Issue 8:3
Everyday Water-Related Emergencies: A Didactic Course Expanding Wilderness Medicine Education
DOI: https://doi.org/10.5072/FK2HX1GX76By the end of the session, the learner will be able to: 1) describe the pathophysiology of drowning and shallow water drowning, 2) prevent water emergencies by listing water preparations and precautions to take prior to engaging in activities in and around water, 3) recognize a person at risk of drowning and determine the next best course of action, 4) demonstrate three different methods for in-water c-spine stabilization in the case of a possible cervical injury, 5) evaluate and treat a patient after submersion injury, 6) appropriately place a tourniquet for hemorrhage control, and 7) apply a splint to immobilize skeletal injury.
Alcohol Withdrawal with Delirium Tremens
DOI: https://doi.org/10.21980/J8S35NBy the end of the session, learner will be able to 1) discuss the causes of altered mental status, 2) utilize CIWA scoring system to quantify AW severity, 3) formulate appropriate treatment plan for AW by treating with benzodiazepine and escalating treatment appropriately, 4) treat electrolyte abnormalities by giving appropriate medications for hypokalemia and hypomagnesemia, and 5) discuss clinical progression and timing to AW.
Headache Over Heels: CT Negative Subarachnoid Hemorrhage
DOI: https://doi.org/10.21980/J8ND2CBy the end of this case, the participant will be able to: 1) construct a broad differential diagnosis for a patient presenting with syncope, 2) name the history and physical exam findings consistent with SAH, 3) identify SAH on computer tomography (CT) imaging, 4) identify the need for lumbar puncture (LP) to diagnose SAH when CT head is non-diagnostic > 6 hours after symptom onset, 5) correctly interpret cerebral fluid studies (CSF) to aid in the diagnosis of SAH, and 6) specify blood pressure goals in SAH and suggest appropriate medication management.
A Homemade, Cost-Effective, Realistic Pelvic Exam Model
DOI: https://doi.org/10.21980/J8HM0FAfter utilizing this pelvic examination model, the learner will be able to: 1) demonstrate ability to perform a pelvic examination comfortably and safely, 2) demonstrate ability to obtain a cervical swab on female patients, and 3) show proficient understanding of female anatomy.
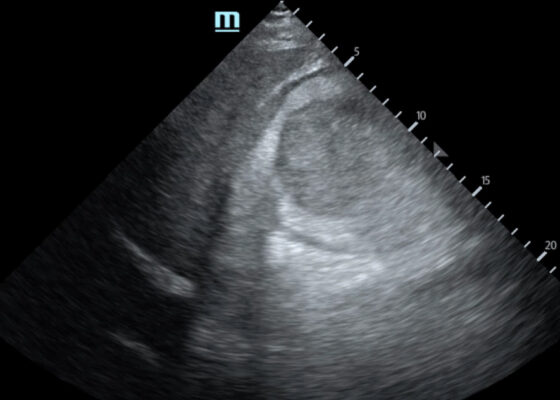
Trauma by Couch: A Case Report of a Massive Traumatic Retroperitoneal Hematoma
DOI: https://doi.org/10.21980/J84D2QUpon arrival at the trauma center, a FAST revealed a large, well-circumscribed abnormality (red outline) deep to the liver (blue outline and star) and gallbladder (green outline and star). The right kidney and hepatorenal space were not clearly visualized. The remainder of the FAST showed no free fluid in the splenorenal space, pelvis, and no pericardial effusion. He had lung sliding bilaterally.
A Case Report of Invasive Mucormycosis in a COVID-19 Positive and Newly-Diagnosed Diabetic Patient
DOI: https://doi.org/10.21980/J81M1GOn physical exam, when the patient was asked to try and look to her right, the right eye failed to move laterally/abduct (blue arrow). Additionally, when asked to look straight ahead, the eye was slightly adducted (red arrow). There was a lack of motion of the right eye in abduction when the patient was asked to look to her right (yellow arrow).
1›
Page 1 of 2