Posts by JETem
Right Ventricular Dilation in Patient With Submassive Pulmonary Embolism
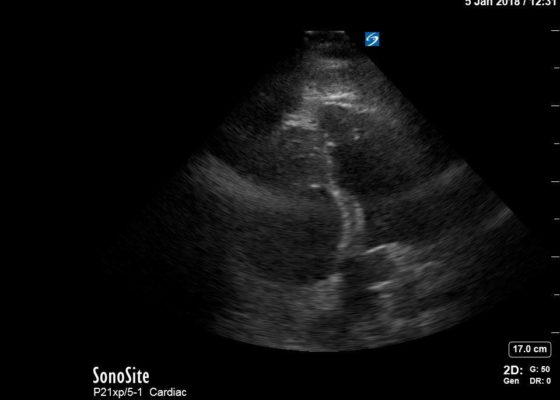
DOI: https://doi.org/10.21980/J82P84Bedside echocardiography four chamber view revealed enlarged right ventricular (RV) to left ventricular (LV) ratio (greater than 1) on apical four-chamber view (see red and blue outlines respectively). The right atrium is not clearly delineated in this image and therefore is not outlined. One can also rule out a large pericardial effusion as the cause of her dyspnea, since there is no large hypoechoic collection surrounding the heart on either four- chamber view or parasternal long view.
Traumatic Hyphema
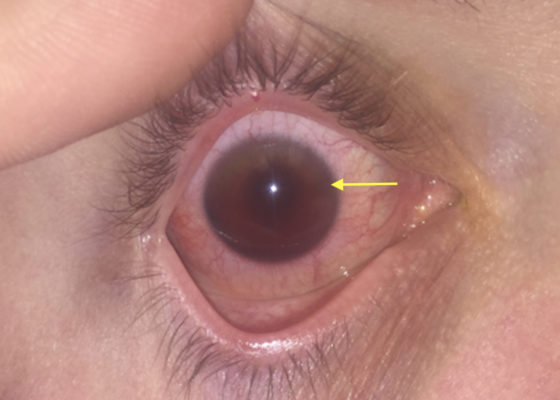
DOI: https://doi.org/10.21980/J8Z04SUpon initial evaluation, the patient had an obvious hyphema in the right eye with associated conjunctival injection. Initially, the bleeding in the anterior chamber was cloudy just above the level of the pupil (yellow arrow), appearing to possibly be a grade II hyphema. There were no other signs of trauma to the eye under Wood’s lamp examination with fluorescein staining. The globe was intact. Intraocular pressure in the affected eye was 19 mmHg and 15 mmHg in the unaffected eye. Extraocular movements were full and intact. The pupil was 4 mm round and reactive to direct and consensual light. Visual acuity was greater than 20/200 in the affected eye compared to 20/25 in the unaffected eye. After an observation period of two hours, with the patient remaining upright, the hyphema had settled down to a rim in the lower anterior chamber (green arrow), a grade I hyphema.
Point of Care Ultrasound Illustrating Small Bowel Obstruction
DOI: https://doi.org/10.21980/J8T637POCUS of the small bowel illustrated significantly dilated loops of bowel (white line), thickened bowel wall (white arrow) and to-and-fro peristalsis, consistent with small bowel obstruction.
The Use of a Social Media Based Curriculum for Newly Matched Interns Transitioning into Emergency Medicine Residency
DOI: https://doi.org/10.21980/J8F92GThis curriculum is designed to bridge this gap by fostering an environment in which incoming interns can communicate, collaborate, and practice clinical reasoning with each other and faculty prior to their arrival in residency. The goals and objectives were tailored to the Accreditation Council for Graduate Medical Education (ACGME) level 1 milestones in patient care. 1) Interpret basic ECGs; 2) Demonstrate ability to interpret basic radiographs; 3) Identify common visual diagnoses; 4) Identify common neurological emergencies on head imaging; 5) Recognize basic airway anatomy; 6) Demonstrate successful application of FOAMed resources to clinical cases; 7) Interpret common ultrasound images; 8) Describe common ED procedures; 9) Demonstrate fundamental knowledge of evidence-based medicine and biostatistics
High Fidelity In Situ Shoulder Dystocia Simulation
DOI: https://doi.org/10.21980/J88305DAt the end of this simulation, learners will: 1) Recognize impending delivery and mobilize appropriate resources (ie, both obstetrics [OB] and NICU/pediatrics); 2) Identify risk factors for shoulder dystocia based on history and physical; 3) Recognize shoulder dystocia during delivery; 4) Demonstrate maneuvers to relieve shoulder dystocia; 5) Communicate with team members and nursing staff during resuscitation of a critically ill patient.
Fainting Spells
DOI: https://doi.org/10.21980/J8Z91RABSTRACT: Audience: The target audience for this simulation is 4th year medical students, emergency medicine residents, pediatric residents, and family medicine residents. Introduction: Brugada syndrome is defined as the combination of specific electrocardiogram (ECG) changes and clinical manifestations of a ventricular arrhythmia, including syncope and sudden cardiac arrest.1 Brugada syndrome is caused by a mutation in the phase-0 cardiac sodium channel. This
Guillain-Barrè
DOI: https://doi.org/10.21980/J8TH06At the conclusion of the simulation session, learners will be able to: 1) Recognize the clinical signs and symptoms associated with Guillain-Barré syndrome, including muscle weakness and hyporeflexia. 2) Identify abnormal vital signs secondary to dysautonomia. 3) Discuss evaluation for impending respiratory failure, including bedside pulmonary function testing. 4) Discuss the management of Guillain-Barré, including management of dysautonomia and respiratory failure, as well as definitive management with plasmapheresis versus intravenous immunoglobulin. 5) Appropriately disposition the patient to the intensive care unit. 6) Effectively communicate with team members and nursing staff during resuscitation of a critically ill patient