lesion’s mixed attenuation and presence of internal air, a gastric bezoar was strongly suspected.
Overlooked and Undernourished: A Case Report of Scurvy Linked to Food Insecurity
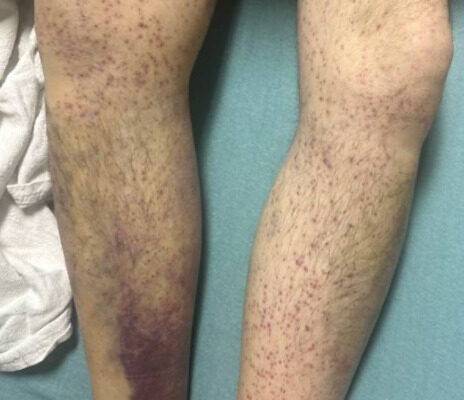
DOI: https://doi.org/10.5070/M5.52313Images A and B of the lower extremities show what initially appeared to be a petechial rash with scattered ecchymoses bilaterally, primarily on the right lower leg. On closer examination, images C and D more clearly show these spots to be flat and non-blanching, indicative of follicular hyperkeratosis with perifollicular hemorrhages. The classic coiled or corkscrew hair findings are not seen in these images. Image E shows evidence of palatal ecchymosis, without evidence of gingival bleeding, likely due to loss of dentition. This constellation of exam findings reflects the production of weakened or dysfunctional collagen in connective tissue and vascular structures and is strongly suggestive of the clinical diagnosis of scurvy. Image F shows resolution of the patient’s dermatologic findings after three weeks of treatment.
A Case Report of a 36-year-old Male Diagnosed with a Spontaneous Coronary Artery Dissection
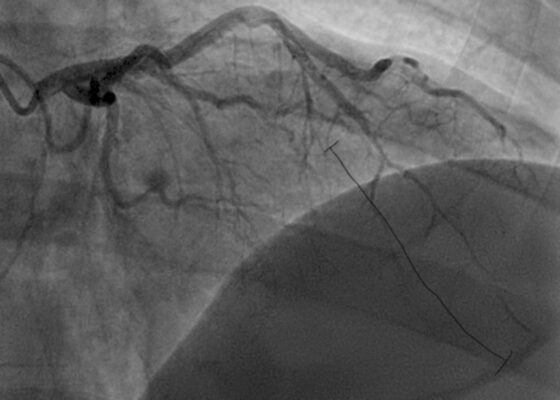
DOI: https://doi.org/10.5070/M5.52022The initial ECG obtained from the patient shows subtle ST-segment elevation noted in leads I, aVL, and V2-V5, suggestive of pathology of the left anterior descending artery. The results of the catheterization revealed a spontaneous coronary artery dissection of the distal portion of the left anterior descending coronary artery, which can be seen in the image of the angiogram, with the diseased portion notated between the brackets.
A Case Report of an Atypical Presentation of Fournier’s Gangrene
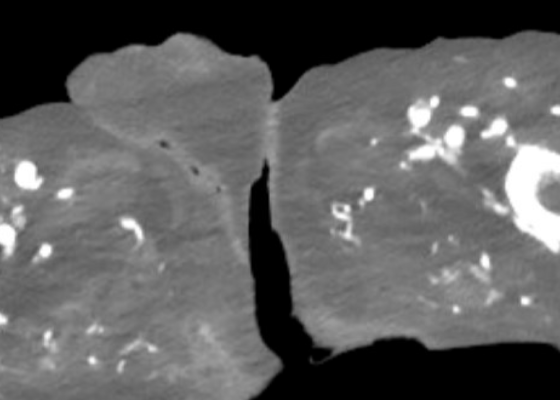
DOI: https://doi.org/10.5070/M5.52203A computed tomography (CT) scan of the abdomen and pelvis was significant for scrotal fluid and punctate gas locules (red arrow) without discrete evidence of invasion into the adjacent soft tissues, suspicious for Fournier’s gangrene. There was also fluid collection centered around the seminal vesicles suggestive of an abscess.
