Talonavicular Dislocation
History of present illness:
A 28-year-old female presented with left ankle pain after a fall down a flight of stairs. She had normal vital signs. Though her left ankle had an obvious deformity on exam, she was able to move her toes with mild limitation secondary to pain without sensory deficits. She had 2+ dorsalis pedis and posterior tibial pulses. Her lower extremity compartments were soft to palpation.
Significant findings:
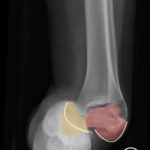
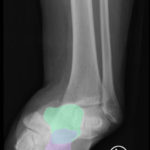
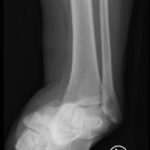
The X-rays were significant for a subtalar dislocation. The calcaneus (red) is laterally displaced with respect to the talar head (orange), and the white lines indicate the normal articular surface. Additionally, there was a talonavicular dislocation, as seen in the fourth image: the talus (green) and navicular bone (purple) overlapping suggests a dislocation. In a normally aligned foot, the boundaries of the two bones create a point of articulation.
Discussion:
Subtalar dislocations arise from both the talonavicular and talocalcaneal joints.1 Talonavicular dislocations are uncommon and occur due to severe inversion or eversion of the foot that disrupts the ligamentous structures supporting the joint.2 A thorough physical exam should be performed to assess the extent of injury. One must also be mindful of concomitant injuries, such as more proximal fractures/dislocations and compartment syndrome. The majority of the blood supply to the talus arises from the dorsalis pedis artery, and therefore, talonavicular dislocations with subtalar dislocations lead to avascular necrosis in 40% of cases.2
Proper diagnosis of talonavicular dislocations require obtaining anteroposterior (AP), lateral, and mortise views of the ankle and foot.3 The utility of computed tomography (CT) in diagnosis has also been discussed. One study reported that 44% of patients who received CT for subtalar dislocation had a treatment plan differing from that based on plain film findings.4 Specifically, CT identified fractures that were not visible on plain films as well as intraarticular debris requiring evacuation in an effort to promote proper healing and function.
Most dislocations are amenable to closed reduction as first-line treatment.1 Early reduction is crucial as it decreases the chance of vascular compromise. Closed reduction is performed by applying traction at the heel with counter-traction at the thigh while the knee is flexed to 90 degrees to relax the gastrocnemius muscle.5 In the case of a lateral dislocation, a firm eversion of the foot is performed while direct pressure at the talar head is applied.5 Post-reduction imaging should be obtained for confirmation. Open reduction and internal fixation (ORIF) is utilized in up to 32% of cases when closed reduction fails.1
Topics:
Talonavicular dislocation, orthopedics, ortho, foot.
References:
- Baba MA, Halwai MA, Mir BA, Bashir A, Wani M. Medial subtalar dislocation of the foot associated with an acute compartment syndrome: a case report. The Foot and Ankle Online Journal, 2013;6(6):1941-6806. doi: 10.3827/faoj.2013.0606.001.
- Wheeless CR. Avascular necrosis and salvage of talus fractures. In Wheeless’ Textbook of Orthopaedics. Towson, MD: Data Trace Internet Publishing; 2016.http://www.wheelessonline.com/ortho/anv_and_salvage_of_talus_fractures. Accessed September 19, 2018.
- Koulouris G, Morrison WB. Foot and ankle disorders: radiographic signs. Semin Roentgenol. 2005;40(4):358-379. doi: 10.1053/j.ro.2005.01.018.
- Bibbo C, Lin SS, Abidi N. Missed and associated injuries after subtalar dislocation: the role of CT. Foot Ankle Int. 2001;22(4):324–328. doi: 10.1177/107110070102200409.
- William Y, Patrick N, Michael B, Stephen F. Talocalcaneal navicular dislocation: a review. In: The Podiatry Institute Update 2011. 2011:49-55.