Issue 1:2
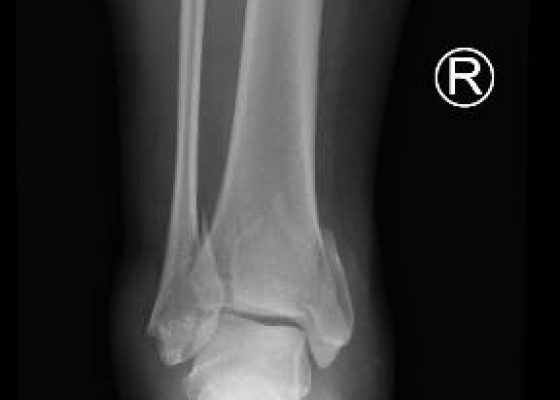
Trimalleolar Fracture
DOI: https://doi.org/10.21980/J8PP46Anteroposterior (AP), lateral, and oblique x-ray views were obtained. The AP view revealed a displaced spiral fracture of the lateral malleolus (red) and a vertical fracture of the medial malleolus (blue). The lateral view revealed a displaced fracture of the posterior malleolus, tibial plafond (yellow), and the oblique view showed widening of the distal tibiofibular syndesmosis (green). CT scans confirmed trimalleolar fracture, annotated with the same colored lines (red, lateral malleolus; blue, medial malleolus; yellow, posterior malleolus).
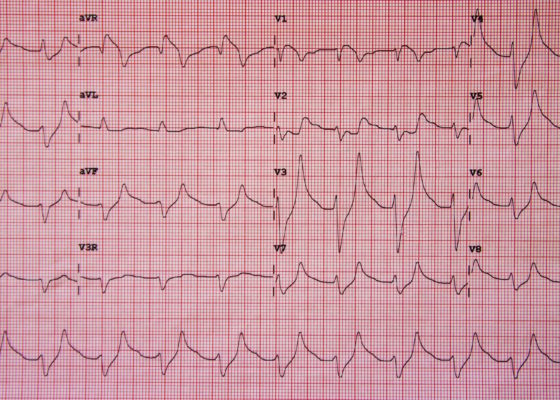
Hyperkalemia on ECG
DOI: https://doi.org/10.21980/J8K017Initial ECG shows tall, peaked T waves, most prominently in V3 and V4, as well as QRS widening. These findings are consistent with hyperkalemia, which was promptly treated. Follow-up ECG post-treatment shows narrowing of the QRS complexes and normalization of peaked T waves.
Perilunate Dislocation
DOI: https://doi.org/10.21980/J8F59RIn the left lateral wrist x-ray, the lunate is dislocated from the rest of the wrist bones but still articulates with the radius. The capitate does not sit within the distal articulation of the lunate and is displaced dorsally. Additionally, a line drawn through the radius and lunate fails to intersect with the capitate. This is consistent with a perilunate dislocation. This is compared to a lunate dislocation, where the lunate itself is displaced and turned ventrally (spilled teacup) and the proximal aspect does not articulate with the radius.
Femoral Neck Fracture
DOI: https://doi.org/10.21980/J89G6GIn the anteroposterior view bilateral hip x-ray, there is an evident loss of Shenton’s line on the left when compared to the normal right, indicative of a fracture in the left femoral neck. This correlates with findings seen on pelvic CT, which reveals both a subcapital fracture and transcervical fracture. The neck of the femur is displaced superiorly relative to the head of the femur while the head of the femur remains in its anatomical position within the acetabulum.
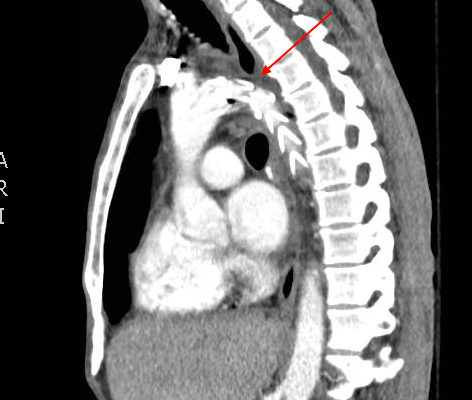
Traumatic Aortic Injury
DOI: https://doi.org/10.21980/J85P4JThe initial chest x-ray showed an abnormal superior mediastinal contour (blue line), suggestive of a possible aortic injury. The CT angiogram showed extensive circumferential irregularity and outpouching of the distal aortic arch (red arrows) compatible with aortic transection. In addition, there was a circumferential intramural hematoma, which extended through the descending aorta to the proximal infrarenal abdominal aorta (green arrow). There was also an extensive surrounding mediastinal hematoma extending around the descending aorta and supraaortic branches (purple arrows).
Wolff-Parkinson-White Syndrome: Electrocardiogram
DOI: https://doi.org/10.21980/J8201KThe initial EKG showed wide complex, irregular tachycardia > 200 bpm (EKG 1). Given the possibility of Wolff-Parkinson-White (WPW), procainamide was given to the patient. The patient’s heart rate responded and decreased to 120-140 bpm with narrowing of the QRS complex. A repeat EKG showed narrow complex tachycardia without P waves approximately 120 bpm (EKG 2). Once the procainamide infusion was complete, the patient had converted to sinus rhythm with a delta wave now apparent, consistent with WPW (EKG 3).
Posterior Elbow Dislocation
DOI: https://doi.org/10.21980/J8X593Elbow dislocations are classified by the position of the radio-ulnar joint relative to the humerus.1 Images 1, 2, and 3 show a left posterior elbow dislocation; the radius and ulna (red lines) are displaced posteriorly with respect to the distal humerus (blue line). The lateral view of the elbow most clearly shows this: trochlear notch of the ulna (red line) is empty and displaced posteriorly relative to the trochlea (blue line). There is no associated fracture. Images 4 and 5 show the elbow status-post reduction, demonstrating proper alignment of the distal humerus (blue line) with the radius and ulna (red lines).
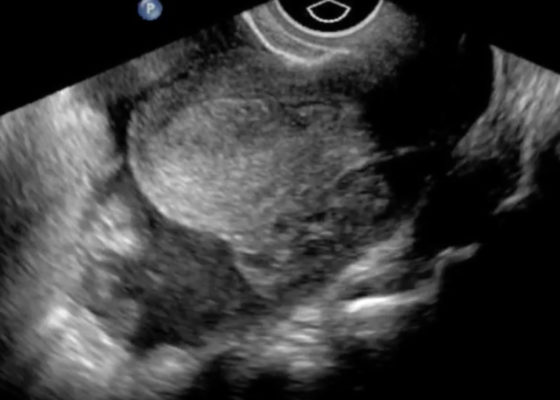
Ruptured Ectopic Pregnancy
DOI: https://doi.org/10.21980/J8SG6TThe patient’s serum beta-hCG was 5,637 mIU/mL. The transvaginal ultrasound showed an empty uterus with free fluid posteriorly in the pelvis and Pouch of Douglas (00:00). A 4.5 cm heterogeneous mass was visible in the left adnexa concerning for an ectopic pregnancy (00:10).