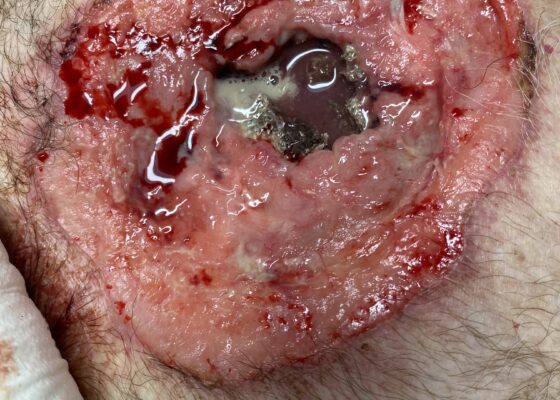
Open Chest Wound with Sternal Fracture in the Emergency Department, a Case Report
DOI: https://doi.org/10.5070/M5.52202The image demonstrates the large chronic-appearing wound of the patient’s anterior chest as well as the visible fractured segments of the patient’s exposed sternum. The sternum is necrotic appearing concerning for a chronic process including osteomyelitis and malignancy. Purulent drainage is visible on the wound consistent with an infectious process.
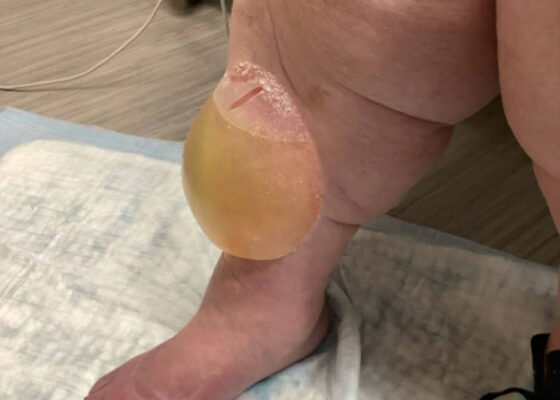
Effects of Volume Overload: A Case Report of an Edema Bulla
DOI: https://doi.org/10.5070/M5.52206This image shows a large edema bulla on the patient's right shin. The bulla is 10 x 10 cm, filled with serous fluid, has a spontaneously occurring defect in the skin of the superior portion of the bulla, and is non-erythematous. The bulla is much larger than the 1-5 cm edema bullae described in the literature. As edema bulla is primarily a clinical diagnosis, taking the full history and physical exam into account is essential to recognize these bullae.
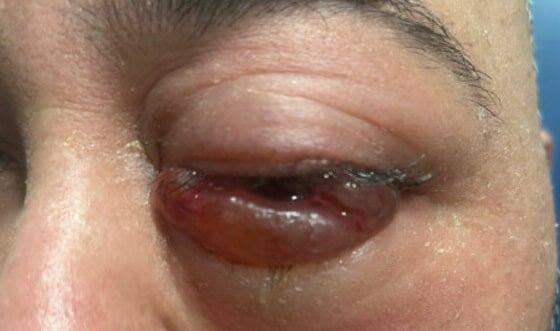
A Case Report of Carotid Cavernous Fistula: A Commonly Missed Diagnosis
DOI: https://doi.org/10.5070/M5.52242The initial physical exam performed by the ED provider revealed severe left eye chemosis, clear drainage, visual acuity of right eye 20/100 and left eye 20/400, and a left eye IOP of 52. There was a deficit of extraocular movement in all directions of gaze and limitation in all visual fields in the left eye. The MRI showed that at the level of the eye, the left cavernous sinus is asymmetrically enlarged compared to the right (red arrow) with an enlarged left inferior petrosal sinus with internal flow void on the pre-contrast MRI images (blue arrow). The orange arrow notes a central filling defect of the left superior ophthalmic vein on the MRA.
Case Report of a Patient Presenting with Nonketotic Hyperglycemia Hemichorea
DOI: https://doi.org/10.21980/J8.52115Laboratory tests indicated elevated blood glucose levels (198 mg/dL) with no urinary ketones, anion gap of 12, thyroid stimulating hormone (TSH) of 12 UIU/ml, and an increased glycated hemoglobin (HbA1c) of 14.9%. After initial stroke evaluation with neurology, imaging studies, including computed tomography (CT)/CT angiography (CTA) of the brain and neck, were unremarkable, ruling out structural lesions or acute stroke. Neurology recommended an MRI which showed T1 shortening within the left basal ganglia involving both the caudate nucleus and the lentiform nucleus. T1 shortening indicates changes in the tissue composition or structure that alters how the tissue responds to the MRI pulse, giving the tissue a brighter appearance on MRI (see white arrow).