Issue 1:1
A Faculty Development Session or Resident as Teacher Session for Didactic and Clinical Teaching Techniques; Part 1 of 2: Engaging Learners with Effective Didactic Teaching
DOI: https://doi.org/10.21980/J8RP4TBy the end of this workshop, the learner will: 1) describe eight teaching techniques that encourage active learning during didactic sessions; 2) plan a didactic session using at least one of eight new teaching techniques for didactic instruction
A Faculty Development Session or Resident as Teacher Session for Clinical and Clinical Teaching Techniques; Part 2 of 2: Engaging Learners with Effective Clinical Teaching
DOI: https://doi.org/10.21980/J8MW2WBy the end of this workshop, the learner will: 1) describe and implement nine new clinical teaching techniques; 2) implement clinical teaching techniques specific to junior and senior resident learners.
Emergencies in Hemodialysis Patients
DOI: https://doi.org/10.21980/J81591By the end of this session, the learner will: 1) describe primary dialysis complications; 2) construct a full differential for a dialysis patient presenting with complications; 3) formulate an appropriate treatment and resuscitation in an acutely ill dialysis patient; 4) plan appropriate disposition and utilization of consultants for dialysis complications.
Approach to Acute Headache: A Flipped Classroom Module for Emergency Medicine Trainees
DOI: https://doi.org/10.21980/J8WC73At the end of this module, the learner will be able to: 1) list the diagnoses critical to the emergency physician that may present with headache; 2) identify key historical and examination findings that help differentiate primary (benign) from secondary (serious) causes of headache; 3) discuss the indications for diagnostic imaging, lumbar puncture and laboratory testing in patients with headache; 4) recognize life-threatening diagnoses on CT imaging and CSF examination; 5) describe treatment strategies to relieve headache symptoms.
Mesenteric Ischemia
DOI: https://doi.org/10.21980/J8CC7FAt the end of this simulation session, the learner will: 1) Recognize signs and symptoms of mesenteric ischemia; 2) order appropriately imaging and labs in the workup of an elderly patient with abdominal pain; 3) manage a patient with mesenteric ischemia, a rare, but serious cause of abdominal pain in the elderly; 4) discuss anchoring bias, specifically related to patients referred to the ED with an established diagnosis by outside specialists.
Atrial Myxoma
DOI: https://doi.org/10.21980/J87P45Bedside ultrasound revealed the presence of a left atrial mass that appeared to be tethered to the mitral valve. The mass was best viewed on ultrasound in the apical four-chamber window with the phased array probe placed over the patients’ point of maximal impact (PMI), with the patient in left lateral decubitus position.
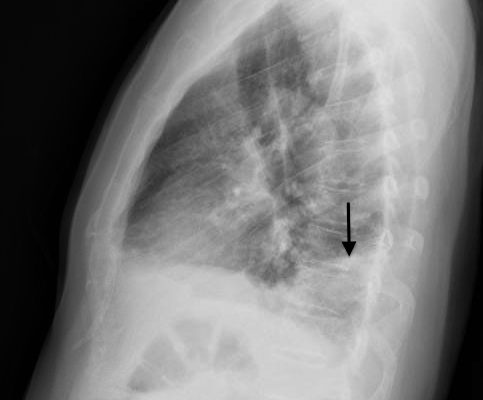
Hampton’s Hump in Pulmonary Embolism
DOI: https://doi.org/10.21980/J83W27In the lateral view chest x-ray, there is a Hampton’s Hump, a pleural based, wedge-shaped opacity at the base of the right lung, representing lung infarction (black arrow). These findings correlate with the sagittal view on CT angiography of the chest. The CT chest also shows a filling defect in the distal posterior basal segmental pulmonary artery (white arrow), as demonstrated by the absence of contrast enhancement in the distal portion of the vessel. This is associated with an opacification of the lung parenchyma distal to the occlusion (red arrow), representing lung infarction.
1›
Page 1 of 2