Procedures
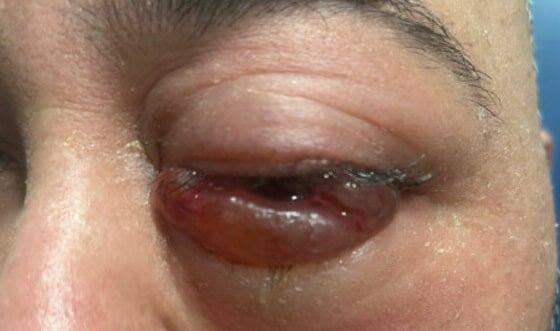
A Case Report of Carotid Cavernous Fistula: A Commonly Missed Diagnosis
DOI: https://doi.org/10.5070/M5.52242The initial physical exam performed by the ED provider revealed severe left eye chemosis, clear drainage, visual acuity of right eye 20/100 and left eye 20/400, and a left eye IOP of 52. There was a deficit of extraocular movement in all directions of gaze and limitation in all visual fields in the left eye. The MRI showed that at the level of the eye, the left cavernous sinus is asymmetrically enlarged compared to the right (red arrow) with an enlarged left inferior petrosal sinus with internal flow void on the pre-contrast MRI images (blue arrow). The orange arrow notes a central filling defect of the left superior ophthalmic vein on the MRA.
Procedural Case: Neonatal Lumbar Puncture
DOI: https://doi.org/10.21980/J8.52364This is a Procedure case involving a neonatal LP. The overarching educational goal of this case is to assess learners’ clinical decision-making, technical proficiency, and communication skills when performing a neonatal LP. Participants will be evaluated on their ability to identify indications and contraindications, obtain informed consent, prepare for and perform the procedure with sterile technique, and implement appropriate post-procedure care. By the end of the session, learners should be able to: 1) describe the indications and contraindications associated with performing a neonatal LP, 2) obtain informed consent for a neonatal LP, using clear, patient-centered language to explain the procedure and to discuss risks, benefits, and alternative options, 3) demonstrate proper preparation for a neonatal LP, including equipment setup, patient positioning, patient monitoring, use of sterile technique, and analgesia, 4) perform a neonatal LP on a procedural task trainer with technical proficiency, demonstrating proper needle insertion, cerebrospinal (CSF) collection, and adherence to sterile technique, and 5) outline appropriate post-procedure management for the patient, including interpreting CSF results, initiating appropriate treatment, monitoring for complications, and providing caregivers with clear follow-up guidance.
A Low-Cost Task Trainer Constructed from Silicone Nipple Covers
DOI: https://doi.org/10.21980/J8.52244Educational Objectives: By the end of this training session, learners will be able to anesthetize an abscess, perform incision and drainage, develop manual dexterity maneuvering instruments to break up the abscess, and place packing using both the linear incision and loop techniques.
Pizza and Paintballs: A Cost-Effective Model for Incision and Drainage Simulation Training
DOI: https://doi.org/10.21980/J8.52047Upon completing this lab session, the participant should have the capability to: 1) describe the indications, contraindications, and reasons for performing I&D of an abscess, 2) select the necessary equipment for performing I&D of an abscess, 3) demonstrate the necessary steps for performing
an I&D procedure on a simulated abscess.
Ultrasound Guided Peripheral Nerve Block Workshop: How to Take Your Residents from Zero to Hero
DOI: https://doi.org/10.21980/J8.52156After completing this small group workshop, the resident should be able to: 1) recognize the indications for the serratus anterior plane block, the posterior tibial block and the ulnar, median, and radial nerve blocks and the anatomical locations that would benefit from these blocks, 2) identify proper probe selection and placement, in addition to patient positioning, in order to perform these blocks, as well as anesthetic choice and dosing, 3) demonstrate knowledge of anatomical landmarks and areas to avoid evidenced by probe placement and positioning, 4) describe the steps to perform these nerve blocks, and 5) demonstrate knowledge of contraindications to these blocks as well as potential complications of these procedures and how to mitigate them.
Troubleshooting the Trach: Emergent Tracheostomy & Laryngectomies Modified Team-Based Learning Activity
DOI: https://doi.org/10.21980/J8.52033By the end of the session, participants will be able to: identify the major anatomy of tracheostomies and laryngectomies, 2) demonstrate step-by-step management of emergent tracheostomy airways, 3) describe common complications of tracheostomies, 4) understand the management of tracheal innominate artery complication.
Innovative Ultrasound-Guided Erector Spinae Plane Nerve Block Model for Training Emergency Medicine Physicians
DOI: https://doi.org/10.21980/J8PW7DThis innovation model is designed to facilitate hands-on training of the ultrasound-guided ESP nerve block using a practical, realistic, and cost-effective ballistics gel model. By the end of this training session, learners should be able to: 1) identify relevant sonoanatomy on the created simulation model; 2) demonstrate proper in-plane technique; and 3) successfully replicate the procedure on a different target on the created training model.
Orthopaedic Surgery Didactic Session Improves Confidence in Distal Radius Fracture Management by Emergency Medicine Residents
DOI: https://doi.org/10.21980/J8K365By the end of this didactic session, learners should be able to: 1) assess DRF displacement on pre-reduction radiography and formulate reduction strategies, 2) perform a closed reduction of a DRF, 3) apply a safe and appropriate plaster splint to patient with a DRF and assess the patient’s neurovascular status, 4) assess DRF post-reduction radiography for relative fracture alignment, and 5) understand appropriate follow-up and necessary return precautions.