Latest Articles
The Eyes Have It: A Low-Cost Model for Corneal Foreign Body Removal Training
DOI: https://doi.org/10.21980/J82S85ABSTRACT: Audience: This corneal foreign body simulator is designed to instruct junior emergency medicine (EM) residents and medical students with an interest in emergency medicine. Introduction: Eye complaints are common in the emergency department (ED), accounting for approximately 2 million ED visits each year.1 Corneal foreign bodies (CFB) account for approximately 7.5% of these presentations, and many EM providers are
Pulseless Electrical Activity Cardiac Arrest
DOI: https://doi.org/10.21980/J8Z055After competing this simulation-based session, the learner will be able to: 1) Identify PEA arrest; 2) review the ACLS commonly recognized PEA arrest etiologies via the H &T mnemonic; 3) review and discuss the risks and benefits of tissue plasminogen activator (tPA) for massive PE.
Spinal Epidural Abscess
DOI: https://doi.org/10.21980/J8T938After this simulation case, learners will be able to diagnose and manage patients with spinal epidural abscesses. Specifically, learners will be able to: 1) Obtain a detailed history, including past infectious, surgical, procedural and social history to evaluate for epidural abscess risk factors; 2) describe clinical signs and symptoms of spinal epidural abscesses and understand that initial clinical presentations can be variable;
3) perform a focused neurological exam including evaluation of motor, sensory, reflexes, and rectal tone; 4) order appropriate laboratory testing and imaging modalities for spinal epidural abscess diagnosis, including a post-void bladder residual volume; 5) select appropriate antibiotics for empiric treatment of spinal epidural abscess depending on patient presentation; 6) disposition the patient to appropriate inpatient care.
Make and Break Your Own Hand: A Review of Hand Anatomy and Common Injuries
DOI: https://doi.org/10.21980/J8PH0ZBy the end of this session, learners should be able to name and identify all bones of the hand; arrange and construct an anatomically correct bony model of the hand; build functional phalangeal flexor and extensor tendon complexes onto a bony hand model; describe the mechanism of injury, exam findings, and management of the tendon injuries Jersey finger, Mallet finger, and central slip rupture; draw/recreate injury patterns on a bony hand model; and describe the mechanism of injury, exam findings, imaging findings, and management of scapholunate dissociation, perilunate dislocation and lunate dislocation, Bennett’s fracture, Rolando fracture, Boxer’s fracture and scaphoid.
A Comprehensive Course for Teaching Emergency Cricothyrotomy
DOI: https://doi.org/10.21980/J8JS9WAfter completing this activity, the learner will be able to: 1) correctly describe the indications for and contraindications to emergency cricothyrotomy; 2) correctly describe and identify on the simulator the anatomic landmarks involved in emergency cricothyrotomy; 3) correctly list the required equipment and the sequence of the steps for the “standard” and “minimalist” variations of the procedure; 4) demonstrate proper technique when performing a cricothyrotomy on the simulator without prompts or pauses.
Fracture Detectives: A Fracture Review Match Game
DOI: https://doi.org/10.21980/J8F06WAt the end of this session, learners will be able to: recognize and identify various orthopedic injuries on plain film images, describe the mechanism of injury of the various orthopedic injuries, describe the physical examination findings seen in various orthopedic injuries, recall associated injuries and at-risk anatomic structures associated with various orthopedic injuries, and describe the emergency department management of various orthopedic injuries.
Hemorrhagic Renal Cyst
DOI: https://doi.org/10.21980/J8C92VBedside renal ultrasound demonstrated a right renal cyst with echogenic debris consistent with a hemorrhagic cyst (red arrow). In addition, a computed tomography (CT) scan of the abdomen and pelvis revealed a 4mm non-obstructing right renal stone and bilateral renal cysts. The CT also confirmed the ultrasound finding of a right renal cyst with mild perinephric stranding possibly consistent with a hemorrhagic cyst.
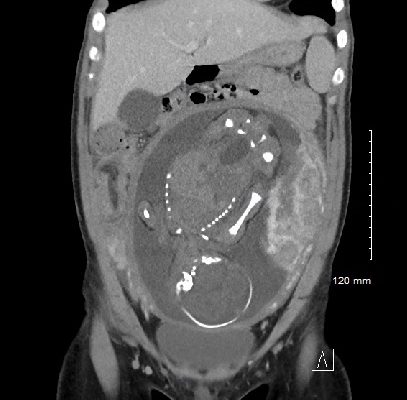
Meckel’s Diverticulum Causing Small Bowel Intussusception in Third Trimester Pregnancy
DOI: https://doi.org/10.21980/J87H19A CT scan was obtained which demonstrated distal small bowel intussusception with focal dilation suggestive of a small bowel obstruction in a pregnant female in her third trimester of pregnancy. The fetus can be seen in the uterus. The yellow arrow identifies the area of small bowel intussusception shown by telescoping intestines with associated bowel wall edema.
Bilateral Common Iliac Artery Aneurysm
DOI: https://doi.org/10.21980/J83S73A bedside ultrasound of the aorta was performed. The proximal, middle, and distal aorta appeared normal in caliber, as demonstrated by the images; however there seemed to be some enlargement at the bifurcation. The bifurcation into the iliac arteries, as highlighted by the yellow arrow, demonstrates a slightly enlarged iliac artery on the left. The aorta was followed below the bifurcation as it divided into the iliac arteries, as shown in the video clip. The ultrasound demonstrated a left iliac artery aneurysm measuring 5.99 cm, as highlighted by the orange circle. There were aneurysms to the bilateral common and internal iliac arteries.
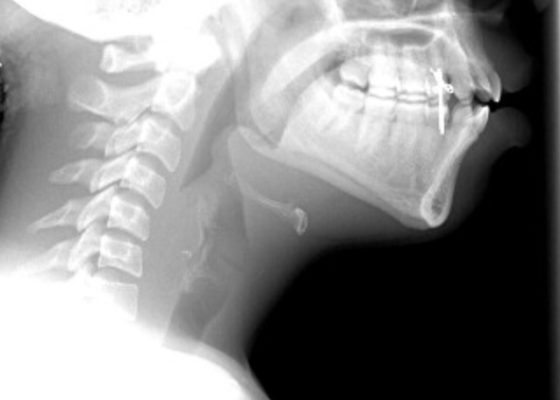
Case Report: Acute Supraglottitis
DOI: https://doi.org/10.21980/J8006VOn arrival, radiographs of the neck soft tissues were obtained, which showed a markedly enlarged epiglottic shadow (red arrow) concerning for epiglottitis. A computed tomography scan of the neck soft tissues with contrast was then obtained which revealed edematous mucosal thickening of the oropharynx (blue arrow) and supraglottic larynx (green arrow) including the epiglottis (purple arrow) concerning for acute infectious pharyngitis and supraglottic laryngitis with severe narrowing of the supraglottic laryngeal lumen, as well as associated extensive inflammation and edema of the superficial and deep left neck spaces. The patient’s white blood cell count was elevated to 25.7x109/L with 87% neutrophils. Her rapid strep test was positive. Otolaryngology was consulted and performed a bedside flexible laryngoscopy which showed significant edema of the epiglottis (orange arrow), vocal cords (white arrow), and arytenoids (black arrow), left greater than right. Based on the findings and concern for impending respiratory failure, the patient received an awake fiberoptic intubation by anesthesia at the bedside.