Ophthalmology
Traumatic Hyphema
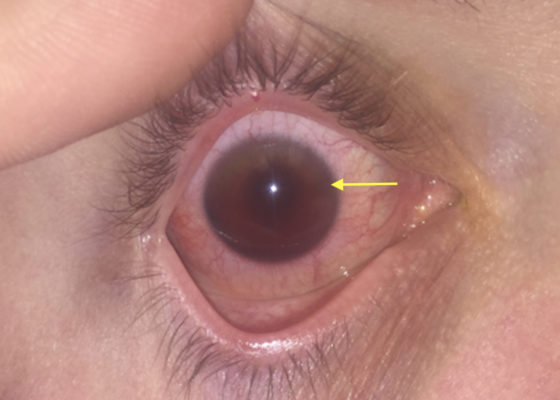
DOI: https://doi.org/10.21980/J8Z04SUpon initial evaluation, the patient had an obvious hyphema in the right eye with associated conjunctival injection. Initially, the bleeding in the anterior chamber was cloudy just above the level of the pupil (yellow arrow), appearing to possibly be a grade II hyphema. There were no other signs of trauma to the eye under Wood’s lamp examination with fluorescein staining. The globe was intact. Intraocular pressure in the affected eye was 19 mmHg and 15 mmHg in the unaffected eye. Extraocular movements were full and intact. The pupil was 4 mm round and reactive to direct and consensual light. Visual acuity was greater than 20/200 in the affected eye compared to 20/25 in the unaffected eye. After an observation period of two hours, with the patient remaining upright, the hyphema had settled down to a rim in the lower anterior chamber (green arrow), a grade I hyphema.
Retinal Detachment
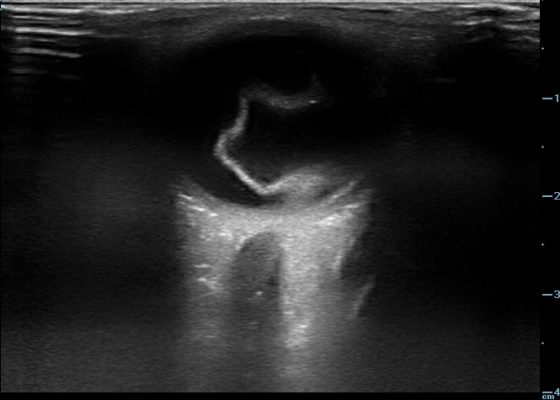
DOI: https://doi.org/10.21980/J8204QBedside ocular ultrasound revealed a serpentine, hyperechoic membrane that appeared tethered to the optic disc posteriorly with hyperechoic material underneath. These findings are consistent with retinal detachment (RD) and associated retinal hemorrhage.
Herpes Zoster Ophthalmicus
DOI: https://doi.org/10.21980/J88H07Physical exam was significant for an erythematous maculopapular rash in the right ophthalmic nerve (V1) region, a crusted vesicle at the right upper eyelid, and surrounding eyelid edema. Visual acuity remained at baseline and intraocular pressure was within normal limits. External slit lamp exam with fluorescein staining was remarkable for pseudodendrites in the inferior-temporal cornea approximately 1.5 mm from the limbus. Ophthalmology was consulted and completed an in-depth evaluation of the corneal lesions. They found no evidence of anterior chamber reaction and performed a complete dilated fundus examination which demonstrated no retinal involvement. The patient was then discharged on acyclovir and erythromycin ointment with close follow-up.
Point-of-care Ultrasound Detection of Endophthalmitis
DOI: https://doi.org/10.21980/J8G634The patient’s ultrasound revealed an attached retina and a complex network of hyperechoic, mobile, membranous material in the posterior segment.
Corneal Sparing Conjunctival Abrasion
DOI: https://doi.org/10.21980/J8KG93Physical exam was significant for multiple broken teeth, multiple minor abrasions on the face, and fine shards of shattered glass on his face and hair. His right eye had conjunctival injection, with no signs of subconjunctival hemorrhage or ocular penetration. Vision, extraocular movement, and pupillary exam were grossly intact. Fluorescein staining with slit lamp exam with cobalt blue filter examination of the right eye revealed superficial bulbar conjunctival uptake of fluorescein dye staining an area of the conjunctiva inferior to the limbus 5 mm vertical by 2 mm horizontal (estimation by photo provided). No foreign bodies were visualized in the inferior fornix. These findings were consistent with superficial conjunctival abrasion. The exam noted sparing of the corneal epithelium.
Globe Rupture
DOI: https://doi.org/10.21980/J8N91ZThe patient’s computed tomography (CT) head demonstrated a deformed left globe, concerning for ruptured globe. The patient had hyperdense material in the posterior segment (see green arrow), consistent with vitreous hemorrhage. CT findings that are consistent with globe rupture may include a collapsed globe, intraocular air, or foreign bodies.
The Halloween Lateral Canthotomy Model
DOI: https://doi.org/10.21980/J8GW2NThe purpose of the model is to teach residents and students how to perform lateral canthotomy and to achieve competency in their skills.
Intraocular Foreign Body: Ultrasound and CT Findings
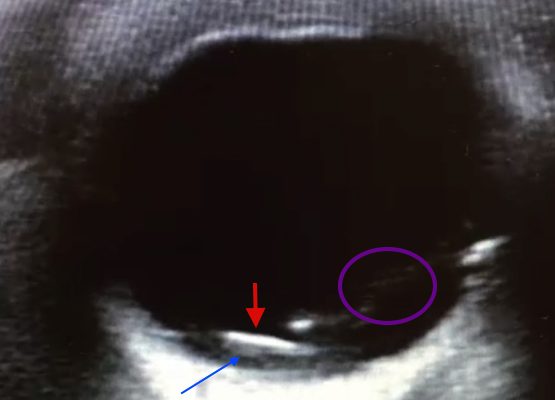
DOI: https://doi.org/10.21980/J8JS3MPoint of care ultrasound revealed a mobile, radiolucent hyperechoic structure (see red arrow) with reverberation within the posterior chamber (see blue arrow), likely a metallic foreign body. Linear areas of mobile hyperechoic material revealed possible vitreous hemorrhage (see purple circular area). Orbital non-contrast CT confirmed a 3 mm metallic focus within the dependent portion of the left globe, lodged in the posterior sclera, with some vitreous hemorrhage but no evidence of globe rupture. Ophthalmology was consulted and the patient was taken to surgery later that night.